In this article:
Arthritis refers to joint inflammation that induces pain and stiffness in the affected areas. Certain lifestyle changes can help prevent joint damage, control pain, and help you stay active. Consult your doctor for an appropriate diet and lifestyle plan.
Home Remedies for Osteoarthritis
These are some at-home treatments that help subside the symptoms of osteoarthritis (OA).
1. Apply warm and cold compresses
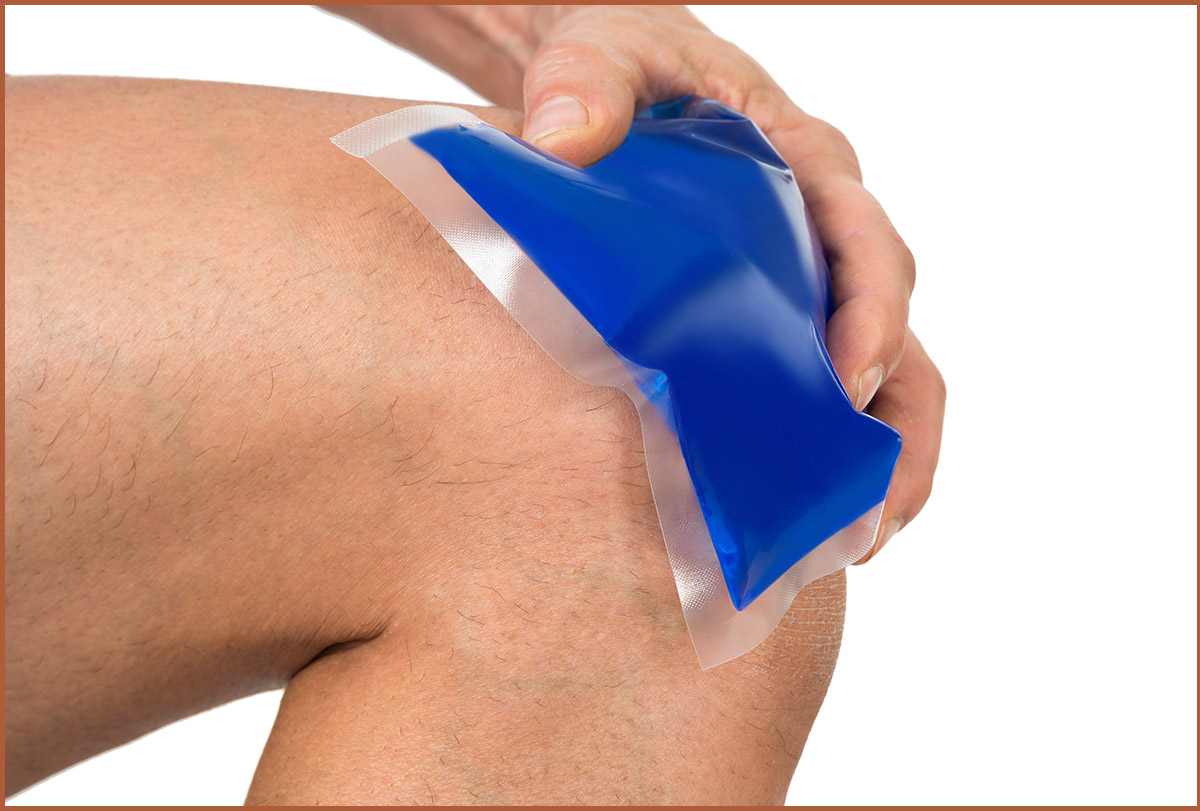
When you apply a warm compress over the joint, the heat penetrates through the skin to relax the tense muscles underneath. Heat also helps improve the range of motion in the joint.
Cold therapy works by shrinking the underlying blood vessels to limit the flow of blood to the joint area, helping subside the swelling. It also helps numb the area temporarily, making you feel less pain. (1)
2. Use turmeric
Turmeric is a potent anti-inflammatory agent that can help subside the pain and swelling associated with arthritis. (2)
How to use:
- Prepare “golden milk” by mixing turmeric, cinnamon, ginger, pepper, and maple syrup in a glass of warm milk and consume.
- Add turmeric to your meals as a spice.
- Take turmeric supplements upon consulting your doctor.
3. Consume garlic and ginger
Both garlic and ginger possess antioxidative and anti-inflammatory properties, (3)(4) which help in preventing and subsiding the swelling of joints, as seen in OA.
How to use:
- Use ginger and garlic as spices in your meals.
- Ginger can be consumed in the form of ginger tea daily.
- Ginger is also available in the form of powders, oils, capsules, and tinctures.
4. Take an Epsom salt bath

