In this article:
Keratosis pilaris, also known as chicken skin, is one of the most common but totally benign dermatological disorders characterized by rough bumpy patches on different parts of the body.
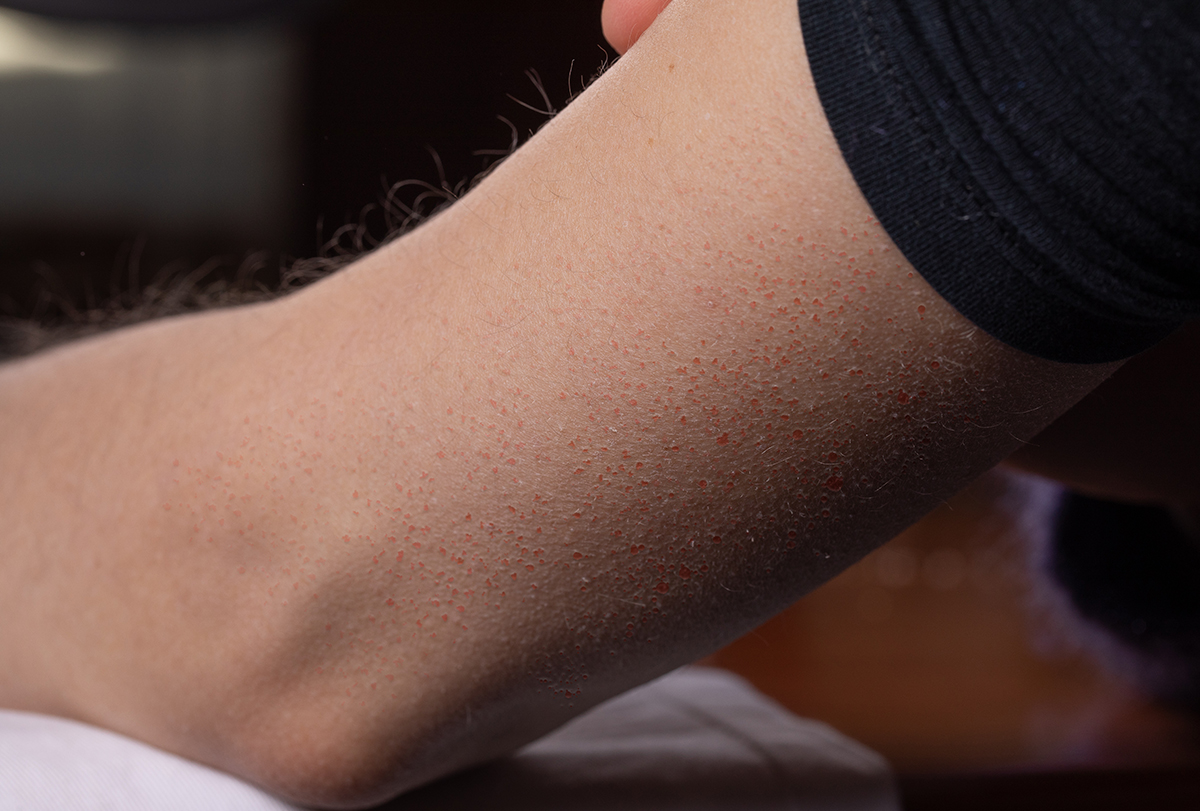
This condition typically starts in early childhood with mild localized lesions. It eventually spreads to larger areas of the skin between the ages of 10 and 20 years.
Keratosis pilaris will resolve on its own after running its full course, usually by the age of 30. In the meantime, there are things you can do to speed up the skin healing process and reduce the severity of the symptoms.
This article presents tried-and-tested treatment modalities, home remedies, and tips that can help you manage this condition better.
Cause of Keratosis Pilaris (Bumps on Arms)
The exact root cause for this condition is not clearly understood, but several factors are known to contribute to it. Your sex or racial ethnicity does not increase the risk of you developing keratosis pilaris, but people with certain preexisting dermatological or medical conditions are more prone to it.
