In this article:
An oral mucocele refers to a harmless and painless mucous cyst in the oral cavity. It is a non-malignant tumor typically clear in appearance.
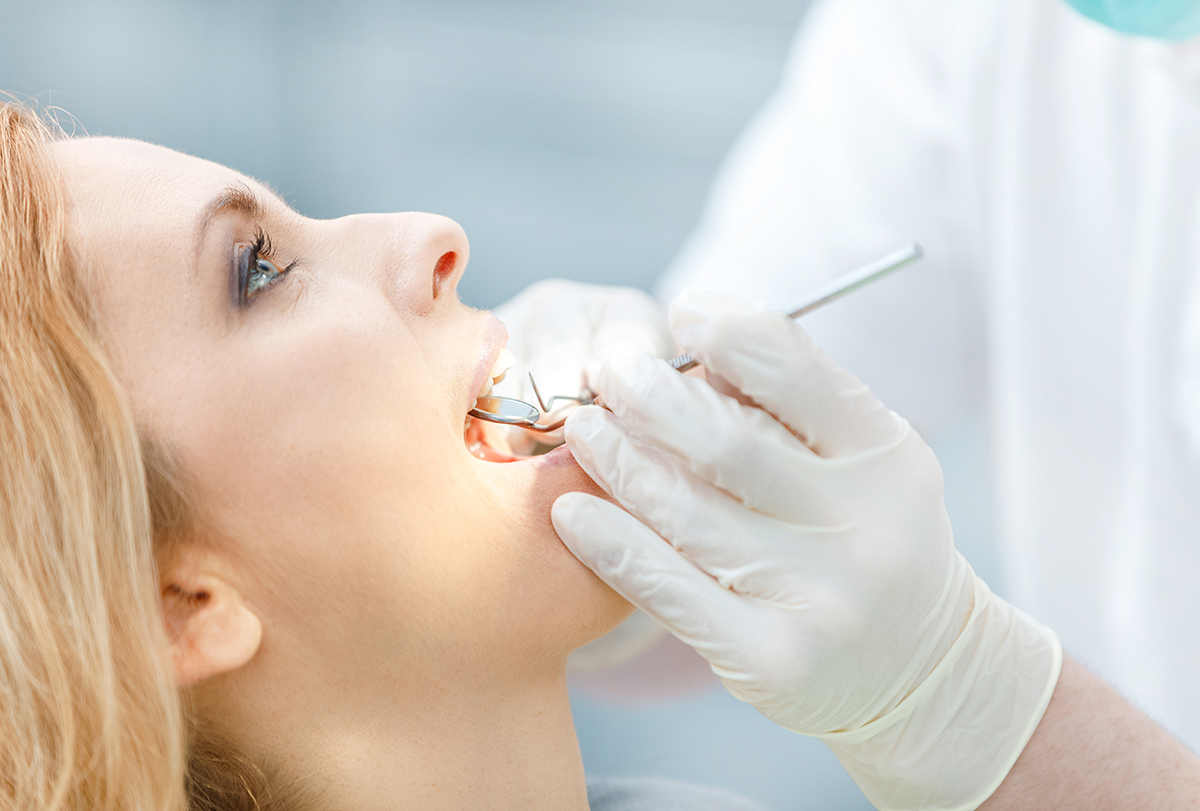
These fluid-filled lesions usually develop due to damage to the ducts of the minor salivary glands.
Formation of a Mucocele
The mouth contains multiple salivary glands which secrete a protein called mucin. This protein combines with water to form a slimy substance known as mucus.
Minor trauma to these salivary glands often causes spillage and pooling of this secretory fluid in the surrounding subepithelial tissue. As the mucus builds up in the tissue, the affected site becomes inflamed and a fluid-filled nodule appears within a few days.
This mechanism is referred to as extravasation and is often observed in cases of accidental biting of the tongue or the soft connective tissue lining the inner mouth. (1)
A mucocele may also take shape if your glandular ducts become plugged or blocked with mucus. Any obstruction in the salivary gland will hamper the secretion of saliva and result in the buildup of mucus within the subepithelial tissue surrounding the affected gland.
