In this article:
Scars are a result of the natural healing process, and so they are usually nothing to be worried about. However, self-care measures and other remedies may help lighten the scars.

It is best to protect yourself from injuries and take proper care of your wounds to avoid scar formation in the first place.
Home Remedies to Treat Scars
You can help improve the appearance of scars at home using various commonly available ingredients.
1. Use onions

Onions are rich in medicinal compounds that stimulate the healing of a wound or injury.
A study demonstrated that the use of a 12% onion extract gel thrice a day could help reduce scar height and other scar symptoms post-operation. (1) Another study found that onion extract gels can safely improve the appearance of new scars by influencing their redness, smoothness, and softness. (2)
How to use:
Ground onions to a paste and apply topically to help reduce the formation of scars.
Summary:
Application of onion in the form of paste or extract-containing gels not only improves scars but also helps prevent scar formation.
2. Apply vitamin C
Vitamin C available in the form of topical oils and serums, can aid in the healing of scars. One study showed that the topical application of a silicone gel containing vitamin C could help improve fine scars on the facial skin of Asians. (3)
Another study demonstrated the safe and effective use of the hyaluronic acid sponge system along with vitamin C for scars older than 4 weeks, especially post-surgery. (4) You can also use lemon since it is rich in vitamin C antioxidants that help promote collagen synthesis. (5)
How to use:
Mix a tablespoon each of lemon juice, almond oil, honey, and milk and apply on the scar for 10 days.
Note: Discontinue the use of lemon if you experience a burning sensation or an allergic reaction.
Summary:
Vitamin C aids in the stimulation of collagen production, thus helping in the reduction of scars.
3. Massage with almond oil
Almond oil has a high content of vitamin E and fatty acid, which help in skin repair.
A study demonstrated the effectiveness of a 15-minute massage using almond oil during pregnancy in reducing the appearance of striae gravidarum. (6) Another study revealed that sweet almond oil helped relieve the itch associated with striae and prevented its progression. (7)
How to use:
Massage the affected area with almond oil at bedtime can help improve scar appearance. Besides, coconut (8) and olive oil can also be used to massage the scar. However, these are just anecdotal remedies, and therefore, should be used with caution.
Summary:
Almond oil has been shown to help inhibit striae development and therefore aids in preventing stretch marks.
4. Apply aloe vera

The use of aloe vera for healing scars is popular due to its anecdotal evidence. However, there is a lack of scientific proof. Aloe vera gel is known to provide nourishment and heal the skin, (9) thus suggesting its use for scar removal.
How to use:
Extract fresh aloe vera gel and apply it directly over acne scars for around half an hour before washing it with warm water. Repeat the remedy twice a day. Alternatively, you may mix aloe vera gel in your moisturizing cream and apply overnight.
5. Try honey
Honey has been long used as a therapeutic dermatological agent due to its antimicrobial properties. (10) While honey has been used anecdotally for treating scars, there is a need for more scientific studies to establish its efficacy. (11)
How to use:
Mix two tablespoons of honey with ¼th cup of oatmeal and apply on acne scars. Leave it on for 15–20 minutes and wash with warm water.
6. Use vitamin E
Vitamin E is popularly used for treating scars. However, it doesn’t have any supporting scientific evidence.
How to use:
Apply the contents of a vitamin E capsule directly over the scar or mix them in your moisturizing cream and apply.
7. Try essential oils
Different essential oils are used for dermatological purposes such as toning, reducing inflammation, soothing, and also as an antimicrobial agent. However, their use for treating scars lacks scientific evidence.
Anecdotally, lavender rosehip, tea tree, and frankincense essential oils have been used for massaging the scar tissue.
Note: Always dilute your essential oil by mixing a couple of drops in a carrier oil. Discontinue use if any adverse reaction occurs.
Self-Care Tips to Manage Scars
The following lifestyle changes and self-care methods can help reduce the appearance of the scars.
1. Use OTC creams, gels, or ointments
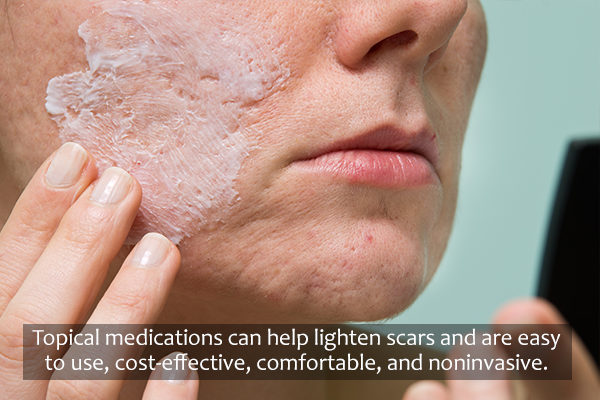
Topical medications can help lighten scars and are easy to use, cost-effective, comfortable, and non-invasive. These include imiquimod 5% gels and creams that help prevent or treat keloids. (12)
2. Try scar massage
Wearing a pressure appliance over the scar, generally, up to 6 months continually, stimulates collagen maturation and remodeling of the scar. It also helps reorient collagen fibers, improve pliability, and disrupt fibrotic tissue. (13)
3. Use silicone sheets or gels
These products create a waterproof seal over the scar to protect it from bacteria and dirt while maintaining a moist environment ideal for skin healing. A study found silicone gel to be effective in reducing scar texture by 86%, scar color by 84%, and scar height by 68%. (14)
4. Opt for a skin camouflage
Special makeup suitable for covering scars is readily available in pharmacies. This type of makeup is especially useful in covering facial scars.
5. Quit smoking
Smoking can interfere with the healing process and can worsen the scars. It is in your best interest to quit this habit.
6. Protect your skin from the sun
Damaged skin can discolor on sun exposure for up to 6 months post-injury. Therefore, avoid sun exposure while your skin is healing by covering the cut with clothes or using sunscreen after 2 weeks of the injury.
7. Exercise regularly
This helps prevent stiffness in the joints around the scar. Physiotherapy and exercise also release tensions arising from scar tissue and improve tissue perfusion, thereby relieving articular contractures. (15)
8. Exfoliate your skin
Gently exfoliating your skin with the help of a scrub or a face sponge can help remove the outer dead layer of skin cells, allowing the growth of newer, healed cells. You may consult your dermatologist to suggest the correct type of skin exfoliation for your scars.
Preventing Scars

Scar formation can primarily be prevented by avoiding injuries, wounds, and accidents. If an injury does occur, the following tips can help reduce the likeliness of scar formation:
- Keep the cut, injury, or scrape clean at all times.
- Apply an ointment to the wound immediately.
- Use a bandage to cover the wound.
- Change the dressing regularly.
- Use sunscreen after the wound is healed to help fade the scar.
While you can treat minor wounds or scrapes at home, it is recommended to get professional medical help if you have a deep or painful wound or if your skin is infected.
Final Word
While most scars fade over time, some may require treatment to help improve their appearance, including keloids and depressed acne scars.
However, the best measure is to prevent the formation of scars. This can be done by enabling proper healing, supported by the use of onions, vitamins C and E, proper wound care, and sun protection.

- Was this article helpful?
- YES, THANKS!NOT REALLY


