In this article:
There is a lot of ambiguity among people regarding the various heart conditions, and one of the most common mistakes that people often make when they refer to acute-heart-related episodes is that they use the terms “heart attack,” “cardiac arrest” and “stroke” interchangeably.

Even though all three can be associated with the heart, their reasons for occurrence are different. They have different symptoms, and they affect the body differently as well.
Armed with proper knowledge about these three conditions and a proper understanding of their difference will help address these issues in a better way, and also alert timely to seek treatment before it gets too late.
If you or someone around you experiences any of these symptoms, then you need to seek immediate medical attention.
Understanding What They Are
Heart attack:
A heart attack is a circulation disorder. A heart attack occurs when there are interruptions in the delicately synchronized system that supplies blood to the heart and pumps blood from the heart to other vital organs.
Sometimes, the flow of oxygen-rich blood to a portion of the heart muscle is blocked or slowed. If the blood flow is not restored quickly, the muscle, which is supplied by the blocked or narrowed artery, begins to die due to a lack of oxygen. This heart-muscle-death is what is traditionally known as a “heart attack,” and medically referred to as a myocardial infarction (MI).
In a heart attack, however, the heart continues to beat.
Cardiac arrest:
A cardiac arrest, on the other hand, is when the heart stops pumping blood; cardiac arrest can result from a “heart attack,” but, fortunately, not very frequently; however, a cardiac arrest can be caused by other ailments.
Although a cardiac arrest can be caused by “mechanical” abnormalities like blood clots in the lungs and bleeding around the heart, a cardiac arrest is, more commonly, an “electrical” disorder and is the leading cause of death in adults. (1)
The heart muscle pumps in response to electrical signals that travel within the heart; this is why we can pick up “heart waves” on an electrocardiogram (ECG or EKG).
When the electrical activity of your heart experiences chaos, it causes the heart to start beating irregularly, at least initially, and then abruptly stop pumping blood through the body. This chaotic electrical activity is frequently referred to as an arrhythmia.
The patient may feel a palpitation or fluttering feeling in his/her chest moments before his/her heart stops beating completely. This is a cardiac arrest. Fortunately, not all arrhythmias lead to cardiac arrest.
Stroke:
A stroke is also caused by interruption of blood flow, but it affects the brain tissue rather than heart muscle. It is a medical emergency that happens when the blood flow to your brain is interrupted. (2)
There are three main types of strokes:
- Ischemic stroke: When the artery transporting oxygen-rich blood to the brain experiences a blockage, it causes brain cells to die. This leads to an ischemic stroke. Such blockages of brain arteries can be caused by narrowing of the arteries, but can also be caused by “small” blood clots that can come from the heart and “plug” the brain arteries.
- Transient ischemic attack (TIA): A “mini-stroke” can occur when the artery transporting blood to the brain stops doing so for a short period; symptoms of stroke can be seen during this period of blood-flow interruption, but the symptoms will resolve without residual deficits.
- Hemorrhagic stroke: When an artery ruptures inside the brain, brain cells can be damaged by interruption of flow in the ruptured artery as well as “local” effects caused by the presence of blood around the brain.
Atherosclerosis, or narrowing of the arteries by plaque, is the primary cause of a heart attack and a brain stroke, and one of the primary causes of cardiac arrest as well. (3)
Although traditional risk factors remain common among both sexes, diabetes, smoking, and psychosocial factors tend to be more strongly linked to cardiovascular events in women than in men. (4)
Understanding the Different, and Sometimes Similar, Symptoms
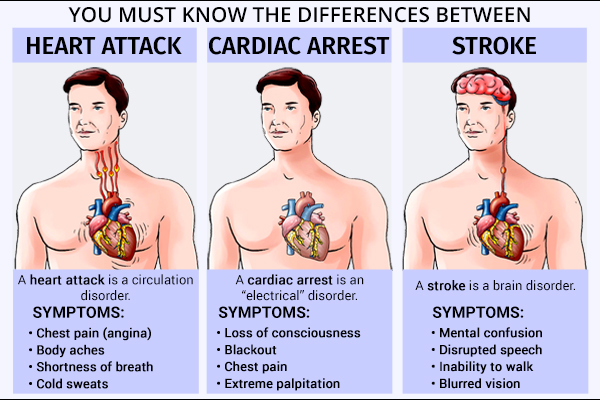
A heart attack and cardiac arrest can have common symptoms, at least initially, and it is difficult to predict whether a heart attack will lead to cardiac arrest. Fortunately, as mentioned above, a cardiac arrest does not happen frequently after heart attacks.
However, the other accompanying symptoms, as well as how long the symptoms last, differentiate these conditions from each other.
The symptoms of a stroke are mostly neurological.
