In this article:
When it comes to oral health, most of us think it’s limited to have clean and white teeth with no cavities. But just as important as flashing a set of pearly whites is maintaining the health and integrity of the gums that protect the roots of your and teeth and hold them in place.

In the absence of proper care, your gum tissue is likely to wear away, making your teeth ultrasensitive and prone to damage.
The gingival tissue contains a moist mucous membrane that is densely packed with blood vessels. This pinkish layer of protective tissue runs over the underlying bone tissue of the upper and lower jaw, forming a barrier between the fragile base of the teeth and invading bacteria or decay-causing plaque.
So long as the jaw bone remains intact, the gums continue to be securely affixed and cover the teeth’s roots and the enamel up to the neck.
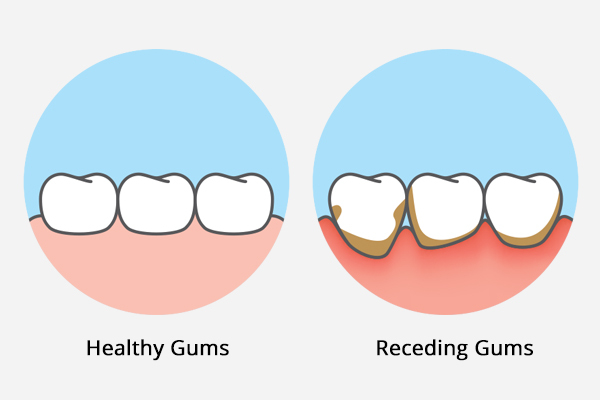
Gum recession, or gingival recession, means the margin of the gum tissue that surrounds the teeth, pulls back exposing more of the tooth or the tooth’s root.
The recession of the gum margins opens up small “pockets,” or spaces, between the teeth and gum line, making it easy for disease-causing bacteria to accumulate and granting them easy entry into the bloodstream.
The damage can spread to the adjoining tissue and bone structures of the teeth, severely hampering their integrity and ultimately resulting in tooth loss.
Causes of Gum Recession
Several factors lead to receding gums, including the following:
- The primary cause of receding gums is periodontal diseases, which are essentially inflammatory bacterial infections that ravage the connective gum tissue and bone structure that hold the teeth in place. (1)
- Many people are naturally predisposed to this condition due to genetic factors that make their gingival structure more susceptible to recession, regardless of proper oral hygiene.
- Aggressive tooth brushing with a hard-bristled brush and overbrushing can cause enough wear and tear to your gums for a recession to set in. (2)
- People with attenuated gum tissue due to dental treatment or those naturally born with thin gums are more vulnerable to gum recession.
- Plaque buildup due to insufficient dental care can result in gingivitis or gum inflammation, which paves the way for periodontitis and eventually gum recession. (3)
- Ongoing hormonal changes in the body, particularly in women undergoing puberty, pregnancy, and menopause, can render the gums increasingly sensitive and prone to recession.
- Gum recession can also occur as a result of traumatic injury to the tooth/teeth.
- Crooked and crowded teeth or a misaligned bite can put excessive pressure on the gums and supporting bone structure and can render the jawbone inadequate in providing enough cover to one or more teeth.
- Nutritional deficiencies are also associated with gum recession. For instance, a lack of dietary vitamin C results in a disease called scurvy, which is often associated with such gingival complaints. (4)
- Improper flossing techniques can cause gingival cuts and subsequent recession. (5)
- Use of tobacco products results in the accumulation of sticky plaque that is harder to get off the teeth and adversely affects the mucous membrane lining.
- A tendency to grind or clench your teeth, also known as bruxism, can exert undue pressure on the teeth, causing the gingival margins to pull back.
- Lip piercings or tongue jewelry can rub against the gums and cause them to wear away over time.
Signs and Symptoms of Gum Recession
Gum recession is a common problem and many people are not even aware of it. Some of the initial indicators of gum recession include:
- Tooth sensitivity
- A tooth that looks longer than normal
- Pain emanating from the gum line
- Loose teeth, because the damaged gums cannot hold them in place any longer
- Swollen and tender gums
- Bleeding from the gums after brushing or flossing
- Bad breath (6)
Standard Treatment for Receding Gums

The dentist will conduct an oral scan and determine the extent of gum damage before laying down an appropriate course of treatment. Once the dentist has pinned down the culpable cause of your condition, he/she will prescribe a customized treatment approach.
- If aggressive or incorrect brushing techniques are causing your gums to pull back, your dentist will give you a personal tutorial regarding proper brushing techniques and recommend oral hygiene care tools and products that can help in your case. (7)
- If gum recession is rooted in some periodontal disease, the ideal approach to prevent further damage involves getting your teeth thoroughly cleaned via root planing or scaling. (8)
- Because the exposed roots of the afflicted tooth render it highly sensitive, the dentist can prescribe desensitizing and dentin bonding agents as well as varnishes to make the nerve symptoms bearable.
- Removable gum veneers made of either acrylic or silicone are used to artificially camouflage the lost gum tissue area. (9)
- Orthodontic treatment may be used to rectify and realign the gum margin by gradually repositioning the teeth over time.
- Pink porcelain or composite are employed to fill in the gaps that develop along the gumline. (7) Similarly, a dentist may use tooth-colored composite resins to cover the exposed root of the tooth and close the pockets of space that open up between the teeth.
Risk Factors Associated With Gum Recession
- If thin or weak gums run in your family, you can inherit this characteristic via genes and you are likely to be more susceptible to gingival tissue loss.
- People who smoke cigarettes and use other tobacco products, show a greater tendency to develop this condition.
- Gum recession is a scourge that particularly affects the elderly, making age one of its prime risk factors. According to the Journal of American Dental Association, an overwhelming 88% of people above the age of 65 experience a receding gum in at least one tooth.
- People with diabetes have also been found to be increasingly prone to this problem. (10)
Final Word
Unlike other tissues in your body such as the epithelial skin tissue, your gingival tissue is not capable of regenerating on its own. Thus, once the gumline starts to recede, there’s no natural way to restore the lost tissue.
Most of the standard treatment approach for receding gums thus aim at halting or delaying the progress of this condition. In extreme cases, however, the dentist may prescribe a surgical intervention to help restore your gums by grafting tissue from another site in the mouth.

- Was this article helpful?
- YES, THANKS!NOT REALLY


