In this article:
Millions of people suffer from diabetes. According to the World Health Organization, the number of people with diabetes has risen from 108 million in 1980 to 422 million in 2014. WHO also projects that diabetes will figure as the seventh leading cause of death by the year 2030. (1)

Diabetes is considered a deadly disease. If not controlled, high blood sugar can affect different body parts and can lead to serious complications like diabetic neuropathy.
Diabetic neuropathy is the result of nerve damage caused by the toxic effects of high blood sugar levels and poor blood circulation. In fact, a consistently high blood sugar level can cause damage to the peripheral nerves that are responsible for communicating messages between the brain or spinal cord and the rest of the body.
As a consequence of this progressive form of nerve damage, you may experience a gradual loss of sensation as well as pain and weakness in the areas affected, typically the feet and sometimes the hands as well.
Prevalence of Diabetic Neuropathy
Nearly 60% of all diabetes patients suffer from some form of nerve damage.
A 2010 study by the American Family Physician reports that diabetic peripheral neuropathic pain affects the functionality, mood, and sleep patterns of approximately 10% to 20% of patients with diabetes mellitus. (2)
Types of Diabetic Neuropathy
There are basically four types of diabetic neuropathies:
1. Peripheral neuropathy
Peripheral neuropathy refers to the condition wherein the nerves that connect the brain/spinal cord to the skin, muscles, and internal organs start to malfunction due to progressive damage. As a result, the intricate communication system that spans between the central nervous system and the rest of the body gets disrupted.
The repercussions of this type of neuropathy are typically felt in the feet and legs and occasionally affect the hands and arms as well. About one-third to one-half of people with diabetes report symptoms associated with this kind of nerve damage, indicating its striking prevalence.
2. Proximal neuropathy
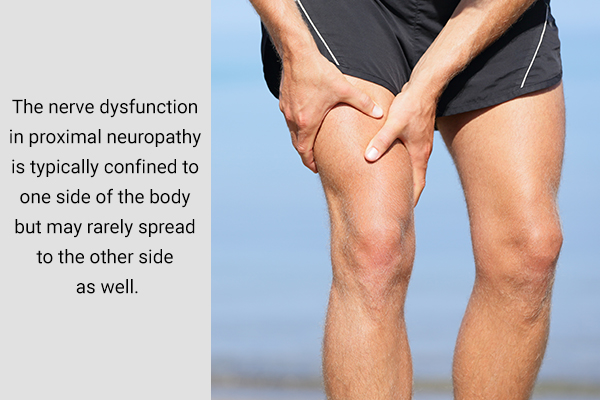
Proximal neuropathy is the second most common form of diabetic nerve damage that affects one’s movement, figuring after peripheral neuropathy. This rare type of motor dysfunction can exhibit mild to disabling symptoms, which include muscle weakness and decreased sensation and pain in the hip, buttock, or thigh.
The nerve dysfunction is typically confined to one side of the body but may rarely spread to the other side as well. The symptoms associated with proximal neuropathy gradually improve over a period of months or years.
3. Autonomic neuropathy
As the name suggests, autonomic neuropathy affects the autonomic nervous system. It involves damage caused to the sympathetic and parasympathetic autonomic nerves that control the involuntary and nonsensory body functions.
This form of neuropathy affects the internal organs and can give rise to various problematic issues pertaining to the heart rate and blood pressure, digestive system, bladder control, sex organs, sweat glands, and eyes.
Another worrisome disadvantage of autonomic neuropathy is that the body fails to pick up on the warning signs of hypoglycemia, which can be especially life-threatening for a patient with diabetes.
4. Focal neuropathy

Focal neuropathy is characterized by damage to a single nerve outside of the central nervous system and is usually caused by some kind of trauma, injury, or compression.
This form of mononeuropathy is relatively less common than peripheral and autonomic neuropathy and typically affects specific nerves located in the hand, head, torso, or leg. More rarely, it can affect a nerve in the back or the chest as well as one that controls eye muscles.
The symptoms associated with focal neuropathy tend to appear abruptly but resolve on their own, without causing any long-term damage.
The most well-known manifestations of focal neuropathy are entrapment syndromes, such as carpal tunnel syndrome wherein the median nerve becomes compressed when it passes through a small tunnel located in the wrist.
What Causes Diabetic Neuropathy?

