In this article:
Molluscum contagiosum is a skin condition that results in the formation of small, raised bumps on the skin. The bumps are usually painless, but they can be itchy and unsightly, and some people may feel self-conscious about them.
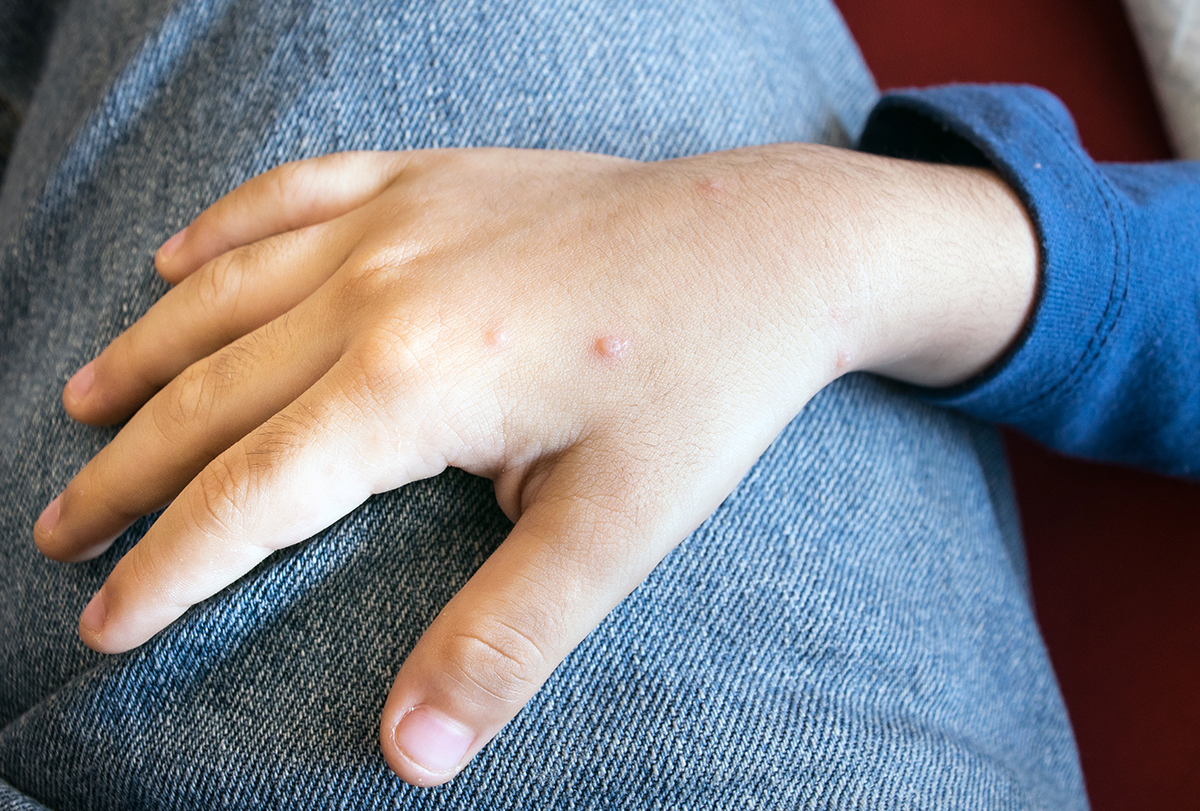
Molluscum contagiosum is caused by a virus, and it is highly contagious. (1) It is also known as water warts and mostly affects children aged 1–10 years.
Causes and Spread of Molluscum Contagiosum
Molluscum contagiosum occurs when you acquire the molluscum contagiosum virus, a type of poxvirus. It is an infectious virus, commonly seen among children, sexually active adults, and people with compromised immune systems.
The common symptom observed is firm pink or skin-colored papules on the skin that can last 6–9 months. The growths may look different and may be resistant to treatment in adults. (1)
Molluscum contagiosum is common in people who live in warm, humid climates with crowded living conditions.
