In this article:
Home remedies help prevent flare-ups and manage symptoms by providing relief from dry skin and inhibiting lesion formation and bleeding. However, bear in mind that these remedies cannot be used as a cure for psoriasis.
Note: Use herbal remedies only after consulting your doctor. Avoid using herbal or home remedies if you are breastfeeding, pregnant, diabetic, have high blood pressure, or are on medications. Discontinue the treatment if you experience any side effects and seek immediate medical consultation.
Home Remedies for Psoriasis
Here are a few remedies to ease psoriasis symptoms:
1. Apply a cold compress
A cold compress can provide temporary relief from itching and can decrease swelling. These occur due to the numbing and distraction effect of the cold temperature.
If performed carefully, a cold compress can be a safe and effective treatment for skin problems that cause itching, such as psoriasis.
How to use:
Wrap ice cubes in a clean washcloth and lightly press the compress against the affected areas for 10 minutes. Repeat this method several times a day.
Note: Avoid direct application of ice to the skin as it can cause frostbite. Discontinue the compress if stinging or burning occurs.
Topical application of cold temperatures can desensitize the nerve endings in that area and thus reduce the perception of itching and skin discomfort caused by psoriasis.
2. Take an oatmeal bath
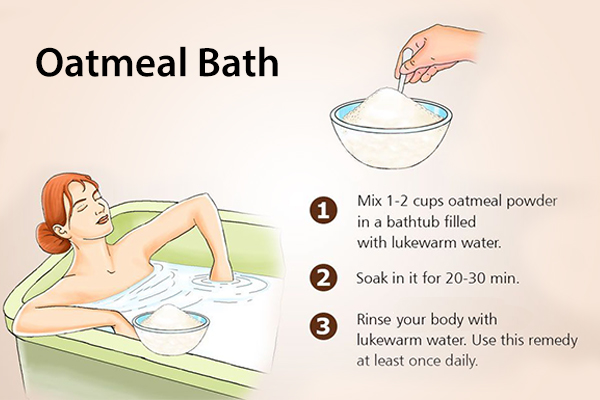
Soaking your skin in colloidal oatmeal is helpful in treating various skin conditions, including eczema, psoriasis, and dry skin. Colloidal oatmeal is made by suspending powdered oats in liquids such as milk, water, or gel.
A 2018 study found colloidal oatmeal-based skin care products to be useful in the treatment of dry skin conditions like psoriasis, in terms of hydrating the skin and improving its overall appearance. (1)(2)
How to use:
- Fill the bathtub with warm water and add in 1 cup of finely ground oatmeal.
- Stay in the colloidal bath for about 20 minutes and then wash with lukewarm water.
- Pat your skin dry and apply a moisturizer.
- Repeat daily during flare-ups.
Note: Oatmeal baths should not be used as the only treatment. It is advised to seek medical help, especially if the symptoms worsen or do not subside.
Colloidal oatmeal is a safe and natural product that has been found highly effective in the management of several dermatological conditions, such as drug-induced rash, dermatitis, psoriasis, among others.
3. Use glycerin on the lesions
Glycerin helps in healing the skin by stimulating cell growth. Moreover, its skin hydrating effect is similar to that of hyaluronic acid (HA), which is one of the best skin moisturizers there is. Thus, glycerin can fare very well in the treatment of dry skin conditions like psoriasis, which has been corroborated by several studies. (3)(4)
How to use:
Apply generous amounts of glycerin to the affected areas and allow it to be absorbed by the skin.
Note: Aloe vera gel or natural plant-derived aloe vera can be used in place of glycerin.
Glycerin can deeply hydrate the skin, enhance its barrier function, and help alleviate psoriasis symptoms like skin dryness, thick leathery patches, as well as erythema or redness.
4. Heal your skin with turmeric gel

Several scientific studies demonstrated that turmeric helps inhibit the action of several inflammatory enzymes involved in psoriasis flare-ups. Thus, these studies favored the topical and oral use of turmeric derivatives as an alternative therapy for treating plaque psoriasis. (5)(6)
How to use:
- Apply turmeric gel to the affected areas. You can also mix turmeric powder and water to form a paste for application. Leave the gel or paste overnight and wash it off with warm water the morning after.
- Turmeric or curcumin supplementation may also be beneficial for psoriasis involving both the skin and joints.
Note: Avoid the ingestion of turmeric if you have gallbladder problems. If you have any blood clotting issues or take medicines for diabetes, get your doctor’s permission before using this herbal remedy.
