In this article:
Rheumatoid arthritis (RA) is a chronic autoimmune disorder characterized by inflammation of the peripheral joints, leading to pain, stiffness, and joint damage and deformity over time.
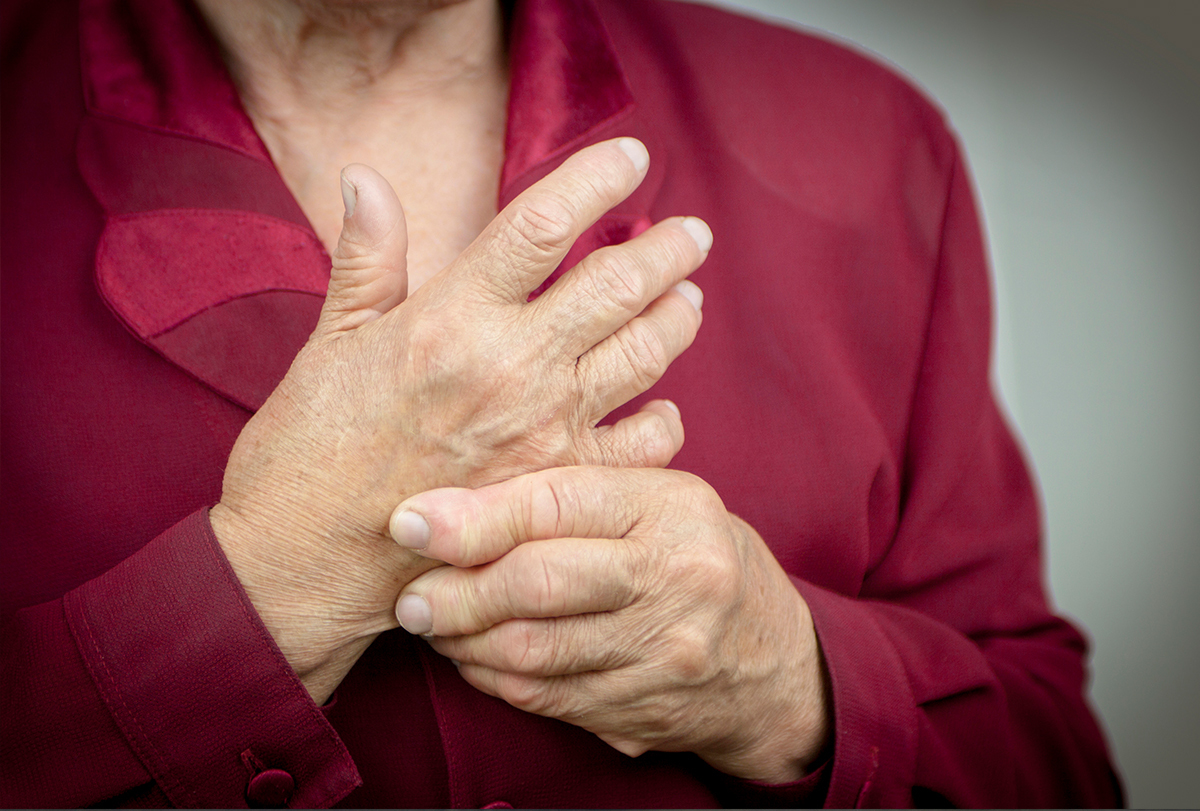
It is a systemic condition, which means inflammation may be present throughout the body, causing fatigue, low energy, anemia, and in some cases, the involvement of body tissues beyond the joints.
How Common Is Rheumatoid Arthritis?
RA is a relatively common disorder and affects 0.24%–1% of the world population.
The incidence of the disease may even be on the rise. In North America, the disease incidence is about 40 per 100,000. (1) Women are affected almost two times more than men.
Different Stages of Rheumatoid Arthritis
Rheumatoid arthritis has four stages, which indicate disease severity:
Stage 1, mild or early-stage RA
In this stage, there is evidence of joint swelling and stiffness but no deformities, and the X-rays indicate no underlying bone damage.
