In this article:
Your spinal column consists of 33 small irregular bones called the vertebrae. These bones interlock with each other to form a complex but flexible cylindrical structure.

The spinal cord runs downward through the hollow center of this cylindrical column with nerve roots growing from it like branches. These nerve roots pass between the intervertebral spaces to exit the spinal column and spread out to the rest of the body.
It is because of these highly sensitive spinal nerve roots that your body can move and feel. If, however, the nerve root becomes compressed or twisted under the load of the vertebral bones, it can give rise to a lot of pain in the surrounding region.
The backbone extends from the neck to the hip and is divided into three primary sections: cervical, thoracic, and lumbar.
The nerve roots in the cervical section correspond to the neck region, the thoracic section to the chest region, and the lumbar section to the lower back region.
Damage to the nerve roots in any of these three sections is known as radiculopathy or a pinched nerve, which is associated with a great deal of discomfort and lack of function in the affected region. For instance, the pinching of a lumbar spinal nerve leads to back pain that radiates to the buttocks and legs, whereas damage to the cervical nerve roots causes shoulder and arm pain.
This article focuses on the causes, symptoms, and treatment of lumbar radiculopathy and tells you how to deal with the discomfort caused by a pinched nerve in the hip.
Causes of a Pinched Nerve
The basic cause of lumbar radiculopathy is spontaneous entrapment of the nerve caused by some pressure from the surrounding anatomy. Some identified specific causes include:
- Surgery on the hip, pelvis, or lumbar spine
- Large abdomen with a fat apron
- Pregnancy
- Increased abdominal pressure from fluid collection
- Tight belts or waistbands
- Compression from carrying a wallet chronically
- Prolonged leaning against an object (table or bench)
- Carrying heavy objects supported by the thigh or groin
- Long-distance walking/cycling/circuit training
- Trauma to the groin or lower back
Symptoms of a Pinched Nerve
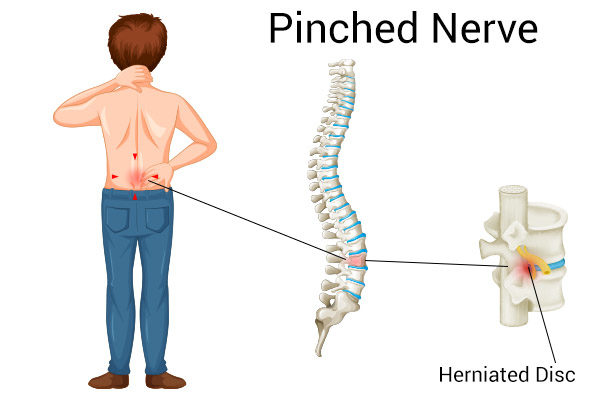
The most common syndrome of hip pain caused by a pinched nerve is due to the compression of the lateral femoral cutaneous nerve. The lateral femoral cutaneous nerve travels from the back of the pelvis and through the hip region. The symptoms of impinging this nerve include:
- Sharp pain is felt in the lower back that may travel through your buttocks, down the legs, all the way to your foot.
- The pain is often described as a burning, stinging, or “pins and needles” sensation.
- The pain tends to be present at all times and in most positions, but it is aggravated by even a light touching on the skin or specific activities, such as sitting down or coughing.
- The pain is usually accompanied by numbness and tingling over the hip and outer thigh on the affected side of the body.
- You may also experience itching, weakness, and diminished reflexes in the affected region.
It is not necessary for you to experience all of these symptoms for it to be a case of lumbar radiculopathy. (1) In some cases, these symptoms may disappear completely, but that does not mean the problem has been resolved.
On the contrary, it could indicate worsening of the condition wherein the nerve becomes so completely compressed that it loses all its functionality. Thus, the sudden loss of feeling in the affected site may lead to the disappearance of pain, but it can also trigger more serious complications later.
The overwhelming pressure on the nerve not only compromises its own function but can cause loss of muscle activity as well. Thus, the severity of your symptoms alone does not indicate how serious your problem is.
Medical Treatment
Lumbar radiculopathy is self-limited and benign in 90% of patients. The pain can last for weeks to months, and the majority go away on their own. The pinched nerve heals as the compression on it is reduced. Hence, decreased pain and numbness indicate that healing is in process.
Stress is not known to cause this condition and there is no evidence that heat helps (although it cannot hurt to try it).
Your doctor will evaluate your symptoms, medical history, and other relevant factors before prescribing the appropriate treatment, which may involve a combination of therapies.