Research suggests that keratosis pilaris is more common in people who suffer from atopic dermatitis, ichthyosis vulgaris, obesity, diabetes mellitus, Down syndrome, Noonan syndrome, or malnutrition. (1) Genes are also involved in the onset and progression of this disease. It occurs when the genes responsible for producing filaggrin (filament-aggregating protein) become mutated and do not work properly.
Filaggrin is abundantly present in the outermost part of the epidermis known as the stratum corneum, which performs the barrier function of the skin. This means that the stratum corneum serves as the body’s first line of defense against foreign irritants.
Filaggrin plays a critical role in strengthening this skin barrier as it binds keratin and other structural proteins tightly together. This surface layer must remain intact to deny entry to external irritants while also preserving water in the skin.
However, nearly 8%–10% of the global population is born with mutated genes that do not produce enough filaggrin to maintain a healthy and strong stratum corneum. As a result, the skin is unable to retain water and ward off irritants well enough, leading to severe dryness, which can take the form of eczema, dermatitis, and keratosis pilaris.
The genetic involvement in such conditions suggests that they can be passed on from one generation to the next.
There are other problems in the body chemistry that can trigger keratosis pilaris as well, such as a dysfunction in the RAS cascade system. What happens here is that the cells lining the insides of your hair follicles start producing too much keratin protein, which builds up inside the follicle cavity and ends up clogging them.
This triggers inflammation in the surrounding skin. These “keratin plugs” eventually take the form of papules or raised bumps that appear red due to the underlying inflammation.
You can get these bumpy patches on any part of the body where hair follicles are present, but they mostly appear on the upper arms, thighs, buttocks, and even the face. The skin around these bumps also tends to dry up and turn scaly, and the hair within these red bumps becomes coiled. (1)
Treatment for Keratosis Pilaris (Bumps on Arms)
The dry, bumpy skin caused by keratosis pilaris is rarely itchy or painful but looks rather unappealing, which can make you self-conscious. Some people are more affected by these cosmetic concerns than others and therefore suffer a great deal of emotional distress due to this condition.
The good news is there are medical interventions that can help improve the appearance of bumpy skin. Most of these modalities work by gently exfoliating the outermost layer of the skin, which helps open up clogged hair follicles to flatten the bumps and reduce inflammation in the area.
So even though keratosis pilaris is a self-resolving condition that subsides over time and does not require any treatment, you can still try the following interventions to improve your skin texture while it persists: (2)
- Topical skin products can provide exfoliation and moisturization. These include emollients to hydrate your dry skin, keratolytic agents such as 6% salicylic acid lotion or 20% urea cream that trap moisture in the skin and help remove the cellular debris clogging the hair follicles, and retinoids (vitamin A derivatives) such as 0.01% tazarotene and vitamin D3 derivatives that can facilitate faster skin regeneration.
- Laser therapy using different types of laser beams, such as alexandrite laser, YAG laser, fractional CO2 laser, and pulse dye laser can help break the bonds between the epithelial cells accumulated on the surface of your skin so that they become easier to shed. Plus, the laser rays penetrate deep into the dermis to stimulate collagen synthesis, which is needed for the formation of new healthy skin. (3)(4)
- Chemical peeling procedures using glycolic, kojic, or lactic acid help accelerate the shedding of the outermost skin layer, inadvertently helping eliminate the keratin buildup inside your hair follicles.
- Microdermabrasion treatments use a minimally abrasive instrument to gently sand your skin, removing the thicker and uneven outer layer.
Home-Based Interventions for Keratosis Pilaris
Here are a couple of things you can do at home to aid the removal of keratin plugs from your hair follicle and thus make the bumps on your skin less noticeable and alleviate the associated inflammation:
1. Follow a dermatologist-recommended skin care routine
Many dermatologists recommend the following three-step plan to be followed every day until clearer skin is observed.