Stage 2, moderate disease progression
In this stage, there may be subtle radiographic signs of joint injuries, such as cartilage loss or early bone changes. The swelling becomes so advanced that it starts hampering joint flexibility, but there is still no deformity.
The tissue inflammation may spread beyond the joint to the adjoining area and even lead to some degree of adjacent muscle atrophy.
Stage 3, advanced disease
There is joint swelling, loss of range of motion, and deformity. X-rays reveal substantial joint damage with bone erosion and extensive loss of cartilage.
Stage 4, end-stage or terminal disease
The joint tissue becomes completely damaged or lost such that there is no swelling, only pain and stiffness accompanied by joint deformity and loss of function. There may be bony “ankylosis,” which means the joints have fused together and have become rigid.
Types of Rheumatoid Arthritis
Due to a lack of knowledge about the cause of RA, it is difficult to classify the disease completely.
As different patients exhibit varying progression rates and symptoms, the disease is currently classified into seropositive or seronegative RA. This basic and primary classification can help determine treatment options.
1. Seropositive rheumatoid arthritis
It is determined by the presence of anti-cyclic citrullinated peptides (anti-CCPs) in the blood. Also known as anti-citrullinated protein antibodies (ACPAs), these peptides are produced by the body in response to a molecular change of proteins called citrullination.
Anti-CCPs are found in around 60%–80% of people having RA. A positive test for anti-CCPs and the presence of RA symptoms are an approximate confirmation of the disease.
Initially, this test was performed to check the presence of rheumatoid factor, which is an antibody that attaches to other antibodies. Various tests can help determine rheumatoid factor levels. However, the anti-CCP test is more specific to RA and is the preferred choice.
2. Seronegative rheumatoid arthritis
An absence of anti-CCP antibodies in the blood while having all other symptoms that are consistent with RA indicates the possibility of having the seronegative type of RA.
Causes of Rheumatoid Arthritis
The actual cause of RA is unknown, although there are many theories, including:
- Genetic determinants may play a role in the development of RA.
- Environmental factors, such as an infection or a toxin, may trigger the immune system in people who are at a high risk of developing RA.
- Leaky gut is often considered a prominent factor. Irritation of the intestinal lining as a result of ingesting certain foods, chemicals, and environmental toxins may result in local inflammation that overwhelms the capability of the gut immune system to contain the irritant. This may lead to systemic immune system activation.
- A poor diet or the overuse of antibiotics may alter the normal intestinal bacterial population, which leads to “dysbiosis” and further contributes to the leaky gut problem.
- Molecular mimicry, wherein the immune system wrongly perceives your healthy tissue as a foreign threat in the wake of infection or environmental exposure and starts attacking the body itself, may result in RA.
Signs and Symptoms of Rheumatoid Arthritis
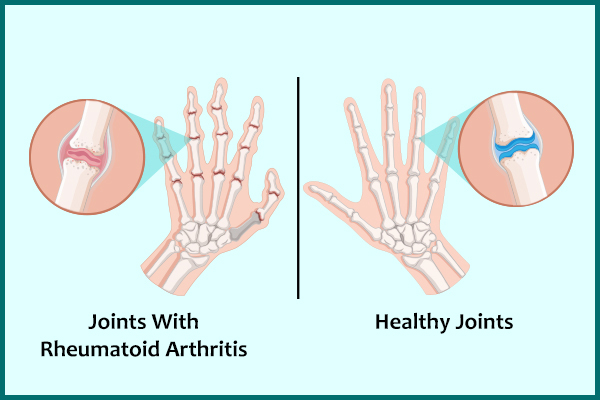
RA usually presents as symmetrical arthritis, which means both hands, both knees, or both wrists, for example, are affected. This is a characteristic feature of RA.
The most common signs of rheumatoid arthritis include:
- Joint pain and tenderness
- Swelling in the joints
- Redness and warmth in the joint
- Stiffness and restricted range of motion of the joints
- Joint deformity
- Tiredness
- Fever
- Hard bumps (called rheumatoid nodules) around the joints, present below the skin
- Red, puffy hands
- Loss of appetite
Treatment for Rheumatoid Arthritis
Rheumatoid arthritis is typically treated with different drugs that address different aspects of the condition, along with other interventions that focus on easing joint stress and improving joint function.