This mechanism is referred to as retention, which is often responsible for the occurrence of mucoceles. (1)
Where Do Mucoceles Appear?
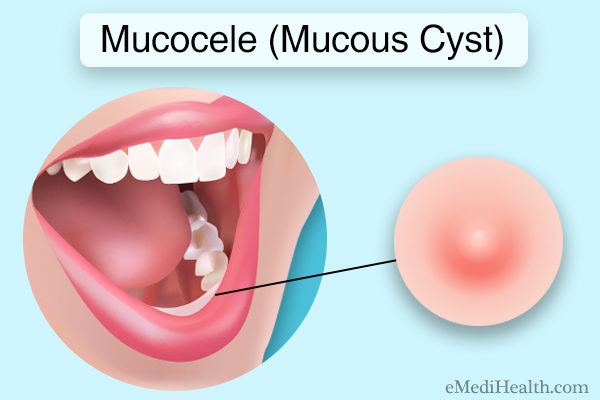
A mucocele can develop anywhere inside the oral cavity where a minor salivary gland may be present, but the usual sites of occurrence include:
- The lower lip, which is the most commonly affected (2)(3)
- Under the tongue (2)
- The buccal mucosa or the inside of the cheeks
- The gums
- The floor of the mouth (mucoceles in this area are sometimes referred to as a Ranula)
Different Types of Mucocele
Mucoceles are broadly divided into three categories depending upon their location:
- Superficial mucoceles: Which lie close to the surface and develop under the mucus-secreting epithelial tissue or the mucous membrane lining the oral cavity
- Classical mucoceles: Which form in the deeper layer of connective tissue known as the upper submucosa
- Deep mucoceles: Which are located in the lower corneum
Causes of a Mucocele
To reiterate, oral cysts are by and large the result of some trauma to the salivary glands. Some of the most common causes of the development of oral mucoceles are as follows:
- If you are in the habit of biting or sucking on your lips or inner cheek, especially when under stress, there is a good chance that such abnormal oral habits will end up damaging or clogging your glandular ducts.
- Excessive smoking can cause chronic irritation to the oral tissue, leading to the development of mucous cysts in the mouth.
- Eating scalding hot food can subject the soft connective tissue inside your mouth to extreme heat, which can result in the appearance of mucoceles.
- Misaligned teeth or abnormal teeth growth can also compress the adjoining oral tissue and pave the way for oral cysts.
- Getting your lip pierced can injure your salivary gland, which can result in the occurrence of a mucus-filled lesion at the site of the piercing.
- Sports injuries that involve a head-on collision or a blow to your face can also render your salivary glands severely damaged.
- Improper chewing can cause your lower lip to get caught between your maxillary and mandibular anterior teeth, resulting in a mechanical injury to the soft tissue and the consequent development of a mucocele.
- If you rupture a salivary gland by accident, it is very likely that a mucocele will appear at the affected site.
How Can You Tell if Your Oral Cyst Is a Mucocele?
The defining features of a typical mucocele are as follows:
- Mucoceles are benign bumps in the mouth that are typically small and painless but can nevertheless be quite a bother as you are constantly conscious of the lesion.
- Larger the bump, the harder it will be to ignore. The discomfort associated with a large cyst can adversely affect your ability to chew, speak, and swallow.
- These fluid-filled sacs are characteristically smooth, soft, and shiny in appearance, with the overlying epithelium totally intact.
- When you press on the fluid-containing mass, it feels fluctuant or mobile rather than firm and it does not blanch under pressure.
- In an overwhelming majority of cases (75%–80%), the enlargement tends to appear on the lower lip, followed by other common sites including the floor of the mouth, the underside of the tongue, the inner cheeks, and the back of the lips where they meet the teeth.
- They are shaped like a dome with a translucent surface that is usually tinged with a bluish or pinkish hue for shallow cysts and straw-colored like mucus for deeper ones.
- When there is bleeding inside the lesion, it will take on a bright-red color.