Start with gentle exfoliation

Your skin keeps regenerating and repairing itself by shedding dead damaged cells from its surface and making new cells to take their place. This is a gradual process, and it takes almost a month for the entire outermost layer of the skin to be replaced by a fresh layer from underneath.
Dead cells often start accumulating on the surface of the skin instead of sloughing off into the environment. This cellular buildup can trickle down into your skin pores and hair follicles to cause congestion, which will worsen a condition like keratosis pilaris.
Thus, it is important to exfoliate your skin once or twice a week to prevent the buildup of dead skin cells from its surface. Use mild exfoliating solutions such as Cetaphil or those that contain apple cider vinegar, grapefruit extracts, alpha and beta hydroxy acids (AHAs and BHAs), sugar beads, clay, kiwi extracts, 5% benzoyl peroxide, or coffee.
You can also prepare your own exfoliating masks with all-natural ingredients that are gentle on the skin. Simply mix a mild acidic agent such as yogurt, honey, milk cream, or lemon juice with a granular ingredient such as brown sugar, oatmeal, Himalayan pink salt crystals, or finely ground almonds or walnuts. The acid will help loosen the dead skin cells by dissolving the bond between them, and the granules will help scrub them off.
Wash the affected skin, apply the mask all over it, and gently rub it in light circular motions. Let the mask sit for 15–20 minutes and then rinse it off.
Don’t use regular scrubs as they can be too abrasive and further irritate or aggravate keratosis pilaris. If you find it difficult to remove the dead cells with your bare hands, you can gently massage your skin with a loofah, buff puff, or rough washcloth to loosen and remove the flaky skin.
Apply a keratolytic

Once you have exfoliated your skin, apply a keratolytic agent all over it. This helps to remove any cellular debris that might have stuck to your skin even after the exfoliation process as well as the excess keratin oozing out of your follicles. Keratolytics work by softening the extra skin and keratin to facilitate their easy removal.
You can either consult a skin doctor to get a prescription-strength keratolytic such as a retinoid or urea or purchase an over-the-counter keratolytic that contains glycolic acid, alpha hydroxy acid (AHAs), or salicylic acid, depending upon the severity of your condition.
Note: Over-the-counter keratolytics contain a low concentration of active ingredients to avoid skin irritation, whereas prescription keratolytics can be quite intense and therefore must be used more carefully.
Whatever keratolytic you use, you must stick to the recommended dosage and direction of application to get the best results and to avoid any undue side effects. Excessive or frequent application can make your skin increasingly dry and irritated and can disrupt the skin’s natural pH, increasing the risk of infection.
If you experience skin irritation even after using the product correctly, discontinue its use and ask your doctor to prescribe a more suitable alternative.
Finish with a thick moisturizer
Keratolytics can be quite drying, so it is important to hydrate your skin with a good-quality thick moisturizer afterward. Preferably use an oil-free cream or ointment moisturizer with lactic acid, malic acid, vitamin C, squalene, urea, or chamomile extracts to prevent clogged pores and soothe your skin.
Reapply the moisturizer after washing your skin or whenever you feel its effects wearing out, at least twice or thrice daily.
2. Use aloe vera gel to soothe skin inflammation

The bumps caused by keratosis pilaris do not cause any pain or itching, but they are usually accompanied by localized redness (erythema) due to the underlying tissue inflammation.
Aloe vera gel can help bring down this inflammation to make your skin appear less red and irritated. This gel is credited with anti-inflammatory and cooling properties that can help calm your inflamed bumps. These effects can largely be traced back to a specific chemical found in aloe vera called aloin. Aloin is known to block the activity of cytokines, which trigger inflammation in the body. (5)
Plus, aloe vera gel is deeply hydrating, which helps banish the skin dryness associated with this condition. It also promotes cellular repair and works as an antimicrobial agent to prevent secondary skin infections.
How to use:
- Extract the gel from an aloe vera leaf and apply it all over the affected skin.
