In this article:
The athlete’s foot belongs to a group of skin infections collectively termed as tinea and is caused by a dermatophyte fungus that lives on the surface of the skin.

This fungus thrives in warm and humid environments such as community swimming pools, locker rooms, and gyms, all of which are essentially places that are frequented by athletes. This is where the infection gets its name from.
Almost anyone can contract this infection, but there is an increased prevalence of athlete’s foot in men than in women.
Causes of Athlete’s Foot
Various strains of dermatophyte fungi are responsible for athlete’s foot, but most cases can be traced back to three species in particular, namely:
- Trichophyton rubrum
- Trichophyton interdigitale
- Epidermophyton floccosum (1)
The dermatophyte species live on or in the surface layer of the skin, or the epidermis, and generally thrive in warm, damp places, such as the sweat-prone area between the toes. It is precisely for this reason that people who perspire a lot are more vulnerable to this infection.
Athlete’s foot can be contracted through the following:
- The friction against footwear can result in injuries or cuts on your feet that give easy access to the infection-causing fungi.
- People who regularly wear closed shoes are also susceptible to this infection. Repeatedly wearing dirty socks can only make it easier for the fungus to gain access to your feet.
- People can contract athlete’s foot through direct or indirect contact with the skin of an infected individual.
- Athlete’s foot can also be contracted by coming in direct contact with the floors of communal pools, showers, and changing rooms, which are breeding grounds of the infection-causing fungi as these places offer favorable conditions for their proliferation.
Signs and Symptoms

The following symptoms usually accompany a typical case of athlete’s foot:
- The skin of your feet appears extremely dry.
- Itching and burning are felt between the toes, which may increase as the infection spreads to other parts of the feet.
- A red, scaly rash appears on the infected skin, usually spreading from between the toes to the insteps of the feet.
- Blisters may develop on the feet, which often peel or crack open when the skin is scratched, exposing small areas of raw, weepy tissue underneath.
- There is inflammation or swelling in and around the affected region.
- The infected foot may give off a foul smell.
Medical Treatment
Athlete’s foot is more or less a harmless condition that can be easily treated at home with over-the-counter lotions, creams, or sprays, preferably containing miconazole, clotrimazole, terbinafine, or tolnaftate. (2)
Follow the manufacturer’s instructions for the correct dosage and method of application. Generally:
- Clean your hands before and after every application.
- Dab or spray a tiny amount of the product onto the affected area.
- Massage the area gently until the product is absorbed.
- Repeat the application two to three times a day.
It is essential to continue using the cream, lotion, or spray for at least 2 weeks after your symptoms have cleared up to ensure that the fungus has been eradicated completely.
Severe cases of athlete’s foot may warrant a stronger treatment that goes beyond these preliminary over-the-counter options. Your doctor may prescribe antifungal pills or topical medicine to apply to your skin.
Diagnosing Athlete’s Foot
Most cases of athlete’s foot are diagnosed by way of a simple visual examination of the feet. Your doctor will most likely inquire about your other symptoms and take into account any history of fungal infections as well.
The doctor may also ask about symptoms present elsewhere on the body since other skin diseases can also exhibit similar symptoms as an athlete’s foot infection.
If the infection presents atypical symptoms or if the standard treatment fails to provide adequate relief, additional testing may be required, which involves the following:
- Using a scalpel with a blunt edge or a toothbrush, the doctor will gently scrape off a piece of the infected skin.
- This skin sample will be examined closely in the lab for the presence of fungi.
- If the result is a false negative, the second round of testing is done.
- After knowing the causative organism, the doctor will prescribe the appropriate treatment.
Risk Factors for Athlete’s Foot
The following factors can make you increasingly predisposed to an athlete’s foot infection:
- A genetic predisposition to the infection (other people in your family have had it)
- Preexisting allergies
- Other preexisting skin conditions such as eczema
- Particularly sweaty feet
- Blood circulation problems in the legs, often due to diabetes or constricted blood vessels
- Compromised immune system, due to a serious illness or the long-term use of certain immunosuppressive medication
- Active involvement in certain sports, especially running and swimming
Complications Associated With Athlete’s Foot
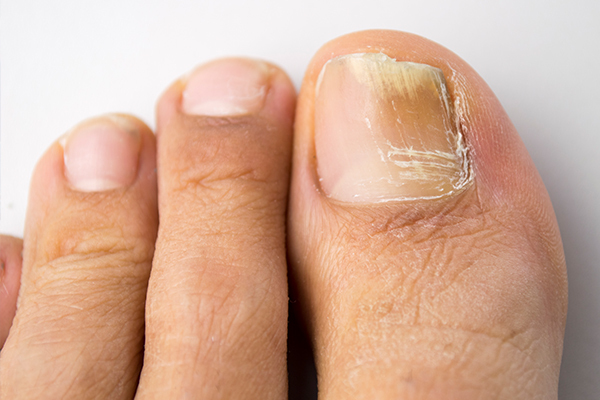
However benign this condition may be, an athlete’s foot must be treated timely to prevent the spread of infection and the complications that arise thereafter.
- If the infection is left to fester for too long, it can spread to the toenails, causing them to thicken and turn yellow. This kind of infection is far more stubborn and, consequently, harder to treat.
- Considering how contagious fungal infections are, an athlete’s foot can also escalate to a more widespread condition encompassing different parts of the body.
- You can get a bacterial infection from the constant scratching that can lead to life-threatening infection and possibly lose your leg.
When to See a Doctor
Most cases of fungal infections such as athlete’s foot often resolve themselves naturally provided proper foot care and hygiene are practiced.
However, if you fail to register any improvement in your symptoms despite routine foot care for more than 2 weeks, it is best to consult a podiatrist or healthcare provider.
Expert Answers (Q&A)

Answered by Dr. Hai-En Peng (Podiatrist)
Not usually. The odor could be a sign of another problem not necessarily related to the athlete’s foot.
It is a nice natural solution that can help, but it’s best to use it in conjunction with topical medication, not as a primary treatment.
It can help dry out the dampness and sterilize the affected foot. Please be sure to use the right amount.
There are many different types of effective topical creams, gels, and lotions that can help you get rid of athlete’s foot. Healing can be as quick as 2 weeks, depending on what medication your physician writes for you.
You can if you want. You don’t necessarily have to stop wearing socks if you have athlete’s foot. Just be sure to wash them well after use. The socks can also help the prescription medication get into the skin better.
Yes, it can. These blisters, if popped, are sterile, clear fluid.
We are an active society. We are constantly trying to lose weight and stay healthy, so we spend a lot of time in gyms and swimming pools.
The locker rooms are breeding grounds for fungi that cause athlete’s foot, so please help yourself by wearing protective footgear as you shower in the locker room area. When going swimming, use supportive sandals to protect your feet on the pool deck.
If you are into martial arts, yoga, or dance, if you can wear socks to protect your feet at the studio, then do so. If you can’t, then be sure to wash your feet when you get home.
You can never trust the habits of other people at the studio. Do not become overly obsessive about it, but be smart. If you do, you’ll be able to significantly lessen your chance of picking up athlete’s foot.
Final Word
If you ignore the athlete’s foot infection, it is more likely to spread from your feet to other areas of your skin such as your hands, groin, and scalp.
This complication usually results from poor hygiene practices, such as using a common towel to dry your infected feet and the rest of your body. Thus, the importance of timely treatment cannot be emphasized enough to contain the spread of this infection.

- Was this article helpful?
- YES, THANKS!NOT REALLY