- Most cases of oral mucoceles tend to resolve on their own, however, recurrence is common. The recovery period usually depends upon how shallow or deep the lesion is. A superficial and shallow cyst is more likely to burst and drain out the thick, pale-yellow fluid contained within it for the healing process to begin. However, even after the wound recovers completely, you cannot rule out the possibility of a recurrence. If the damage is deeply rooted, the cyst will naturally take longer to heal.
- Mucoceles can be of varying sizes but usually figure between 2 and 10 mm in diameter. In fact, approximately 75% of all oral cysts are reported to be less than 1 cm wide.
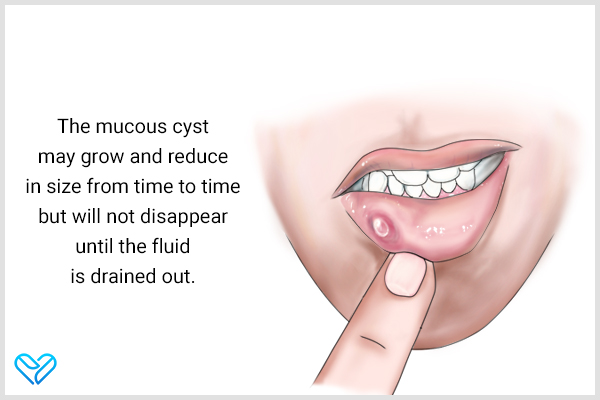
- If left untreated, the mucous cyst may grow and reduce in size from time to time but will not disappear until the fluid is drained out.
Non-Invasive First-Line Treatment
Most cases of mucoceles may be addressed with non-invasive and easy-to-follow home treatments. In fact, early interventions right at the onset of the condition can result in quick recovery.
Saline rinse
One regimen that may yield favorable results for healing small-sized oral cysts is rinsing your mouth with a saline solution.
When done regularly, this simple technique may help draw the fluid accumulated within the cyst to the surface of the skin and speed up the draining process.
Moreover, this self-care measure can help shrink the size of the cyst, reduce the risk of infection, and unclog the plugged salivary gland responsible for the formation of the cyst in the first place.
Medical Treatment for Mucoceles
Medical treatment is usually required if the cyst keeps coming back or is abnormally large. A number of surgical procedures can help remove the cyst permanently.
Surgical removal is the only way to minimize the risk of recurrence of mucous cysts.
Your doctor will take into account all the relevant factors before recommending the most appropriate treatment strategy for your particular case.
The standard choice of treatment for mucoceles includes:
- The surgical removal of the cyst along with the minor salivary gland with the use of a scalpel blade is perhaps the most commonly used method for the treatment of mucoceles. The incision is then tied together with intermittent sutures. (4)
- Another less invasive way to excise the mucocele and the adjoining salivary gland is with the use of laser therapy.
- Cryotherapy may be recommended in some cases, which essentially involves the freezing of the affected oral tissue to get rid of the cyst. (5)
- The doctor may administer an intralesional corticosteroid injection into the lesion to bring down the inflammation and accelerate the healing. (6)
- Marsupialization is another technique that is used in the medical treatment of mucoceles, especially the ones caused by a blockage of the salivary gland. (7) This procedure aids the formation of new glandular ducts, thereby allowing the accumulated saliva secretions to flow out of the glands and reopening the salivary gland.
Diagnosis of Mucocele
Identifying a mucocele is an easy task for a trained eye and usually, all it requires is a brief physical examination by your doctor.
To get a more in-depth understanding of what may have caused the cyst, your doctor will most probably take into account your medical history and inquire about any problematic oral habits that you may have.
In order to confirm the diagnosis and eliminate the possibility of a serious health risk such as oral cancer, your doctor may conduct a biopsy of the lesion. This involves scraping off a small skin sample from the affected site, which is then closely analyzed under a microscope to determine whether cancerous cells are present. (8)
This type of extended testing is usually warranted if:
- You have not encountered any kind of injury that can explain the formation of an oral cyst.
- The cyst is more than 2 cm wide.
- The fibrous wall of the lesion is unusually thick.
- The cyst is present for more than 2 weeks.
