In this article:
Ice therapy can be an important intervention for soothing injuries that are accompanied by pain and swelling. Mild to moderate injuries can often be managed at home when the trauma only affects soft tissues.

Icing an injury is often combined with other therapies depending on the type and severity of the injury.
What Kind of Injuries Should Be Treated With Ice Therapy?
Ice therapy is typically used in the treatment of sudden traumatic injuries, sports injuries, overuse injuries, and muscle spasms.
Examples of acute injuries that may benefit from ice therapy include:
- Pulled or strained muscles
- Sprains (ankle, wrist, shoulder)
- Impact injuries limited to soft tissue (a jammed finger, bruised hip, facial traumas)
Ice therapy has also been used in the treatment of some types of chronic injuries. Repetitive motions and high-impact exercise can expose certain areas of the body to repetitive stress. These stressors can add up over time, resulting in painful injuries.
Those suffering from overuse injuries with repetitive flare-ups tend to have some relief with ice treatment. (1)
Examples of recurrent conditions that may benefit from ice therapy include:
- Tendonitis (jumper’s knee, tennis elbow)
- Recurrent ligament/joint inflammation (arthritis flare-ups)
- Shin splints
- Plantar fasciitis
- Other diagnosed “overuse” injuries
These injuries are typically soothed with ice therapy after performing activities that aggravate inflammation and pain in the affected area. (1)
When Can Heat Therapy Be Beneficial?
Previous research has included cold therapy, heat therapy, and pain medication in various combinations, making it difficult to attribute pain relief to one aspect of treatment. (2)
Stimulating nerves in different ways can help reduce pain perception, be it using heat or cold therapy, at safe temperatures.
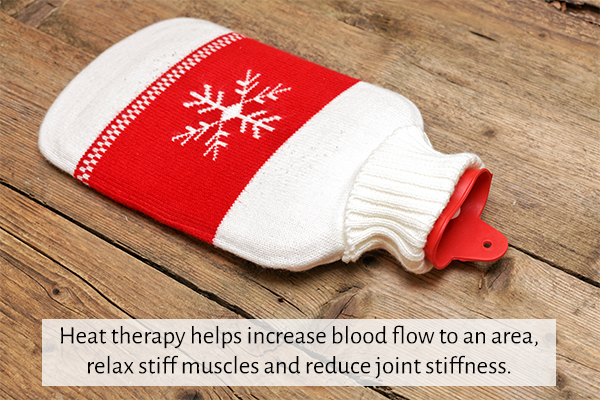
The goal of heat therapy is to increase blood flow to an area, helping relax stiff muscles and reduce joint stiffness. This treatment modality may be used as part of a treatment protocol for neck and back stiffness, muscle spasms, and decreased flexibility. (3)
You must wait 3 days or more after an injury for the initial swelling to subside before applying heat therapy. (3)
The Science Behind Ice Therapy
Icing lowers the temperature of the skin surface and the tissues underneath, causing the following effects:
- The temporary narrowing of blood vessels near the skin surface
- Slow pain signaling from the nerves (4)
- Slow transport of molecules that promote inflammation (1)
However, there still isn’t enough evidence to support the application of ice in clinical therapy. Recommendations are based on observations that ice therapy, as part of the initial treatment for swollen and painful injuries, provided benefits. (5)
Make Your Own Ice Pack at Home

There are many easy ways to make an ice pack. For a comfortable ice therapy session, choose an option that is easy to hold over the desired area.
You can do any of the following:
- Place a handful of ice cubes or crushed ice in a plastic bag and then wrap it with a thin towel or cloth.
- Reusable options, such as freezer gel packs or refillable ice bags, work just as well.
- Ice massage is another popular method among athletes, which requires a few small paper cups, water, and a towel. Fill each cup with water and freeze. Once the ice is frozen, the paper rim can be peeled away to expose a small amount of the ice, which can be gently massaged onto the soft tissue injury for a short duration. Keep peeling the paper cup to expose more ice as needed. Continuously move the ice to avoid contact with one area of skin for too long.
How Does Ice Therapy Work?
Using ice therapy within the first 2–3 days of injury is recommended for the reduction of swelling. The application of cold temperature at the site of injury temporarily numbs the nerves in the area, reduces blood flow to the site, and slows down the signals that promote inflammation beneath the skin’s surface.
Based on the current evidence, it is unclear what negative long-term effects ice therapy may have on the growth of muscle fibers and blood vessel branches after the injury has resolved. (2)
Proper Way to Ice an Injury
It is advisable to apply ice therapy as soon as possible after an injury. Several sessions of ice therapy can be applied with plenty of rest in between for the first 2–3 days. This is when swelling and inflammation is most likely to develop.
Avoiding direct contact with the skin is the easiest way to avoid skin damage or frostbite. Depending on your cold tolerance, ice can safely be applied for short periods using an ice pack. Generally, 10–20 minutes of continuous ice therapy can be followed with an hour or more of rest.
How Long Should You Ice an Injury?
Experts recommend icing an injury repeatedly during the first 2 days of its occurrence, for no more than 20 minutes at a stretch at an interval of 2–3 hours.
Individual responses to cold are unique, and some may be more sensitive to changes in temperature than others. Once an area begins to feel numb, the ice can be removed to allow for rest and recovery. Prolonged periods of numbness are undesirable and should be avoided.
Paying attention to how the area feels can signal when it is time to end an ice therapy session. If the tissue starts to feel numb before the set time to end the session, take a break early to allow blood to flow back to the area.
Key Mistakes to Avoid When Icing an Injury