Epsom salt contains magnesium that can help reduce the pain and inflammation associated with OA. (5)
How to use:
Add 2 cups of Epsom salt in your warm bathwater. Salt baths should not exceed 30 minutes at a time.
5. Apply capsaicin
Topical capsaicin has a good safety profile and efficacy in reducing OA pain of the hand, knee, hip, or shoulder when applied three to four times a day. (6)(7)
Note: Make sure to wash your hands after each application to prevent exposure to the eyes.
6. Consume apple cider vinegar
Apple cider vinegar is an anti-inflammatory agent. However, there’s no human trial to support its use in treating OA.
How to use:
Dilute 1 tablespoon of ACV in a glass of warm water and consume daily.
Alternative Treatments for Osteoarthritis

Various alternative treatments and therapies can help in the symptomatic management of OA.
1. Massage therapy
A study found massage therapy to be a safe and effective short-term treatment option, particularly for people with knee OA. (8)
If you are not confident about the proper technique, you can get it done by a licensed therapist at a spa. Please consult your physician to make sure massage therapy will be safe and effective for you.
Additionally, certain analgesics can be massaged into the skin for greater symptomatic relief. These include peppermint oils and other menthol-containing gels or sprays.
Menthol decreases nerve activity and the transmission of pain signals. Also, the cooling effect can restrict blood flow to the joint tissue and thereby reduce swelling. (9)
2. Acupuncture
Acupuncture is a traditional Chinese technique that involves the insertion of needles in specific points of the body to heal various maladies. This alternative therapy may help alleviate the symptomatic discomfort associated with OA and improve joint mobility when performed by a trained specialist.
3. Hydrotherapy
Hydrotherapy combines the double benefits of heat treatment and light resistance exercise, both of which can help relieve the pain and stiffness in your arthritic joints. (10)(11)
The therapy involves performing gentle forms of exercise in an aquatic setting. The pools used for hydrotherapy are filled with warm water, which helps soothe your body and decrease the pain and stiffness in and around the joints. Please consult your physician to make sure hydrotherapy is safe and effective for you.
4. Occupational therapy
Occupational therapy is a multifaceted treatment that helps people with physical, cognitive, or sensory impairment to regain full control over their daily lives.
This kind of supportive care is provided by trained specialists who identify the strengths and weaknesses of individual patients and then design a rehabilitation plan accordingly.
Occupational therapy involves a combination of different treatment interventions to maximize the flexibility of the joints, from rehabilitation exercises to the performance of everyday tasks. (12)
Self-Care Tips for People With Osteoarthritis
Here are some of the things you can do to help manage OA.
1. Exercise daily

Leading a sedentary life will diminish your muscle strength and render your joints stiffer than before.
While rigorous or heavyweight exercises are to be avoided, it is important to practice light stretching and strengthening exercises regularly to keep your joints limber. Besides, a carefully designed exercise plan can also inhibit OA progression. (13)
Exercise therapy that includes a mix of muscle-strengthening, flexibility, and aerobic exercises is preferred over general physical activity to address the pain and disability associated with OA. (14)(15)(16)(17) Exercise also helps keep your weight under check, which is essential for controlling the symptoms and progression of OA. (18)
Here are a few exercise options to help manage OA:
- Do 30 minutes of aerobic exercises, such as walking, biking, or swimming, at least five times a week.
- Try gentle weight training and resistance training a few times a week to enhance your muscle strength.
- Give 30 minutes of your day to range-of-motion exercises to retain the flexibility in your joints.
Note: People with OA should refrain from participating in high-impact sports to avoid the risk of injury.
2. Manage your weight
People who are obese or overweight are inherently more prone to joint damage, as the body load falls on the skeletal junctures. (19) Weight loss can help relieve the pain and other discomforts associated with OA by reducing the burden on your joints. (20)(21)(22)
3. Modify your diet

