In this article:
When it comes to pain, people can be afflicted by several kinds.
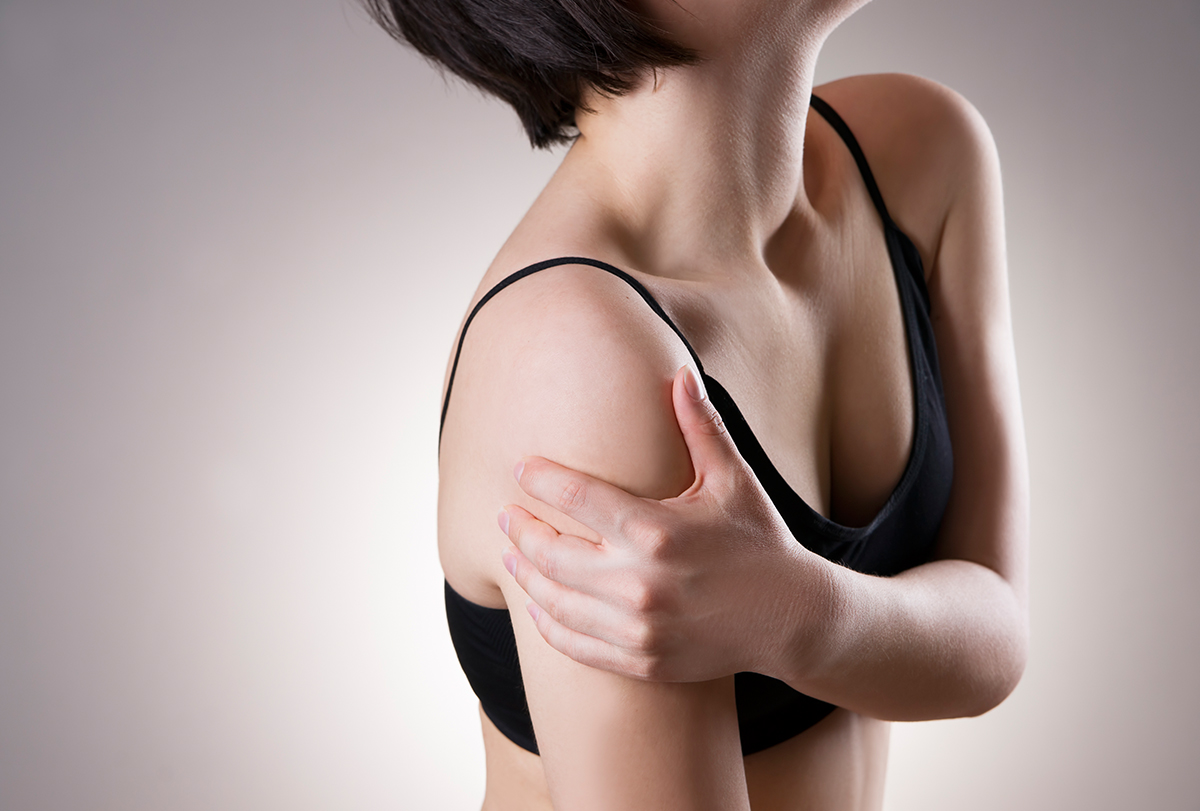
Broadly speaking, there is neuropathic pain of the peripheral nerves and central nervous system, which feels like numbness, tingling, stabbing, or burning and radiates along the nerve distribution.
The other kind of pain is nociceptive pain, which feels more like a dull, deep, waxing, and waning pain that is localized to an area and is exacerbated with a sharp pain feeling with movement or touch and alleviated by rest.
Musculoskeletal (MSK) pain is a form of nociceptive pain that relates to pain within the bones, joints, connective tissue/soft tissue, muscles, tendons, and ligaments. (1)
MSK pain can be acute, meaning it has occurred within the last 2 weeks and is sudden and severe such as after a fracture. It can be chronic, meaning it has been ongoing for more than 2 weeks and is slowly progressive and long-lasting, such as in osteoarthritis.
What Areas of Pain Are Considered Under Musculoskeletal Pain?
MSK pain within the bone can occur after fractures, splints, or less commonly bone tumors.
More often, however, MSK pain presents within high-impact joints such as the knees, thumbs, big toes, and vertebrae in the form of strains, spasms, cramps, and tears.
Lastly, tendon, ligament, and soft tissue/connective tissue MSK pain secondary to strains, sprains, tears, and inflammation can occur with overuse and injury. (2)
What Are the Common Causes of Musculoskeletal Pain?
The most common causes of MSK pain are tissue damage from everyday wear and tear, overuse injuries, excessive exercise, age-related degenerative damage, awkward positions, and trauma. (3)
A whole array of medical conditions can also cause MSK pain such as fibromyalgia, arthritis (osteo, rheumatoid, septic), tendinitis, bursitis, rotator cuff tears, meniscal tears, myositis, gout, and fractures.
What Are the Signs and Symptoms of Musculoskeletal Pain?

