In this article:
Mouth ulcers are open sores that can give rise to a great deal of pain and discomfort in the oral cavity. These lesions usually have a white or yellow center surrounded by an inflamed red border.

They often appear on the inside of the cheeks, on the lips, under the tongue, on the floor of the mouth, or at the base of the gums. Although they are relatively harmless, they can be extremely irritating and discomforting nuisance.
Causes and Types of Mouth Ulcers
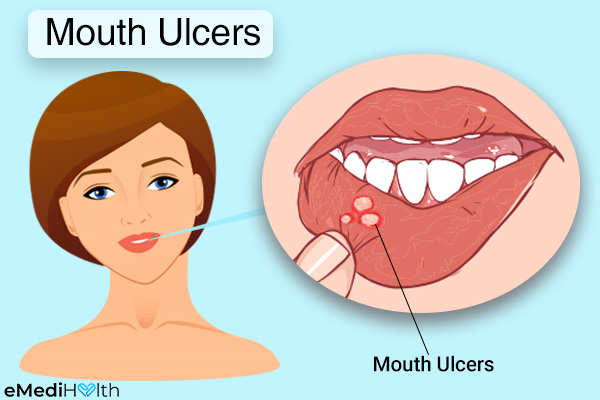
Mouth ulcers are broadly categorized as traumatic or aphthous.
1. Traumatic mouth ulcers
Traumatic mouth ulcers result from trauma that causes erosion of a part of the mucous membrane, which is the delicate tissue lining the inside of your mouth.
Ulcers caused by trauma or injury usually appear as singular and painful sores next to the source of damage and often resolve by themselves once the cause is removed.
Many factors can give rise to traumatic mouth ulcers, such as:
- Biting the inside of the cheek or tongue by accident
- Poor-fitting dentures and braces or rough fillings
- The constant friction of the mouth or tongue against crooked or sharp teeth
- Rigorous brushing or accidental scraping of the oral soft tissues while brushing
- Burning your mouth by consuming hot food or beverages
- Cutting your gums or the insides of your cheek by eating hard, rough, or crunchy foods, such as toast, chips, pizza, and bread crust
- Irritating the lining of your mouth by using strong antiseptics
- An allergic reaction to some toothpaste ingredients
2. Aphthous mouth ulcers
Aphthous mouth ulcers are recurring episodes of mouth ulcers in otherwise healthy individuals. This condition remains largely idiopathic. Aphthous ulcers afflict around 20%–30% of the entire population and are classified into three different types, namely, minor, major, and herpetiform.
a. Minor aphthous ulcers
Minor aphthous ulcers are characteristically small in size and pale yellow with visible swelling and redness in the area around them.
Minor ulcers are the most common of all types of mouth ulcers. They commonly occur as a single lesion, but they can sometimes develop in a cluster of up to five at the same time. It can take between 7 and 10 days for minor ulcers to resolve and heal completely.
As the name suggests, minor aphthous ulcers are associated with relatively minimal pain and virtually no signs of scarring. Ulcers such as these are commonly referred to as canker sores. However, it would be wrong to assume that all mouth ulcers are canker sores.
b. Major aphthous ulcers
Major aphthous ulcers are relatively severe and take a long time to heal. Each major ulcer is likely to take between 2 weeks and several months to resolve.
These ulcers tend to be relatively larger than the minor ones, extending to 10 mm or larger across. They are irregularly shaped and slightly raised. Major ulcers generally do not appear in a cluster, and only one or two may appear at a time.
As they penetrate deeper into the tissue, major ulcers tend to leave behind a scar. Large ulcers can give rise to a lot of pain and discomfort, which can make eating difficult. Sometimes, the ulcer may appear near the tonsils, which can make swallowing quite difficult.
c. Herpetiform ulcers
Herpetiform ulcers are so named due to their uncanny resemblance to the sores associated with herpes. They are the size of a pinhead and generally not more than 1–2 mm in diameter.
Multiple ulcers of this kind usually occur together in clusters and can sometimes join together to form large, irregular-shaped ulcers. These ulcers have a tendency to recur very quickly, so the condition may seem quite chronic. Usually, an ulcer of this kind takes between 2 weeks and 2 months to heal.
Herpetiform ulcers are more prevalent among women than among men, and there is a greater incidence reported in older adults.
Signs and Symptoms of Mouth Ulcers