Turmeric acts as an anti-inflammatory agent that can help curb psoriasis-induced skin discomfort when used orally or topically.
5. Moisturize your skin with olive oil
A 2018 study demonstrated the use of olive oil for the treatment of psoriasis. It was found out that the polyphenols present in extra-virgin olive oil act as anti-inflammatory and antioxidant agents, which help in managing immune disorders such as psoriasis.
The use of a cream formulated with plant-based extracts, black cumin oil, and olive oil on skin lesions for 12 weeks helped in alleviating psoriasis. (7)
How to use:
- Heat olive oil to lukewarm temperature and apply it to the affected areas to provide hydration.
- Alternatively, combine 1 teaspoon each of olive oil, honey, and beeswax and use this lotion.
Oleic acid (a monounsaturated fatty acid), oleuropein, and vitamin E provide physiological functions to olive oil, making it an important anti-inflammatory and antioxidant agent that can help relieve psoriasis symptoms.
6. Apply aloe vera

Aloe vera oil/gel can be applied to psoriasis lesions to reduce the discomfort and promote healing. This topical remedy can help moisturize the dry, irritated skin while also exhibiting significant antimicrobial and skin repair benefits.
Some studies have highlighted the positive role of aloe vera in healing psoriasis, but further research is needed to confirm just how effective it is. (8)(9)
Note: Although aloe vera is considerably mild and safe for application, you must still exercise caution since psoriasis can make your skin ultra-sensitive. Always conduct a patch test before the full-fledged application of any such topical agent.
Topical use of aloe vera for psoriasis can impart some much-needed moisture to the dry patches, strengthen the skin barrier, prevent infections due to its antiseptic potential, soothe the itch and redness by curbing inflammation, and remove scaling.
7. Consider licorice root
Licorice is commonly used for the treatment of psoriasis in the Chinese medicine system or as an anecdotal remedy, but not so much in modern clinical practice. Thus, you will have to check with your doctor before consuming this plant medicinally for the appropriate dosage.
Licorice root contains an active compound known as glycyrrhizin, which helps in subsiding irritation, redness, and inflammation caused by psoriasis.
8. Massage your scalp with apple cider vinegar
Apple cider vinegar is yet another popular remedy for psoriasis relief, but it lacks any kind of scientific support, which is why you must be careful while using it.
It is believed that organic ACV can help normalize the skin pH and bring down underlying inflammation to relieve the psoriasis itch, especially in the scalp.
How to use:
- Mix equal parts of organic ACV and water and then apply this solution on your scalp several times a week.
- Rinse the scalp thoroughly once the solution has dried up.
Caution: Although ACV is basically alkaline, but it can prove too harsh for your already irritated and sensitive skin. You must always dilute the liquid with water, and then patch test it on a small area before applying it all over your psoriasis patches.
Discontinue its use if you experience significant burning or any kind of irritation. Never apply ACV on open wounds as well as cracked or bleeding skin.
9. Dip your skin in an Epsom salt bath

Taking an Epsom salt bath can help soothe the itching and skin discomfort associated with psoriasis, while the warmth of the water can help soften and exfoliate the flaky patches.
This simple home therapy has provided a lot of relief to many users, but is devoid of any scientific backing.
How to use:
- Add 1–2 cups of Epsom salt per gallon of your warm bathwater and soak your body in it for about 15 minutes.
- Apply a hydrating lotion all over your body right after bathing, while the skin is still damp to seal in the moisture.
10. Get more of omega 3 and vitamin D
Omega 3 and vitamin D are also cited on internet forums and other platforms as complementary aids for relieving psoriasis symptoms, but there is little to no research backing such claims. Thus, it is vital that you consult your doctor before starting any supplement, no matter how popular it is. (10)
For instance, people have reported good results after taking fish oil supplements, which is rich in omega-3 fatty acids that can help reduce inflammation, ward off infections, while also hydrating the skin and scalp.
Directions:
- Your first attempt should be to meet your omega 3 requirement through food sources such as weekly servings of fatty fish or eggs, and supplements should only be considered when dietary intake is not enough. (11) The topical use of vitamin D ointments is a well-recognized treatment modality for psoriasis, but the role of oral supplementation is not well understood. Psoriasis triggers the growth of excess skin cells, which form lesions, but vitamin D application can help slow down this cell proliferation. So, you may also benefit from the dietary intake of this nutrient, especially if you are deficient.