Someone with molluscum contagiosum can also spread it to other parts of their body if they touch a lesion and then touch their body elsewhere, which is referred to as autoinoculation. Shaving may also spread molluscum contagiosum to other parts of the body. (1)
While lesions are present, this virus can spread from one person to another. The virus can also spread from one region of the skin on one portion of your body to another.
The virus can spread through direct contact with an infected person or through contact with contaminated surfaces. It can also be spread through sexual contact. (1)
Symptoms Indicative of Molluscum Contagiosum
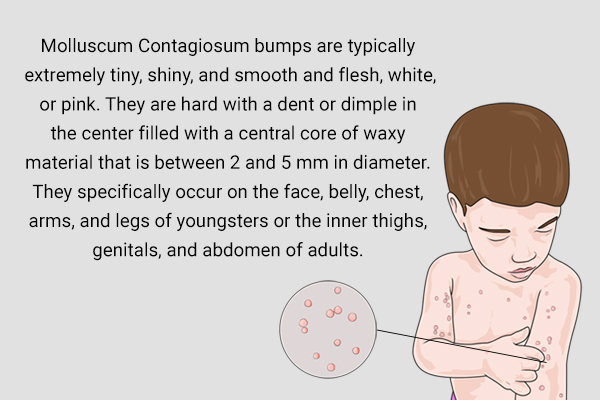
The symptoms of molluscum contagiosum generally are lumps, which may show up singly or in a cluster of up to 20. The lumps are characterized as follows:
- They are typically extremely tiny, shiny, and smooth and flesh, white, or pink. They are hard with a dent or dimple in the center filled with a central core of waxy material that is between 2 and 5 mm in diameter.
- They specifically occur on the face, belly, chest, arms, and legs of youngsters or the inner thighs, genitals, and abdomen of adults. They can be between the size of a pinhead and the size of an eraser on the top of a pencil and can be present anywhere other than on the palms of your hands or the soles of your feet. (1)
Treatment for Molluscum Contagiosum
Efficient molluscum contagiosum treatments can be carried out by a medical professional. These consist of:
- Cryotherapy: Each bump is frozen by the doctor using liquid nitrogen. (2)(3)
- Curettage: With a little tool, the doctor pierces the lump and scrapes it off the skin. (2)(3)
- Laser treatment: Every bump is eliminated by the doctor using a laser. (3)
- Topical treatment: To cause the top layers of skin to peel off, the doctor administers lotions containing acids or chemicals to the lumps. Iodine, salicylic acid, tretinoin, and cantharidin may be found in topical treatment creams (a blistering agent that a doctor usually applies). (2)(3)
Note: During the surgery, anesthesia may be required. (3) These techniques target individual bumps; therefore, the treatment may need more than one session. If you have a lot of huge bumps, you might need extra treatment every 3–6 weeks until the bumps go away. As the current bumps heal, new ones could develop. (4)(5)
When to See a Doctor
You should see a doctor if you notice lesions in the genital area, such as near the penis, vulva, vagina, or anus.
Ideally, you should see a doctor as soon as the first symptoms appear. However, the lesion can sometimes be mistaken for an allergic reaction to dust and other allergens, and this can delay the patient in seeking treatment.
If you have skin lesions that have not disappeared within 24–48 hours and are increasingly painful and swollen, it may be time to consult a doctor and a dermatologist. (1)
Final Word
As with all viral diseases, the quickest way to cure a case of molluscum contagiosum is to pay a visit to your doctor and follow the recommended treatment plan.
Although unsightly, the virus can be dealt with effectively and with minimal discomfort if treated timely.
 Continue Reading6 Home Remedies for Molluscum Contagiosum and How to Use Them
Continue Reading6 Home Remedies for Molluscum Contagiosum and How to Use Them
- Was this article helpful?
- YES, THANKS!NOT REALLY