- The cyst resembles a cancerous tumor (adenoma) or a fatty lump, medically called a lipoma.
A mucocele can often be confused with canker sores, but keep in mind that mucoceles appear as raised blisters, whereas the latter appear as sores or ulcers.
Self-Care Tips for Relief
- Assess the condition of your cyst from time to time. Make sure that it has not become infected. If you notice pus formation and increased inflammation at the affected site, the chances are that your condition has progressed to infection and needs special care.
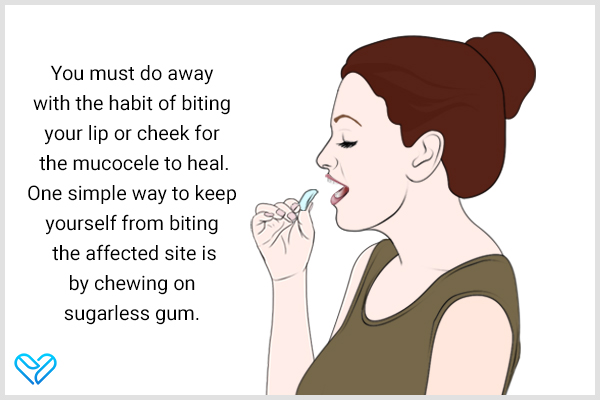
- You must do away with the habit of biting your lip or cheek for the mucocele to heal. One simple way to keep yourself from biting the affected site is by chewing on sugarless gum. This keeps your mouth occupied and helps you overcome the urge to meddle with the cyst. However, depending on the size and location of the mucocele the constant chewing can cause more trauma or friction.
When to See a Doctor
Under no circumstance should you try to excise the oral cyst on your own. Picking at the lesion can cause it to rupture and spill the accumulated fluid to other areas of the oral cavity.
The forced popping of the cyst not only increases the risk of infection but can also cause permanent scarring of the affected tissue.
A visit to the dentist is warranted if:
- Your cyst fails to improve despite proper care.
- The size of the lesion increases progressively.
- The cyst becomes so large or discomforting that it interferes with your chewing, swallowing, and speech.
Expert Answers (Q&A)
Answered by Dr. Wessam Atteya, BDS (Dentist)
A mucocele (mucous cyst) is a clear or bluish bump that forms on the lips, floor/roof of the mouth, or tongue. Mucoceles may cause difficulty while speaking, chewing, swallowing, and in some cases, breathing. They usually heal within 3–6 weeks.
Yes, they can resolve on their own. However they may persist for many years and cause discomfort. Hence surgical removal is required.
No. Mucoceles are classified as benign conditions.
Yes, especially the chronic and recurrent forms.
No, this can lead to recurrence.
Yes, it can help sometimes.
Yes, when it grows and involves the skin, it can cause some scarring (minor) after surgical removal.
The best treatment for mucoceles is excision. Simply making an incision will also drain out the contents, but it again tends to rapidly fill up after healing. They may recur after excision also, but there are fewer chances of this happening when the associated salivary glands, too, are removed.
Your doctor should then send the excised tissue for microscopic examination to check for the possibility of a salivary gland tumor.
You may also try out some home remedies for relief:
– Rinse the mouth with salt water for a few minutes, 4–6 times a day.
– Apply honey on the affected area as a cream.
Final Word
Most cases of mucoceles resolve on their own without any medical or surgical intervention but keep recurring. This is particularly true for infants and young children, with almost 44% of pediatric cases of mucoceles reported to heal on their own within 3 months on average.
That said, it is essential that you consult your registered pediatrician the minute you notice any kind of worsening in your child’s condition, whether in terms of discomfort or cyst size.
Occasionally, the cyst may rupture due to an unintentional force or trauma and release the fluid, thereby triggering the healing process.
In rare cases, the lesion may extend to the neck muscle and severely impede your breathing function. It goes without saying that cases such as these qualify as a medical emergency.
In most instances, you can expect the mucocele to reappear even after subsiding completely unless the damaged duct and mucocele are surgically excised.
- Was this article helpful?
- YES, THANKS!NOT REALLY



