In this article:
Keloids are an aggressive form of scars that usually develop due to excessive growth of thick, fibrous tissues over the site of a wound. Although a rarity, a keloid can develop without any skin injury in some people, known as a spontaneous keloid.
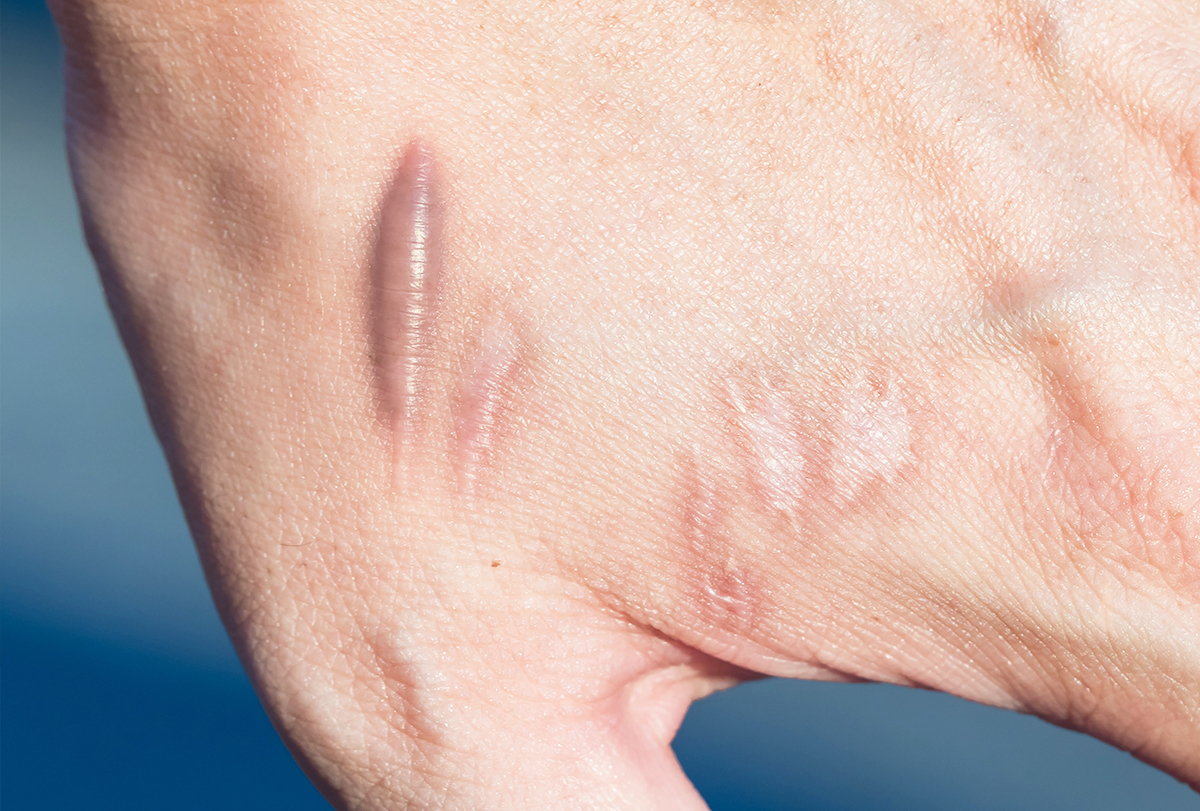
Keloids can be of varying shapes and sizes, depending upon the site of scarring. They can become considerably painful and itchy as they continue to grow.
Causes of Keloids
In the event of a superficial injury, the skin tries to heal itself by producing an increased amount of collagen at the affected site. This leads to the formation of scar tissue over the wound to prevent further damage to the affected skin.
In some cases, extra layers of scar tissue keep piling up, resulting in a keloid. Such excessive tissue growth is usually noticed in the case of:
- Acne
- Piercings
- Minor burns
- Tattoos
- Chickenpox
- Bites
- Scrapes
- Cuts
- Surgical incisions
Signs and Symptoms of Keloids
Keloids can form anywhere on the body up to three months post-injury. However, some areas are more prone to this type of scarring, which includes the chest, shoulders, cheeks, upper back, and earlobes.
Keloids are characterized by the following:
- A pinkish flesh color to a deeper red or purple
- A lumpy or jagged feel
- Elevated and firmer than the surrounding skin, having a smooth surface
- Tender to the touch
- Itchy
- Sensitive to irritation and sunlight
Medical Treatment
The standard treatment for keloids involves both surgical and nonsurgical options. Some of the most commonly used methods for improving the appearance of scars or the complete removal of keloids are as follows.