- Eat foods such as milk and cereals fortified with vitamin D, fish, eggs, yogurt, orange juice, but in recommended amounts.
- You should spend time in the sun to stimulate the natural production of vitamin D in the skin and opt for supplements if you fail to get your required dosage through other means. Always consult your doctor before starting the supplement.
11. Treat psoriasis with tea tree oil
Tea tree oil is considered a panacea for your skin, which works as an effective antibacterial, antiseptic, and anti-inflammatory agent. All these properties can help in treating a variety of skin conditions, such as acne, eczema, and even psoriasis.
Regular application can help bring down the swelling, redness, and irritation while also preventing the growth of bacteria in the psoriasis patches. This skin healing oil is also known to remove dead skin cells and hydrate the skin.
This remedy has a lot of anecdotal support, but not enough scientific backing. Thus, it is recommended that you consult your dermatologist before trying it. (12)(13)
Caution: However, like all essential oils, tea tree oil is very strong in concentrated amounts and must be diluted in a carrier oil before application. Also, you must patch test the oil on a small area of the skin to rule out any adverse reactions.
Alternative Therapies
You can try this specialized technique as an adjunct to your main treatment, but only under the supervision of a trained expert.
Give acupuncture a try
Acupuncture is an ancient Chinese technique wherein needles are inserted at specific points of the body to relieve inflammation, promote blood circulation, stimulate immune function, and address various other sources of illness.
This alternative therapy is mildly invasive and must be performed by a trained acupuncturist. It has been successfully used for the management of psoriasis and has sometimes fared better than some of the most common Western medications prescribed for this condition. (14)(15)
Preventive Self-Care to Avoid Flare-Ups

Taking a few precautionary steps can help to manage the symptoms of psoriasis and improve the cosmetic look of the skin. The following tips may be helpful:
- Shower daily and avoid scrubbing your skin to prevent irritation.
- Cleanse private areas daily, shower every other day, or take a very quick shower only using a cleanser on the private areas.
- Prefer using a mild soap or body wash over a harsh bar soap to avoid drying of the skin.
- Do not use hot water for bathing as it can aggravate the condition. Use lukewarm water in the shower or bath and limit bathing to 20 minutes or less.
- Spending some time in the sun over a couple of days may help subside the psoriasis symptoms mildly, but prolonged exposure at a stretch can lead to sunburn. Subsequently, a new plaque of psoriasis may develop on the damaged skin.
- Practice relaxation techniques to manage stress.
- Use humidifiers to maintain the moisture level indoors.
- Ask your doctor about the foods you need to avoid to prevent a flare-up. High-glycemic foods, excess sugar, and processed foods can contribute to insulin resistance and inflammation in the body, which may worsen psoriasis.
- Do not scratch or pick at the lesions.
- Wear soft cotton and linen materials.
- Avoid the use of possible irritants such as perfumes and dyes.
- Decrease alcohol intake as it can render your treatment ineffective.
- Apply the medications as directed by your dermatologist until the symptoms improve.
Most-Asked Questions About Psoriasis
Is psoriasis contagious?
Because psoriasis does not develop due to an infection, it is not contagious.
Does psoriasis increase the risk of cancer?
Having psoriasis can predispose you to cancer due to the chronic inflammation associated with the disease. The risk of developing cancer also increases with the use of UV light and immune-suppressive medications for therapy.
An increase in the prevalence of factors such as obesity and smoking that are well-known factors for carcinogenesis also contributes to the development of cancer in patients who have psoriasis. (16)
How does diet affect psoriasis?
Psoriasis is a chronic problem that causes prolonged inflammation. Therefore, it is essential to lead a healthy lifestyle and include anti-inflammatory foods in a well-balanced diet while limiting your intake of inflammatory foods like dairy, red meat, gluten, refined sugar, and processed foods.
A review paper published in 2019 concluded that though dietary modifications may not help in treating psoriasis, they are required as an adjunct to first-line treatments. (17)
Does pregnancy affect psoriasis?
Psoriasis does not have any effect on fertility or pregnancy. However, some women find improvement in their psoriasis during pregnancy, while some others feel that the condition worsens.
Psoriasis treatment may harm the baby; thus, consultation with a doctor is recommended.
Are psoriasis and eczema similar?