As described above, MSK pain feels like a dull, deep, aching, waxing, and waning pain that is localized to an area of the body and is exacerbated with a sharp stab feeling with movement or touch. It is usually alleviated by rest and anti-inflammatories. (4)
Furthermore, there may be stiffness, swelling, and restricted range of motion after activity and during flare-ups of this pain. Tight muscle knots may be noted as well as muscle spasms and twitching.
Muscle weakness, poor posture, and sleep disturbance due to pain may occur in more severe cases. In case of fractures, bruising is usually seen. In case of ligament issues, joint instability is common.
For tendon or bursa issues, the motion that activates that tendon or the area over the bursa will cause soreness and tenderness.
What Is the Best Treatment Plan for Musculoskeletal Pain?
Once diagnosed, benign, non-inflammatory, noncrystal, and noninfectious MSK pain can be treated using a graduated approach from least invasive to most invasive treatment. (5)
Initially, the intervention will start with rest, icing, elevation, compressing the area, and avoiding any triggering activities. (6) Stretching, massaging, and nonpainful range of motion exercises follow suit.
During this time, patients may try nonsteroidal anti-inflammatory drugs (NSAIDs) both orally and topically or Tylenol to reduce the inflammation and dull the pain, thus allowing you to participate in the above light exercising, stretching, and massaging along with allowing you to get through the day. (7)
Muscle relaxants can be trialed at this time too. If these fail, then a formal course of physiotherapy, chiropractic, and acupuncture may be needed.
If a good trial of the above therapies for approximately 3 months fails, then a trial of cortisone, hyaluronic acid, or plasma-rich platelets (PRP) injected straight into the joint can be done. Similarly, lidocaine, saline, PRP, or prolotherapy can be injected straight into the problematic area.
Beyond that point, other prescription drugs such as duloxetine and/or opioids or surgery can be the next step.
How Is Musculoskeletal Pain Diagnosed?
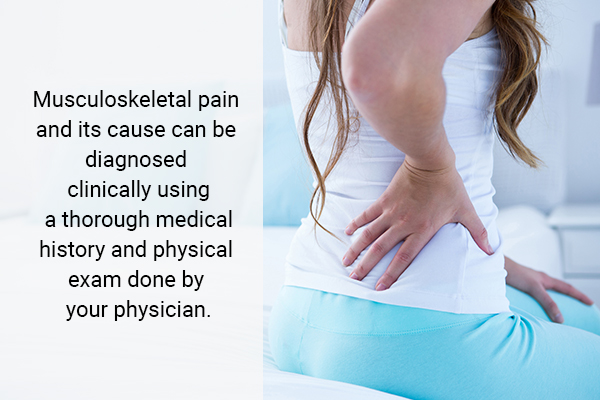
MSK pain and its cause can be diagnosed clinically using a thorough medical history and physical exam done by your physician.
Your doctor will also utilize specific bedside tests to aid in the diagnosis such as the Neer and painful arch tests, the Hawkins test, rotator cuff specialized tests, apprehension tests, the drawer test, leg and cross raises, and the McMurry test.
These details will aid your physician in either making a diagnosis or ordering appropriate confirmatory investigations if needed such as ultrasound, X-ray, CT scan, MRI, arthroscopy, joint aspirate analysis and microscopy, and various blood work panels.
Some imaging investigations may require the injection of a dye (gadolinium) into the joint for better visualization. (8)
Who Are More Prone to Musculoskeletal Pain?
Everyone is prone to MSK pains; it’s the price of living and enjoying life.
However, some risk factors can put individuals at high risk of chronic MSK pains. These include connective tissue and genetic disorders (such as Ehlers-Danlos syndrome), obesity, mood disorders, numerous injuries or significant trauma, smoking, diabetes, and low bone mass/density.
Dehydration, overexercising, overuse and repetitive tasks, awkward positions, and poor biomechanics while sitting or lifting are all secondary causes of MSK pains.
What Home Remedies Can Be Used to Treat Musculoskeletal Pain?

MSK pain can generally be treated conservatively at home by using hot and cold compresses, rest, and supplementing the diet with natural anti-inflammatories such as green tea, ginger, turmeric, (9) and curcumin.
Similarly, some people reap benefits from avoiding inflammatory foods and drinks such as alcohol, refined carbohydrates, gluten, monosodium glutamate, saturated and trans fats, salt, and alcohol.
Some studies have found dietary supplements such as glucosamine and chondroitin to be effective in alleviating MSK pain, especially in patients with arthritis. You can easily get them at your local pharmacies without a prescription.
How Can One Differentiate Between Musculoskeletal Pain and Normal Pain?

All pain is both normal and abnormal at the same time; it depends on the extent or severity of the said pain and its effects on one quality of life.
It’s normal to experience all types of pain, such as neuropathic or nociceptive pain (such as MSK pains), in response to an appropriate trigger. For example, if you fall and break your bone, you should have MSK pain, that’s the normal response; it would be abnormal to not feel pain in this scenario.
However, pain without a trigger, pain that is very intense and out of proportion to the trigger, or pain that lingers much longer after the trigger has resolved is abnormal pain.
Thus, normal pain can be MSK pain that is triggered by a certain cause, whose intensity is not out of proportion to the trigger, and that is self-limiting after the trigger has resolved. Abnormal MSK pain fits the opposite of these.
Final Word
A common theme within sports medicine is the best medicine is always prevention. Thus, MSK pains and ailments can be avoided by following a healthy diet, maintaining a healthy weight, and getting regular exercise with both 150 min/week of cardio exercises and 3 days/week of additional core and strength conditioning.
Stress management, ergonomic work environments, mindfulness of biomechanics, or seeing a physiotherapist/occupational therapist to ensure great biomechanics while exercising or working can all prevent MSK pains from occurring.
Most causes of MSK pains can be diagnosed clinically by your doctor without the need for imaging. Most causes also do not require any invasive procedures to heal, and a combination of the above recommendations and time heals most cases. (10)
MSK pain is best treated by a multidisciplinary team of medical doctors, naturopathic doctors, physiotherapists and occupational therapists, chiropractors, massage therapists, acupuncturists, and pain specialists.
- Was this article helpful?
- YES, THANKS!NOT REALLY