1. Steroid injections
Directly injecting a long-acting corticosteroid solution into the scar can help make the keloid less noticeable. When injected into the skin, the steroids work by splitting the links between collagen fibers. This mechanism helps break down the accumulated scar tissue under the skin.
Steroids are also credited with a potent anti-inflammatory action that can help provide symptomatic relief from the itching, redness, swelling, and tenderness that usually accompany keloid formation.
2. Direct surgery
If nonsurgical treatment fails to remove or diminish the appearance of keloid scars, you may have to consider more invasive options such as surgery.
Direct surgery is usually preferred in addressing more severe scarring. It involves making an incision into the affected site to remove the extra layer of scar tissue and then tying up the open cut with stitches.
3. Cryotherapy
Yet another fairly noninvasive therapy involves the use of cold therapy to freeze the scar tissue before removing it from the body. This treatment method works primarily for small-sized keloids and is particularly effective for light-skinned patients. (1)
Cryosurgery is often paired with a monthly dose of cortisone injections.
4. Laser surgery
Laser surgery is not a standalone treatment for keloids, but it works in conjunction with several other therapeutic tools. The laser can help reduce the height of the scar, make the scar visibly smoother, or fade the abnormal discoloration of the scar.
5. Radiotherapy
Radiotherapy is generally given as an adjunct therapy after excising the keloid. Since it has an inherent risk of carcinogenesis, it is used only in a few cases, with caution.
Diagnosis of Keloids
Diagnosing a keloid is a pretty straightforward task for a skin specialist with a trained eye: one look at the scar and your doctor can immediately tell if it is a keloid or not.
If there is still some uncertainty regarding the diagnosis, your doctor will conduct a biopsy of the scar tissue, wherein a small sample of the affected skin will be closely examined under a microscope.
Who Is at Risk?
Some people have an increased tendency to develop keloids than others. These include the following groups:
- African-Americans
- People who fall in the age bracket of 10–30 years
- Young women who have their ears pierced
- People who have undergone an open-heart surgery
- Genetic predisposition
When to Call a Professional
Keloids are categorized as benign tumors that are unlikely to turn malignant. Even though they do not qualify as a major health concern, you are advised to consult a skin specialist if the condition becomes particularly bothersome, on account of the following reasons:
- The scar becomes particularly enlarged.
- The scar becomes excessively itchy and uncomfortable.
- The scar develops on a joint such that it impedes your movement.
- The scar makes you feel extremely conscious and starts affecting your emotional and mental well-being.
Expert Answers (Q&A)
Answered by Dr. Niyati Sharma, MBBS (Dermatology)
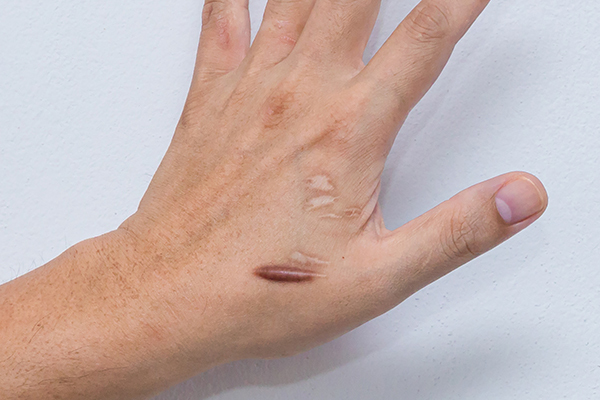
No, it’s a permanent scar.
Yes. If you have a tendency to have keloids, avoid any cosmetic or other unnecessary procedures. Otherwise, at the time of surgery, your surgeon or dermatologist should insert intralesional cortisone to prevent keloids from occuring.
No, there is no such link. If, however, you have had no procedure done or had no acne in that area and the scar occurred spontaneously, please see your dermatologist, as it could be a cancerous growth.
Yes, that’s how it typically occurs or sometimes even due to severe forms of acne.
The best treatment so far is administering intralesional cortisone every 6 weeks. Cortisone is injected into the keloid via a small (diabetic) syringe.
Avoid rubbing keloids, as this can aggravate them. Keep them protected from the sun, and avoid any unnecessary procedures in the first place. If you have acne and you are forming keloids, treat acne aggressively with the help of your dermatologist.
Final Word
Keloids are primarily a cosmetic concern rather than a medical one. These abnormally large scars can make one conscious as they are difficult to hide, and can prove discomforting if they are located in certain tricky areas.
For instance, if you get a large keloid over a joint, it can be difficult to move the affected area. But if you tend to the injured site as soon as possible, there is a chance that the scar may not grow to be a keloid.
Once formed, there are several topical treatments that can help reduce the visibility of the scar but none of them can heal it completely.

- Was this article helpful?
- YES, THANKS!NOT REALLY