A healthy diet is an important part of OA management. People with OA can benefit from increasing their intake of the following:
a. Vitamin D
Vitamin D is one of the most important bone-building nutrients, and therefore, its deficiency can accelerate the progression of OA. (23)
b. Vitamins C and E
Foods that are replete with vitamins C and E can help strengthen your bones and reduce joint inflammation.
c. Omega-3 fatty acids
The consumption of omega-3 fatty acids may help reduce the inflammation and pain caused by OA. These foods include:
- Seeds such as chia seeds and flaxseeds
- Nuts
- Cold-water fish, such as salmon, trout, sardines, and mackerel
- Other seafood such as shrimps and oysters
d. Antioxidant and anti-inflammatory foods
Brightly pigmented fruits and vegetables, such as carrots, cantaloupe, and broccoli, are usually loaded with antioxidants and can be a great value addition to your diet.
e. Unsaturated fats
These are the good kind of fat, which can be included in your diet. Some good dietary sources of healthy fats include:
- Vegetable oils such as canola, corn, and sunflower oils
- Nuts such as walnuts and almonds
- Seeds such as sesame seeds, chia seeds, and flaxseeds
- Fatty fish such as mackerel and salmon
- Fruits such as olive and avocado as well as their oils (24)
The Mediterranean diet
The Mediterranean diet has all the makings of a healthy eating plan for patients with OA, a claim that has also been substantiated by research. It is recognized as an anti-inflammatory diet since it emphasizes the intake of foods that fight inflammation while limiting those that induce it.
Anti-inflammatory foods that form the crux of this kind of healthy eating include:
- Locally grown fruits and vegetables
- Fatty fish
- Whole grains
- Healthy fats such as olive oil and canola oil
- Select dairy items such as yogurt
- Nuts
- Wine
- Berries
Meanwhile, the consumption of pro-inflammatory foods such as red meat, sugar, and most dairy products is kept to a minimum. (25)
4. Take supplements
If you are unable to meet your daily nutritional needs through diet alone, you may consider taking nutritional supplements but only after consulting your doctor first.
There is some preliminary evidence that favors the use of the following supplements for improving OA symptoms:
- Avocado/soybean unsaponifiables (ASU), which are supplements made from avocado oil and soybean oil extracts (26)
- Nutritional supplements such as glucosamine and chondroitin sulfate
- Ginger supplements (27)
However, further research is needed to establish these claims.
5. Get adequate rest

Restful sleep is one of the best stress busters and is an essential requisite for proper OA management. Increased stress is one of the prime contributors to the onset of OA and can also accelerate the progression of the disease.
So, make sure to follow a regular sleeping schedule and get enough hours of shut-eye every day. A well-rested body is better equipped to cope with the pain and stress of OA. It is also important to balance activity with rest. Take multiple breaks in between periods of activity, and quit the task the minute it feels exhausting.
6. Practice mindful relaxation techniques
Living with pain can negatively impact your emotional and mental well-being, which can make the fight against OA even harder. Thus, you must make a concerted effort to maintain a positive outlook.
Relaxation techniques such as meditation, listening to soothing music, or engaging in any activity that you find pleasurable can help distract you from the pain.
7. Use assistive devices and orthotics
Doctors often recommend assistive devices to patients with OA. These devices mainly serve two purposes:
- Reduce the stress on your joints
- Protect your joints from further damage
Since OA majorly targets the knees and can make walking increasingly painful, you can use a cane or a crutch for body support.
Your doctor may advise you to wear tape, braces, or splints over the affected joint to hold it in a proper position. However, there isn’t enough research-based evidence to conclusively establish the effectiveness of these assistive devices. (28)(29)
Most-Asked Questions About Osteoarthritis
What is the difference between osteoarthritis and rheumatoid arthritis?
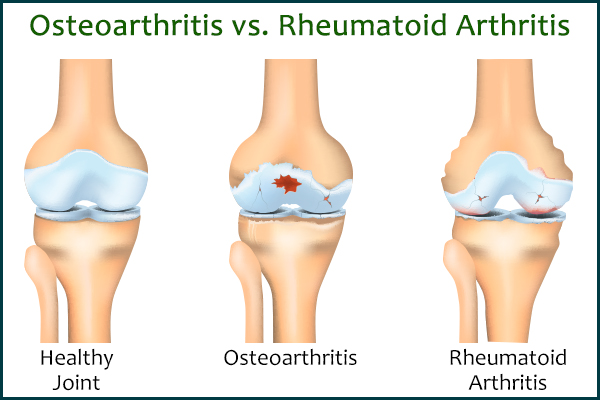
Even though both OA and RA target the joints and share some common symptoms, they are brought on by different causes.
OA occurs due to the mechanical degeneration of the joints, whereas RA is an autoimmune condition wherein the body starts attacking the healthy joint tissue. RA can begin at any age, but OA is more common in older adults.
What is the difference between osteoarthritis and osteoporosis?
Unlike OA, which is caused by the progressive breakdown or thinning of the cartilaginous cushion in the joints, osteoporosis is a bone disease characterized by decreased bone density.
Can you reverse osteoarthritis?
You can maintain or improve joint function through proper medication, physical therapy, diet, and lifestyle changes, but the problem may not go away completely. Surgical treatment can reverse the OA in certain cases in the right candidate.
Final Word
While osteoarthritis cannot be cured, various treatment methods can aid in symptomatic relief. It is vital to modify your lifestyle and diet for a healthy and normal life. It is best to consult a therapist for the exercises that help improve joint mobility and reduce pain.

- Was this article helpful?
- YES, THANKS!NOT REALLY