Diabetic neuropathy is by and large the result of a prolonged struggle with diabetes. Chiefly rooted in the sustained levels of high blood sugar, the nerve damage tends to get aggravated when your diabetes is not properly managed over a long period of time.
Other contributing factors for diabetic neuropathy include:
- Elevated cholesterol levels that cause damage to the blood vessels
- Physical damage to the nerves in the form of mechanical injury or compression as well as due to surgery
- Unfavorable lifestyle choices, such as excessive smoking or alcohol consumption
Such neuropathy can also be traced back to a deficiency of vitamin B12, which is made worse by Metformin, a common medication used to manage diabetes. Your healthcare provider can rule out any such vitamin deficiencies by conducting a simple blood test.
Symptoms of Diabetic Neuropathy

Diabetic neuropathy may exhibit varying symptoms depending upon the specific type of neuropathy and the nerves affected. At their onset, the symptoms associated with different forms of diabetic neuropathy are generally mild and minor and often tend to go undetected. In fact, some people experience no symptoms at all.
As the neuropathy gets progressively worse with more and more nerve fibers affected over time, the symptoms become more pronounced. What may start off as numbness, tingling, or pain in the feet can escalate to a more serious extent and result in a sensory loss, coordination difficulties, and even motor (movement) problems.
Diabetic neuropathy initially affects the peripheral nerves, and the damage is first felt in the extremities, particularly the feet. As you continue to grapple with diabetes over the course of several years, the resultant damage to the nerves gradually progresses more centrally and can end up affecting the involuntary (autonomic) nervous system as well.
Some of the common symptoms of diabetic nerve damage include:
- Numbness, tingling, prickling pain, or altered sensation in the toes, feet, legs, hands, arms, and fingers
- Pain in the legs, hips, and thighs
- Thinning or wasting of the muscles in the affected region
- Impaired movement due to difficulty in lifting the front part of the foot and toes, known as foot drop
- Twitching and muscle cramps
- Difficulty in focusing your eyes, sometimes resulting in double vision
- Indigestion, nausea, or vomiting
- Diarrhea or constipation, particularly at night
- Bloating or belching
- Dizziness or faintness on standing due to sudden plunges in blood pressure
- Problems with urination, such as trouble starting urination, failing to sense a full bladder, and inability to empty the bladder completely
- Erectile dysfunction (impotence) or ejaculation problems in men
- Vaginal dryness, low sex drive, and difficulty reaching orgasm in women
- Muscle weakness or paralysis affecting one or several muscles
- Weight loss
- Abnormal perspiration patterns, which include sweating too much or too little and, consequently, improper regulation of body temperature
- Swelling in the abdomen
- Hypoglycemia (low blood sugar) unawareness, a condition in which the body fails to recognize the symptoms of hypoglycemia
Treatment for Diabetic Nerve Pain
Treatment for diabetic nerve pain primarily aims to delay or control the degeneration of blood vessels and nerves brought on by high blood sugar. Secondly, it aims to reduce the severity of your symptomatic discomfort.
Bringing down your blood sugar within normal range is perhaps the most important prerequisite for any treatment strategy to yield positive results.
Your doctor will consider all the necessary health markers before laying down an overarching course of treatment to achieve and maintain proper glycemic control through diet, exercise, and medications.
The doctor may also recommend soothing baths and prescribe certain analgesics, antidepressants, and anticonvulsants to alleviate the pain and discomfort associated with diabetic neuropathy.
Diagnosing Diabetic Nerve Pain