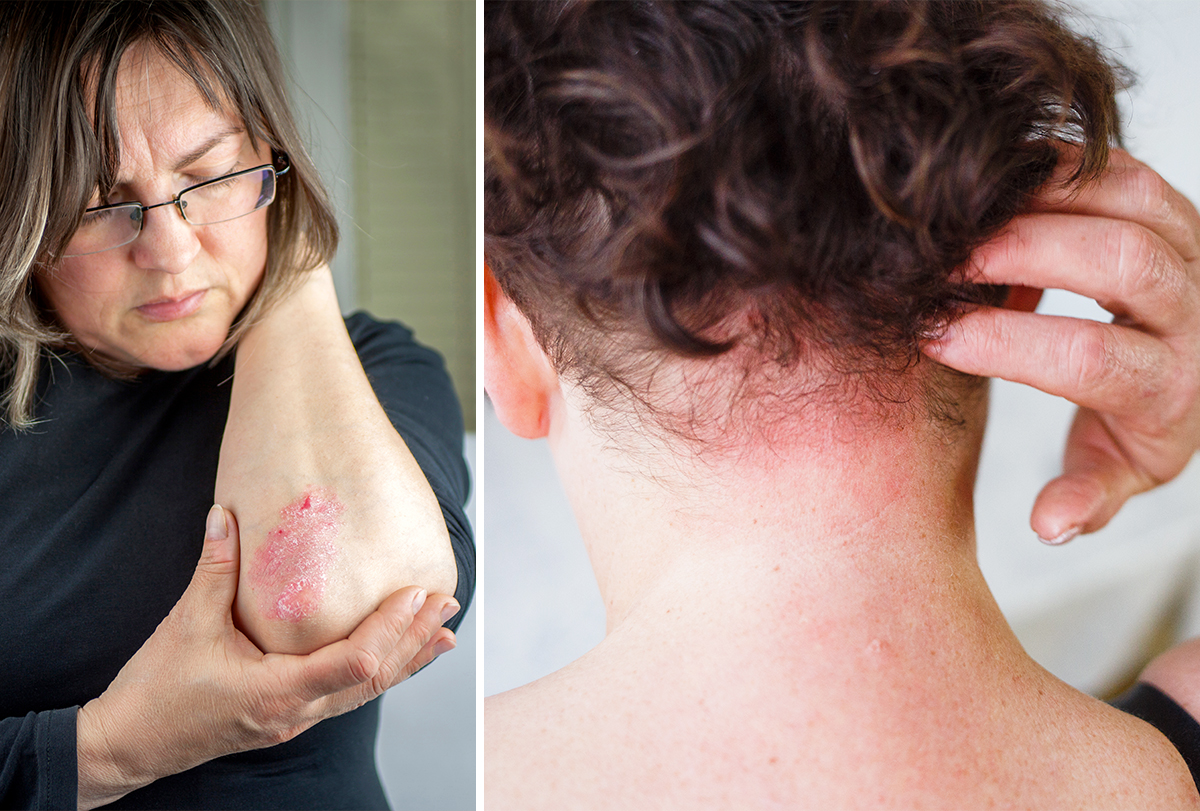
Psoriasis and eczema have a similar appearance, but an experienced dermatologist can distinguish between the two using features such as the flakiness of the skin in eczema and the buildup of silvery scales in psoriasis.
Similarity: Both psoriasis and eczema cause a rash (patches of inflamed, red, and itchy skin) on the same body parts, such as the scalp and the hands. While these skin conditions are non-contagious, they may lead to infections.
Difference: Psoriasis occurs due to the overactivity of an individual’s immune system, speeding up the growth of cells. On the other hand, eczema is usually triggered by an allergy, skin barrier dysfunction, environmental issues, bacterial infection, among other contributing factors.
Are coal tar products beneficial for the treatment of psoriasis?
Yes, coal tar products have helped in clearing stubborn psoriasis patches on the palms and soles of many patients when used along with standard topical corticosteroids. (18)(19)
They have also delivered good results in terms of alleviating scalp psoriasis and increasing its remission.
But the success rate of coal tar products for treating psoriasis varies from patient to patient. Thus, it is essential that you speak to your dermatologist to find out if this treatment is suitable for you and to seek the ideal product recommendation.
Final Word
While psoriasis cannot be completely cured, it can be managed with the help of the recommended treatments. Flare-ups can be prevented by taking measures to avoid triggers.
Additionally, you can take the help of natural home remedies to alleviate the symptoms. It is vital to moisturize your skin to prevent irritation and discomfort.

- Was this article helpful?
- YES, THANKS!NOT REALLY