1. Medication
You may be given a combination of medicines, and the prescription and choice of the drug may change over the course of treatment as your symptoms evolve or worsen.
The doctor usually starts treatment with disease-modifying antirheumatic drugs (DMARDs), such as methotrexate, leflunomide, hydroxychloroquine, and sulfasalazine. These drugs aim to provide symptomatic relief while also slowing the progression of the disease.
DMARDs may be clubbed with NSAIDs, pain killers, and low-dose corticosteroids to reduce the inflammation and pain in the joints for better mobility.
When DMARDs are insufficiently effective in a patient with RA, the next step is the addition of biologic agents, such as infliximab (Remicade), etanercept (Enbrel), adalimumab (Humira), and abatacept (Orencia).
Caution: Excessive or prolonged use of corticosteroids can improve your symptoms but greatly damage your body in the process. Thus, this drug must only be taken in the doctor-prescribed small doses and for a limited time.
2. Physical therapy
This includes customized exercises, joint massages, and heat and cold treatment to improve joint flexibility and mobility.
3. Occupational therapy
The therapy is designed to restore the range of motion in the damaged joints so that you can go about your daily activities with relative ease. It helps you adapt to your condition rather than undo the damage and is performed under the guidance of a trained specialist.
4. Surgery
If a joint becomes severely damaged, usually seen in stages 3 and 4 RA, joint replacements may be required. Knee and hip surgical replacements are generally quite successful, as are shoulder joint replacements.
But for smaller joints, such as those of the hands and feet, wrists, and elbows, joint replacement surgery is not available.
Some orthopedists perform ankle replacement surgery, but this procedure has mixed success. There are no surgical interventions that treat RA per se, only those that treat end-stage joint damage.
Most Commonly Affected Joints in Rheumatoid Arthritis
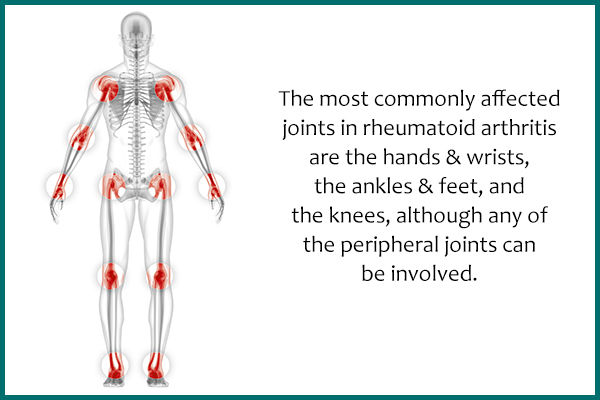
RA may involve multiple joints or just a few. Sometimes, a person can have severe disease and damage in one or two joints with no involvement elsewhere. Others have mild or moderate severity but the involvement of many joints.
- The most commonly affected joints in RA are the hands and wrists, ankles and feet, and knees, although any of the peripheral joints can be involved.
- The cervical spine (neck) may also be affected, but the rest of the spine is generally not involved in RA. That is, low back and spine pain is generally not a problem for patients with rheumatoid arthritis.
- Although less common, the hips, elbows, and clavicular joints (collar bone) that connect to the sternum (breast bone) or shoulder may exhibit rheumatoid inflammation.
- RA mostly targets the large knuckles (the metacarpophalangeal, or MCP, joints) and the first finger joints (proximal interphalangeal, or PIP, joints) while sparing the smallest finger joints (the distal interphalangeal, or DIP, joints).
How Is Rheumatoid Arthritis Diagnosed?