- Gently massage it in for a few minutes so that it is properly absorbed by the skin. Let your skin soak in the goodness of the gel for at least 30 minutes.
- Rinsing it off with cool water.
3. Get enough of vitamin D
Vitamin D facilitates the removal of excess keratin from the skin and therefore plays an important role in the management and prevention of keratosis pilaris.
Your body is capable of making this vital nutrient itself (inside the skin), but only when exposed to the UV rays of the sun. Thus, you must soak in some sunshine every day to keep your vitamin D levels up. The best time to do this is early in the morning when the atmosphere is clean and clear enough to allow direct sunlight.
Meanwhile, avoid the sun when it is at its peak (midday) as it can burn or damage your skin. No matter how bright it is outside, you must never step in the sun without wearing a broad-spectrum zinc- and/or titanium-based sunscreen on all the exposed areas of the skin.
Even though the sun is the biggest source of vitamin D, the increasing pollution and busy lifestyles prevalent today have made it almost impossible for people to maintain healthy vitamin D levels through sun exposure alone.
But worry not, you can meet part of your vitamin D needs through your diet. Eat vitamin D-fortified foods as part of an overall well-balanced, nutritious diet. If you still fail to get enough vitamin D through foods, speak to your doctor about starting a vitamin D supplement.
Measures to Prevent Flare-Ups

Keratosis pilaris is a self-resolving condition that gets better in its own time. So, while there is nothing you can do to cure it, you can observe some measures that can reduce the intensity and frequency of its flare-ups.
Some Dos
- Keratosis pilaris causes skin dryness but is also aggravated by it. Thus, a basic step for managing this condition and avoiding future flare-ups is to keep your skin properly moisturized at all times. Experts generally recommend thick emollients for this purpose as lightweight ones may not provide enough hydration to address the extreme dryness associated with this condition. The best time to apply moisturizer is when your skin is slightly damp after a wash because it locks in the moisture. Reapply the moisturizer whenever your skin starts to feel dry again.
- Don’t take frequent or long baths. The more you expose your skin to water, the drier it becomes, which can exacerbate your symptoms. As contradictory as it may sound, water tends to pull out the inherent moisture from your skin, leaving it dry and crinkly. Bathe once a day and for no more than 10–15 minutes.
- Don’t use hot water for bathing or washing as it strips away the natural lipids from your skin, making it drier than before.
- Add some oatmeal (6) to your bathwater to soothe your dry, inflamed skin. Oatmeal is not only moisturizing in nature but is also known to exhibit anti-inflammatory and anti-microbial properties.
- Living in a dry environment makes your skin dry as well, which can worsen keratosis pilaris. To avoid that, you must use a humidifier to moisten the air in your home. Your skin will extract the moisture from the atmosphere to keep itself hydrated. A humidifier is a necessity if you happen to live in an arid terrain or during the winter months when indoor heating sucks the moisture from the air. Adjust the settings to keep the humidity level between 45% and 55%. Make sure to clean the humidifier from time to time to keep it clean and mold-free.
Some Don’ts
- Do not shave or wax the skin affected by keratosis pilaris as it can cause more bumps. If you must, go for laser hair removal to get rid of the unwanted body hair without aggravating the sensitive skin.
- Only use mild cleansing solutions instead of regular soaps or detergents to clean your affected skin. Make sure the cleanser is devoid of common skin irritants such as fragrance compounds, harsh chemicals, and alcohols that can further dry out your skin and trigger flare-ups.
- While exfoliating or cleansing your skin, avoid any harsh scrubbing action as it can disrupt the epidermal barrier further, paving the way for more irritation, redness, and secondary infections.
- Do not exfoliate frequently as it can remove the natural oils from your skin and increase the dryness as well as compromise its structural integrity.
- Do not pick or scratch the bumps, as it can lead to unsightly and permanent scarring.