Symptoms of a heart attack:
The following symptoms of a heart attack (5) can appear early on and persist for days. (6)
- Chest pain (angina): People usually characterize this as a heaviness or tightness in the middle of the chest. Some often confuse it with indigestion. It might stay for a few minutes, go away and then come back again.
- Body aches: The sensation of chest pressure or an indigestion-like feeling might be accompanied by pain in the arms (especially the left arm), neck, back, abdomen, and jaw.
- Shortness of breath and wheezing
- Cold sweats
- Lightheadedness and dizziness
- Increased anxiety
- Nausea
- Coughing
These symptoms aren’t relieved by medications, rest, or home remedies that typically resolve them when they are caused by more benign conditions.
So, if you feel like you have indigestion and you take something to treat it, the symptom will return because the problem is with your heart and not your digestive system. If the symptoms last longer than 15 minutes without relief, consult your medical provider or emergency services immediately.
In addition, these symptoms are likely to occur more when you exert yourself (running, jogging, exercising, swimming, etc.), though they can occur at rest also.
Symptoms of a cardiac arrest:
Sometimes, in the few minutes preceding a cardiac arrest, a person may experience symptoms similar to a heart attack:
- Loss of consciousness/fainting
- Blackout
- Chest pain or pressure
- Shortness of breath
- Extreme palpitation or fluttering feeling in the chest
- Generalized weakness
However, in most cases and unlike a heart attack, a person who suffers a cardiac arrest will experience:
- Symptoms of cardiac arrest that arose and dramatically worsened or accelerated within just a few minutes or even seconds.
- Becoming unresponsiveness
- Cessation of breathing
- Loss of pulse
- Sudden collapse
These appear suddenly and often result in instant death.
After a heart attack, there will be an increased risk of cardiac arrest. This is why it is important NOT to delay medical attention if a heart attack is suspected.
If you have suffered a heart attack, then you are at a greater risk of cardiac arrest.
Symptoms of a stroke:
- Sudden mental confusion: You may have trouble understanding things and following conversations. You may find it hard to remember names, places, random facts and other things you used to be able to recall.
- Disrupted speech: You may slur your speech.
- Face, arm, or leg paralysis: You may experience numbness or paralysis on one side of your face or the entire face. You may experience paralysis, numbness or weakness in your legs and arms, especially on one side. If one side of your mouth droops when you smile, or one arm keeps falling when you lift both of them up, you might be experiencing a stroke.
- Inability to walk: You may experience a loss of body coordination and dizziness while trying to walk.
- Blurred vision: Your vision may blur in one or both your eyes, or your eye may become runny. You might also start seeing double.
- Headaches: A searing pain in the head might be accompanied by dizziness and vomiting.
- Nausea or difficulty in swallowing.
- Transient ischemic attack (TIA): About 1 in 3 people who have a transient ischemic attack will eventually have a stroke, with about half occurring within a year after the transient ischemic attack. (7)
Expert Answers (Q&A)
Answered by Cardiologist Mamas Mamas

An important aspect of care is CPR by bystanders, which can lead to a double or quadruple increase in the survival rates of cardiac arrest victims. However, there are gaping disparities among the CPR rates administered by bystanders, varying between 5%–70%.
In the UK between 30% to 40% of out-of-hospital cardiac arrests receive bystander CPR. It is important that everyone knows basic CPR as it may just save your loved one’s life. I would encourage all readers of this website to learn CPR.
I often see patients at my clinic or during my practice that have had a heart attack at some point in the past without experiencing any noticeable symptoms.
Patients may have experienced symptoms that they didn’t recognize as a heart attack at the time such as heartburn, breathlessness, or a general feeling of malaise. Moreover, patients are sometimes unable to recollect the specific symptoms once they have lived through a “silent” heart attack.
High blood pressure is one of the most important risk factors for cardiovascular disease, but people often don’t realize they suffer from it until it is too late! That is why I would encourage your readers to visit their doctors and get their blood pressure evaluated. There are several ways of reducing blood pressure, ranging from a healthy lifestyle and diet to medications.
High fiber, low saturated fat diets are essential. I would advise lean meat, fish, or chicken as good sources of dietary protein. It is important to eat salads and fruits as part of a healthy diet.
People should aim to cut back on refined sugars such as chocolate, sweets, and soft drinks. Another critical factor is how you cook food, avoiding fried foods, and opting for grilled meals instead.
Final Word
Lifestyle changes can reduce the risk of cardiovascular disease. It is important to be physically active and maintain healthy body weight, along with giving up on habits that have an ill effect on your health like smoking.
It is also necessary to monitor and control your blood pressure and cholesterol levels, which is perhaps the best way to prevent heart attacks, cardiac arrests, or strokes.
- Was this article helpful?
- YES, THANKS!NOT REALLY