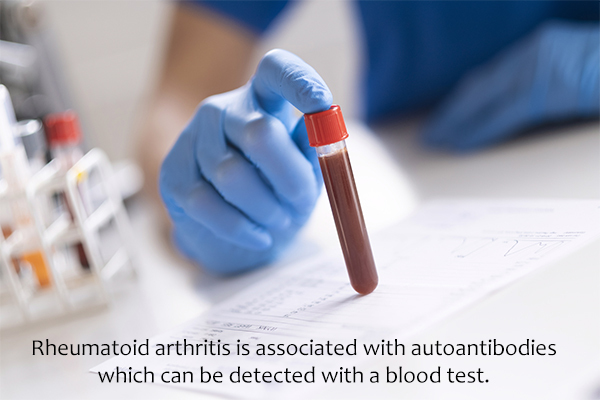
A physician familiar with RA, usually a rheumatologist, is best suited to make a diagnosis of RA. The doctor will conduct a few blood tests to detect the presence of two antibodies, namely rheumatoid factor (RF) and anti-CCP antibodies.
Together, the RF and anti-CCP tests can identify over 80% of patients with RA, whereas nearly 20% of patients with RA test negative for these autoantibodies despite having the disease.
For this reason, RA diagnosis cannot be based on antibody tests alone and has to be compounded with characteristic symptoms, X-ray changes, and other blood tests that may reveal anemia and an elevated sedimentation rate and C-reactive protein, which are signs of inflammation in the body.
Risk Factors for Rheumatoid Arthritis
Several factors can predispose you to develop RA, including:
- Genes: People with a family history of RA are slightly more prone to it, but inherited factors don’t play a major role in its development.
- Environment: Toxic substances, such as air pollution, chemicals, smoke, and insecticides, can negatively affect the body, often contributing to joint pain in patients with RA.
- Hormones: More women are seen to be affected by RA than men. This could be indicative of a link between female hormones and RA.
- Unhealthy lifestyle: Researchers suggest that poor lifestyle habits such as smoking, obesity, and poor health can undermine one’s immune system, and thereby pave the way for autoimmune diseases such as RA.
Possible Complications of Rheumatoid Arthritis
In general, patients with RA have frequent “comorbidities,” that is, other chronic disorders that complicate their overall health. (2)
- Patients with RA have reduced healthspan and lifespan. (3)
- RA increases the risks of cardiovascular diseases, such as hypertension, diabetes, and elevated cholesterol, even beyond the usual factors.
- Patients with RA also have about twice the risk of lymphoproliferative diseases, such as leukemia and lymphoma.
- Some of the medications used for RA treatment may result in adverse effects and can increase the risk of infection or kidney problems, thus requiring close monitoring.
When to See a Doctor
The sooner you treat RA, the better. Early diagnosis leads to timely treatment, which keeps the condition from getting worse and resulting in more serious complications.
It is recommended to schedule a visit to your doctor if you experience:
- Prolonged swelling and soreness in your joints for weeks
- Stiffness in the joints on waking up
Expert Answers (Q&A)
Answered by Dr. Rajat Bhatt, MD (Rheumatologist)
Here are two differences between RA and OA:
• Osteoarthritis is degenerative arthritis that occurs with age or secondary to injury. Rheumatoid arthritis is inflammatory arthritis in which the body attacks its own joints, leading to inflammation and deformities.
• RA of the hands mostly affects the large knuckles with rarely any swelling, pain, or stiffness in the smallest finger joints. This is in stark contrast to OA, which typically involves the smallest finger joints with little to no discomfort in the large knuckle joints.
Yes, physical or psychological stress can lead to flare-ups of rheumatoid arthritis.
Joint deformities can develop, and the condition can have adverse effects on workability. It can also lead to intractable pain.
No.
It depends on the joints involved. Hand exercises often help. Squeezing a ball and stretching the back and hips also might help.
Avoid an inflammatory diet, red meat especially. Some studies show avoiding sugar might help as well. (4)
Final Word
Rheumatoid arthritis is a lifelong condition that gets progressively worse if not managed properly. You must act fast to curb the joint damage in the early stages, or else this condition can turn into a disability.
The pain, stiffness, and swelling in the joints can get so severe that you will find it difficult to move about and perform even the most basic tasks. So, get evaluated at the first sign of RA, rather than waiting for the symptoms to escalate. Treatment is unlikely to bear satisfactory results once your joints become badly damaged.

- Was this article helpful?
- YES, THANKS!NOT REALLY