- Do not wear clothes that are too tight and made from fabrics that cling to your body because they rub against your sensitive skin and may cause flare-ups. Similarly, avoid coarse fabrics that can be too harsh on your skin.
- Avoid allergens that can cause eczema flare-ups or other such skin conditions that may trigger keratosis pilaris if not managed properly.
- Do not go for artificial tanning to camouflage your bumps as it will only make them more noticeable.
Most-Asked Questions About Keratosis Pilaris
Can dietary modifications help treat keratosis pilaris?

Keratosis pilaris cannot be cured, but you can take medication, try home remedies, and adopt self-care measures to ease its symptoms until it resolves on its own. Some dietary modifications may help in this regard, but there are no clinical trials to prove it. However, experts have explained how particular foods can help improve this skin condition.
Keratosis pilaris is associated with specific nutritional deficiencies such as vitamin A deficiency. (7) Ask your doctor about the nutritional deficiencies that could be a risk factor for this condition.
To meet all your nutritional needs, consume a diversified and well-balanced diet. If you fail to get enough of a particular nutrient through diet alone, ask your doctor to put you on a supplement.
As discussed earlier, certain dermatological disorders that cause intense skin dryness can potentially trigger or aggravate keratosis pilaris. This includes eczema, dermatitis, and ichthyosis vulgaris, among others, and diet plays a critical role in managing them.
If your keratosis pilaris is triggered by any such conditions, consider eating foods that are rich in omega-3, such as fish oil, zinc, magnesium, and vitamin D, as well as probiotics such as yogurt, kefir, and sauerkraut. (8) These foods help moisturize, repair, and protect dry, worn-out, sensitive skin and thereby prevent future flare-ups.
Plus, you must drink at least 8 glasses of water throughout the day to hydrate your skin from within. While these dietary tips may help improve your skin condition, you really cannot make your own diet plan until your condition has been properly diagnosed by a specialist.
Can diluted apple cider vinegar help remove the bumps caused by keratosis pilaris?
Some user reports suggest that applying diluted apple cider vinegar (ACV) over the bumps caused by keratosis pilaris may improve skin texture.
The idea behind it is based on the acidic property of the vinegar, which is claimed to dissolve the keratin plugs, reduce skin dryness, exfoliate skin buildup, and curb inflammation. So far, there is no scientific evidence to support these claims.
However, this topical remedy is quite popular among general users with no reported side effects. So, there is no harm in trying but only in the recommended concentration (1 part ACV in 2–3 parts water) and after conducting a patch test. If you experience even the slightest irritation, discontinue its use.
Can coconut oil, Moroccan argan oil, or olive oil help manage keratosis pilaris?

The answer to this question is controversial. The American Academy of Dermatology advises against using oil-based products to treat keratosis pilaris as the oil can further clog the hair follicles and worsen the condition.
However, some anecdotal evidence suggests that argan oil or olive oil may help nourish and moisturize dry, bumpy skin to give it a smoother finish. These lubricating oils are loaded with vitamin E and omega-3, which are both strong antioxidants that can help repair and protect your skin.
Some users have also reported positive results after applying coconut oil (preferably mixed with ACV) over the affected skin post exfoliation.
The best part is that all these oils are mostly safe for all skin types and therefore can be used by anyone. However, you must patch test them first on a small area of the affected skin just to rule out any possible side effects.
Once you do start using these oils, keep track of any signs of recovery or flare-ups to see how well your skin is responding to them.
Final Word
Fortunately, keratosis pilaris is not contagious, painful, or dangerous so you don’t have to get worked up about it. But if your keratin plugs or red bumps are making you uneasy or distressed or affecting your confidence, consult a dermatologist about it.
Your doctor will examine your condition and suggest a treatment plan accordingly. This may or may not include medication and clinical therapies. In many cases, simple home treatments combined with a proper skin regimen and self-care measures will go a long way in improving the appearance and texture of your skin and in minimizing flare-ups.
- Was this article helpful?
- YES, THANKS!NOT REALLY