Most mouth ulcers can occur anywhere on the lining of the mouth – on lips, the floor of the mouth, and inside of the cheeks, under the tongue, and rarely, on the roof of the mouth.
The signs and symptoms of mouth ulcers tend to vary depending upon the cause, but most cases of mouth ulceration are usually accompanied by:
- The development of one or multiple open sores in the mouth
- Pain or discomfort in the mouth
Typical mouth ulcers share some easily identifiable physical characteristics:
- A mouth ulcer is usually round or oval in shape.
- Mouth ulceration can manifest as a single lesion or multiple sores on the soft, sensitive lining of the mouth.
- The lesion can be white, yellow, or gray in the center and is usually surrounded by red, swollen edges.
- The soft lining of the mouth around the wound tends to be extremely tender, which can make chewing and brushing extremely painful.
In extreme cases, the patient may also experience the following symptoms:
- Fever
- Loss of appetite
- Lethargy
- Swollen glands
Standard Treatment for Mouth Ulcers
The standard treatment for mouth ulcers involves the following steps.
1. Treatment of the cause
If the ulcer is caused by a bacterial infection, the doctor may prescribe a course of antibiotics to treat the underlying problem. If the ulcer results from constant friction against a misaligned or sharp tooth, your dentist will file down the jagged edges.
Ill-fitting dentures and braces can also be properly affixed by your dentist if they are found to be the source of trouble. (1)
2. Topical treatments
Your doctor may suggest certain ointments, creams, or other substances to be applied topically on the ulcerated skin. These include anesthetics, corticosteroids, and protective coatings to promote fast healing and to ease the discomfort.
Topical treatment may also involve burning the ulcer with a laser or chemicals, which is only to be done under the doctor’s supervision.
Diagnosing Mouth Ulcers
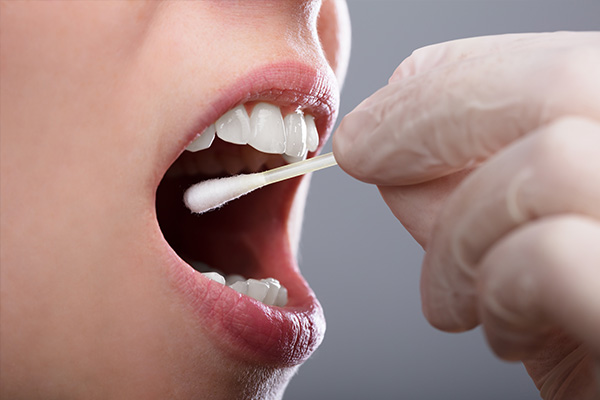
Because mouth ulcers are completely benign, mild cases generally do not require a visit to the doctor for a proper diagnosis. (2) However, if the lesion persists for longer than 3 weeks, worsens with time, or frequently recurs, getting a formal diagnosis is necessary.
Your doctor will conduct a close examination of your oral cavity and will order a few tests if necessary, which may include:
- Swab tests
- Complete blood count
- Iron, folate, and B12 tests
- Celiac antibody count
If the preliminary test results are inconclusive or if your condition persists, your doctor will have to extract a small portion of the ulcer and the adjoining skin tissue, which is then tested to identify probable causes.
In rare cases, an endoscopy may be performed to rule out the risk of inflammatory bowel disease.
Complications Related to Mouth Ulcers
Mouth ulcers generally clear up within 2 weeks, but in some rare cases where the ulceration is severe and extensive, the wound may give way to a secondary bacterial infection.
When to See a Doctor
Most cases of mouth ulcers generally resolve on their own without any medical intervention. However, it is essential that you consult a dentist, an oral medicine specialist, or an ear, nose, and throat specialist (otolaryngologist) if:
- The condition becomes so painful that it starts to disrupt your daily life.
- The mouth ulcer does not clear even after 3 weeks.
- Your gums begin to bleed.
- You develop white patches on your tongue or anywhere inside the oral cavity.
- The pain and redness in and around the ulcer get worse.
- You constantly run a fever higher than 100.5°F (taken by mouth).
- You notice new or unusual symptoms as the condition progresses.
- The ulcer shows no sign of subsiding despite adequate self-care.
- The mouth ulcers keep coming back.
Expert Answers (Q&A)
Answered by Dr. Mugdha Motani, BDS (Dentist)

Recurrent mouth ulcers could have multiple causes:
– Repeated abrasion due to a faulty denture or a sharp tooth or filling
– Oral thrush infection
– Genetic predisposition to mouth ulcers
– Poor oral hygiene
– Stress/anxiety
– Nutritional deficiencies (such as vitamin B12 or iron)
– Low immunity/autoimmune diseases
– Hormonal fluctuations during puberty, pregnancy, or menopause
– Blood disorders such as anemia
– Skin conditions such as lichen planus
– Inhalers that contain steroids, such as those for asthma or COPD
– Side effects of some drugs
– Bacterial or viral infection
– Cancer of oral region
– Radiotherapy/chemotherapy involving the oral region
– Celiac/inflammatory bowel disease
No. Touching or rubbing an ulcer will cause irritation and more pain.
Not all oral ulcers mean cancer. Typically, a mouth ulcer heals within 2 weeks with no scar formation.
If an ulcer that is present in the mouth is a mix of red and white areas with ragged, uneven edges and for more than 2 weeks, it needs to be checked by a dental professional.
No. Rather, sometimes agents such as mint present in toothpaste can irritate the mouth ulcer more.
Teens and preteens are more susceptible to ulcers, especially females. Children with low immunity and nutritional deficiencies are also at higher risk.
About Dr. Mugdha Motani, BDS: Dr. Motani has over 10 years of experience in dental surgery. She has also worked in some of the most reputed medical institutes such as the All India Institutes of Medical Sciences (AIIMS) in India and the National Health Service (NHS) in the United Kingdom.
Final Word
Mouth ulcers are a common oral problem among people. However, they are usually harmless and resolve within 10 days. You can also use topical ointments to help reduce pain and support recovery.
In case the ulcer is prolonged, causes discomfort, or interferes with your daily routine, you must consult a dentist.

- Was this article helpful?
- YES, THANKS!NOT REALLY