For the preliminary diagnosis of diabetic neuropathy, your doctor will take into account your symptoms and medical history. Thereafter, you will have to go through a physical examination before the doctor can give you his/her clinical verdict.
This presumptive diagnosis will then be backed up by a number of definitive tests specifically designed to estimate the loss of nerve function.
For instance, nerve conduction studies aim at measuring the speed of nerve signals in the arms and legs, and electromyography assesses the electrical discharges produced in the muscles. In the same vein, your doctor may feel the need to conduct a few additional tests of nervous system function to reach a more conclusive diagnosis. A clinical examination may identify early signs of neuropathy in diabetics without symptoms. (3)
Risk Factors Associated With Nerve Pain
The threat of diabetic nerve damage becomes more and more imminent with time and the symptoms become more noticeable as the disease progresses. Thus, someone who has grappled with diabetes for years is likely to be at a much greater risk than those at relatively nascent stages of the disease.
Moreover, the poorer your glycemic control, the more likely you are to develop diabetic neuropathy.
Other factors that make one increasingly vulnerable to diabetic nerve damage include:
- People with high blood pressure
- People who are overweight or obese
- People above the age of 40
- People who smoke
- People of African or Native American descent
- People experiencing complications of their diabetes elsewhere in their body such as in the kidneys, heart, and eyes
Complications Associated With Diabetic Neuropathy
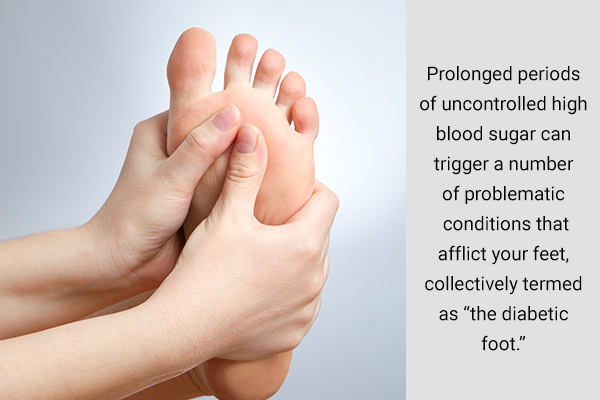
The typical problem areas associated with diabetic neuropathy are the peripheral regions or extremities, which include your feet, legs, hands, and arms. However, even among these commonly identified neuropathic sites, your feet tend to bear the greatest brunt of diabetic nerve damage.
Prolonged periods of uncontrolled high blood sugar can trigger a number of problematic conditions that afflict your feet, collectively termed as “the diabetic foot.”
People with diabetes are increasingly prone to burning, tingling, or stabbing pain in the feet. This kind of neuropathic foot pain can occur simultaneously along with feelings of numbness and gradually give way to a loss of feeling or sensation in the feet. It is on account of this reduced sensitivity that people with diabetes may not feel any pain or irritation arising from foot wounds or injuries.
Due to this hampered sensitivity, diabetes patients tend to remain unaware of foot injuries which go untreated for a long time. This negligence can take an ugly turn, as your injured foot might become infected and develop ulcers and gangrene. (4)
Once the situation goes out of hand, the doctor might have to resort to surgical treatments for the redressal of podiatric complications, such as surgical removal of dead or decaying tissue as well as partial or complete amputation of the foot.
To avoid such complications, people with diabetes are advised to regularly examine their feet for any sign of injury or infection. Plus, they should visit their podiatrist at least once a year for a more thorough check up that could help diagnose new problems related to diabetic neuropathy.
This includes underlying circulation problems along with identifying other signs of trouble, such as wounds, blisters, and a joint disorder known as Charcot arthropathy or Charcot’s foot.
When to See a Doctor
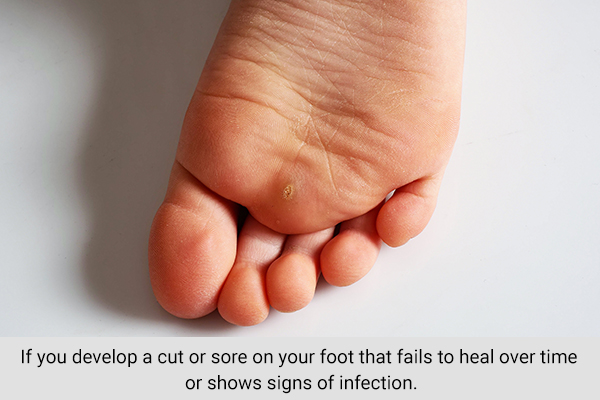
The following red flags should alert you to get immediate medical help:
- If you develop a cut or sore on your foot that fails to heal overtime or shows signs of infection
- If you experience burning, tingling, weakness, or pain in your hands or feet that end up disrupting your daily activities or sleep
- If you notice unusual changes in digestion, urination, or sexual function
- If you experience dizziness
Final Word
Diabetic neuropathy is a common complication of prolonged or poorly controlled diabetes which gets progressively worse if left untreated.
The first step towards controlling this form of nerve damage is to control your blood sugar levels such that they remain within the healthy range. This has to be achieved through medication, diet, exercise, and an overall healthy lifestyle. How well any of the treatments for diabetic neuropathy will fare depends on how well managed your diabetes is.
In fact, as many as 60% of people with type 1 diabetes have managed to stave off diabetic neuropathy simply by maintaining strict control over their blood sugar levels.

- Was this article helpful?
- YES, THANKS!NOT REALLY