1. Surgery
Should the pain persist, surgery for nerve decompression or nerve transection (removal of a nerve segment) may be necessary. Of all the medical interventions, surgery, traction, and corticosteroid were found to be the most effective for long-term pain relief. (2)
2. Nonsurgical interventions
- Many patients may find relief from taking OTC anti-inflammatory medications such as ibuprofen, aspirin, or other such NSAIDs. You can even take nonprescription pain meds such as Tylenol. But always check with your doctor before starting any medication to know about its safety and correct dosage.
- Anticonvulsants, which act on nerves, may also be used (Dilantin, Neurontin).
- If the pain is persistent, an injection or nerve block procedure by an anesthesiologist may be warranted.
Diagnosis
Pinched nerves are commonly diagnosed on examination. Your physician will perform a number of diagnostic maneuvers that are guided in the context of your personal medical history, looking to identify and rule out the most dangerous potential causes.
With a straightforward diagnosis of a pinched nerve, the exam will show a loss of light touch or pinprick sensation in a discrete area of the upper lateral thigh. The neurologic changes will likely be sensory (feeling) and not motor (ability to move).
Doctors may choose to order a nerve conduction study to further support the diagnosis in addition to other tests and imaging (MRI) if the physical exam is not entirely conclusive. (3)
To gauge the nerve function in the affected region, doctors sometimes use a neurologic test called an electrodiagnostic study or EMG/NCS. This procedure involves the insertion of small needles in the muscles of the area where the symptoms can be felt.
The needles transmit electrical discharges that can help study the underlying nerve activity in the area. This enables the doctor to trace the pain to its source and thereby identify the pinched nerve.
Self-Care Measures

Here’s what you can do at home to ease the pain:
1. Proper clothing
At home, patients may find relief by wearing loose/non-binding clothing.
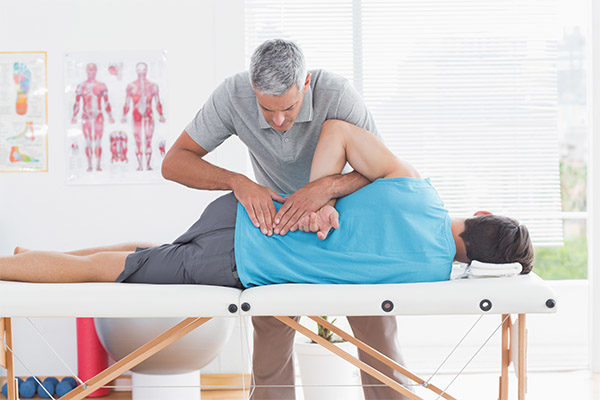
2. Massage
Massage may help relax the muscles and nerves in the area and thereby ease the pain to some degree, but the evidence to support this claim is not very strong.
3. Lifestyle changes
The best lifestyle changes are the ones that improve risk factors, namely, diabetes and obesity. A healthy weight loss diet, appetite control, glycemic control, and proper posture are essential for both preventing and relieving this problem.
4. Physical therapy
Abdominal toning, weight loss, and back strengthening exercises can help take the load off your spine and ease symptoms. You must also make concerted efforts to correct your posture and avoid certain positions to minimize the pressure on your back and spinal nerves.
5. Cold therapy
Applying an ice pack or any kind of cold compress on the affected site can help with pain relief by temporarily numbing the underlying nerves. But never apply the ice directly as it can cause undue skin damage.
6. Relaxation
You can engage in meditation and other relaxation activities to ease the tension in your body.
Risk Factors
The most commonly identified risk factors for lumbar radiculopathy include:
- Obesity
- Diabetes
- Advanced age
The median age of presentation is 50 years old. Interestingly, the incidence is sevenfold higher in diabetic patients than in the general population.
When to See a Doctor
Seek prompt medical assistance if:
- You are experiencing severe out-of-proportion pain.
- You have a fever.
- You have numbness in the groin characterized by an inability to control urine or feces.
- You have paralysis in any part of the body.
Ask your doctor what his concern is while knowing your medical history. Ask what other diagnoses he is considering.
Your doctor will ask you about recent travel, history of trauma, change in medications, if you have a fever or neurological signs, if the pain wakes you up in the night, if the pain is associated with any other symptoms, if you have had surgery, and other questions.
Final Word
A pinched nerve in the hip is usually benign and will go away on its own. There aren’t many therapeutic options once it has been diagnosed. The best way to prevent it is to avoid obesity and diabetes.
- Was this article helpful?
- YES, THANKS!NOT REALLY