Ice therapy will only work if done correctly, or else it can worsen the damage. Here’s what you need to avoid:
- Icing for too long: Prolonged exposure to cold temperatures can cause long-term damage to the skin and deep tissues. Try ice therapy in multiple short sessions of 10–20 minutes with a period of rest in between to allow blood to flow back into the area. (6)
- Forgetting to protect the skin: Directly applying ice to one area of skin for too long can lead to skin damage or frostbite. Thus, always wrap the ice in a thin towel or cloth to protect the skin from direct exposure.
- Restarting activity too soon: Resting the area can play an important role in recovery. It is important to avoid overexerting an injury immediately after ice therapy sessions and during the recovery period.
Ways to Prevent Skin Damage Due to Icing
Ice therapy can have unintended consequences if steps are not taken to protect against additional injury. Precautions to avoid frostbite and recognize complications early are essential for safety. If severe, frostbite can permanently damage skin and tissues.
A few simple steps can prevent overexposure to cold temperatures while using ice therapy:
- Monitor the length of ice sessions.
- If using an ice bag or pack, reposition it periodically.
- If using an ice cup, use the ice massage technique in short sessions.
- Monitor the appearance of the skin for changes.
- Discontinue ice sessions when numbness begins.
- Make sure to rest immediately after ice sessions.
- Do not overexert an injury after applying ice.
Signs of Skin Damage Caused by Ice Therapy
Prolonged or direct exposure to freezing temperatures can deeply damage the skin and even result in frostbite. Discontinue ice therapy if you notice any of the following signs:
- Redness, along with feelings of tingling and numbness in the affected area, occurs.
- The treated skin begins to lose its color.
- Calluses appear at the site of application.
People Who Should Avoid Ice Therapy
People diagnosed with Raynaud’s disease, peripheral neuropathy, or any condition that compromises nerve sensation or blood circulation are susceptible to accidental injuries from overexposure to ice and, therefore must exercise extra precautions.
Discussing your symptoms and medical history with a medical professional before starting ice therapy can help determine if ice therapy is appropriate.
Injuries That Require Medical Attention
If the injury occurred more than 2 days ago, ice therapy might not be an effective treatment.
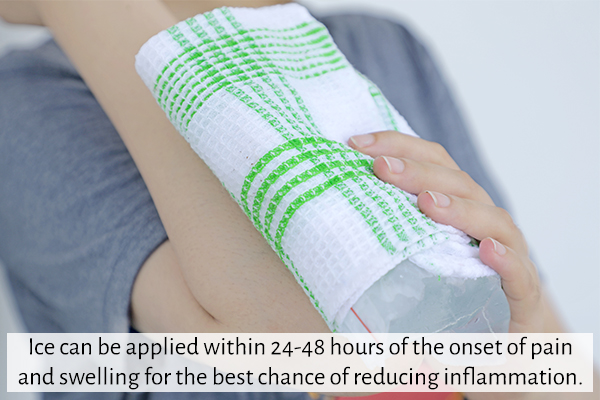
Ice can be applied within 24–48 hours of the onset of pain and swelling for the best chance of reducing inflammation. If your symptoms don’t improve after 2 days of icing your injury may be a serious one that needs medical attention.
Injuries that affect the underlying bone may require X-rays to check for potential fractures. The area around a broken bone or dislocated joint might look misshapen or deformed. However, changes in appearance may not always occur. (7)
Persistent swelling, worsening pain, or difficulty with movements may indicate a need to reach out to your doctor for evaluation and treatment.
Final Word
Ice therapy has long been used to dull pain and reduce swelling after acute injuries. However, more research would strengthen the scientific basis for recommending ice therapy as a treatment.
Applying ice within the first days of injury, taking reasonable precautions, and allowing the area to rest can help make ice therapy a beneficial part of recovery.
- Was this article helpful?
- YES, THANKS!NOT REALLY


