In this article:
Bedsores are skin lesions that develop as a result of unrelieved pressure forces or pressure forces mixed with shearing forces over a short period of time, enough to interfere with the blood supply in the affected area.

The sores could go from the superficial to the deeper layers of the skin, occurring most of the time over boney protuberances. Bedsores are also called pressure injuries, decubitus ulcers, or pressure sores.
People at Risk of Developing Bedsores
Patients with gait impairment secondary to any physical or memory problems are at potential risk for developing bedsores. This medical problem is most of the time missed in patients in all settings – outpatient, in-patient, and long-term care facilities. (1)
Additional risk factors may include poor general health status, poor nutrition, urinary and fecal incontinence, poor hygiene, low socioeconomic status, and advanced age.
Some of the most common pathologies associated with bedsores are cerebrovascular disease sequelae affecting mobility and mentation, moderate to severe dementia of all cases, severe rheumatoid arthritis, amputation in general, spinal cord injury, and frailty. (1)
Multifactorial interventions to reduce and prevent the development of pressure ulcers are among the top strategies currently recommended to be implemented in different settings.
Different Stages of Bedsores
The healing process varies and depends on the complexity of the sore.
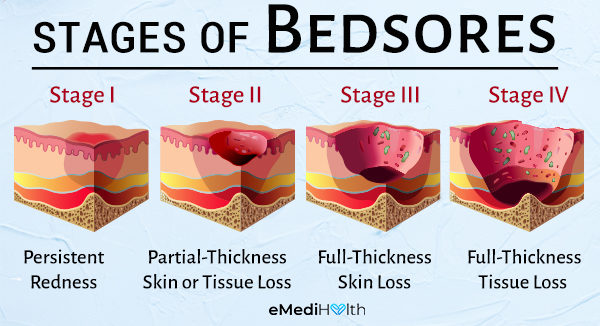
To facilitate treatment and prognosis, the lesion is classified into four stages based on the National Pressure Ulcer Advisory Panel Staging System. (2)
Stage I: Persistent redness
At this stage, the affected skin is still intact, usually over a bony area. The skin of darkly pigmented individuals may not appear pale, but its color may be different from the surrounding affected area if a lesion is present.
The area, in general, may be painful, firm, and soft with a different temperature from that of the adjacent skin.
Stage II: Partial-thickness skin or tissue loss
At this stage, the skin could be open as a superficial ulcer without associated tissue death.
The lesion could also appear as an intact or ruptured blister. It could be shiny or dry and shallow or superficial without bruising or tissue death. At this level, the affected area most likely is painful and tender.
Stage III: Full-thickness skin loss
Full-thickness skin loss is when the lesion has deepened into the subcutaneous fat without exposing bones, tendons, or muscles. Dead tissue may be associated without hiding the depth of skin loss. Other complications including skin erosion and tunneling may be present.
The depth of the sore varies by the area of the body affected. Some examples could be the ear, lower back of the head, bridge of the nose, and distal portion of the legs where there is no fatty subcutaneous tissue.
The ulcers can be superficial, contrasting with areas of significant adiposity where the sore could be extremely deep.
Stage IV: Full-thickness tissue loss
Stage IV bedsores could look like an extensive wound with possible muscle, tendon, and bone exposure with or without associated dead tissue (slough or eschar) and localized discharge.
The depth of the ulcer varies by anatomic location as explained with the stage III lesion, but the difference is stage IV ulcers can extend into muscles and supporting structures such as the tendon, joint capsule, and fascia.
At this stage, infection of the bone, known as osteomyelitis, is likely to occur. The muscle and exposed bone could be visible and/or directly palpable.
Additional stages in the United States: (2)
1. Unstageable/unclassified: Full-thickness skin or tissue loss depth unknown
There is full-thickness tissue loss and the ulcer is entirely covered by eschar or dead tissue in the wound bed.
Surgical debridement of the dead tissue or eschar is required (if clinically possible) to expose the base of the wound. The depth is difficult to determine but it is usually stage III or IV.
2. Suspected deep-tissue injury depth unknown
The affected skin may first become painful, firm, boggy, and colder or warmer than the surrounding area, and then turn purple or maroon or develop a blood-filled blister caused by damage to the underlying tissue from either pressure or shear.
This evolution may be rapid, exposing additional layers of tissue even when the best medical treatment is provided.
Such deep-tissue injury may be difficult to detect in patients with dark skin. The healing process could vary from a few days and weeks to months, depending on the severity of the lesion and the condition can sometimes lead to life-threatening complications.
How Quickly Do Pressure Wounds Develop?
Pressure wounds may develop within 4–6 hours (3) (some sources have described bedsore development even within 1 hour of exposure).
Wounds develop as a result of unrelieved pressure forces or pressure forces mixed with shearing forces directed to the affected skin in the patient, hampering the blood supply and thereafter causing skin injuries at different levels.
The Importance of Wound Dressing
Bedsores should be covered appropriately. Dressing not only contributes to the healing process by keeping the wound environment moist (yet not wet) but also provides a protective covering.
But bear in mind that the dressing should not be adhesive. There are special dressing treatments for different bedsore complexities and characteristics, which are described in the National Pressure Ulcer Advisory Panel Staging System.
The Efficacy of Petroleum Jelly for Healing Bedsores
A wide variety of topical products are available for bedsores. However, there is a paucity of data regarding which one is more efficacious for any particular lesion. Overall, only a low risk of causing more damage to the site has been described in the literature. (4)
Petroleum jelly Vaseline has been utilized to protect the skin from becoming dry and also shields the sore from animals and other surrounding contaminants. Consulting with a specialist should always be considered.
Topical Honey to Heal Bedsores
Honey does help heal bedsores as it works as a natural antiseptic and has analgesic properties as well. (5)(6)
It is important to keep in mind that any treatment selected for particular bedsore should be chosen after evaluating the affected area for moisture, exudates, or bacterial overgrowth. Consulting with a specialist should always be considered.
Best Way to Treat Bedsores in Bedridden Patients

The best way to treat bedsores in bedridden patients is to implement preventive measures and surveillance accordingly.
Moderate-quality evidence from systematic reviews sustains a multifactorial intervention to prevent bedsores development. (7) This includes the following:
- A thorough clinical evaluation should be done. A frequent assessment coming from the primary care physician leading a multidisciplinary team with ongoing education and standardization, if possible. (8)
- Good hygiene should be maintained.
- The usage of specialized support surfaces, such as pillows between parts of the body that press against each other, could be beneficial.
- Repositioning the patient frequently and avoiding friction are essential as well.
- There should be a management of nutrition in general.
Bedsores and the Risk of Sepsis
Sepsis is a potentially life-threatening medical condition triggered by the immune system’s response to a particular infection in the body. Sepsis can develop after complicated bedsore, and the decision to treat for infection should be a clinical one.
Some red flags that may alert of developing sepsis from bedsores may include reddish discoloration of the affected area with or without associated induration (hardening of soft tissue), warmth, purulent drainage, or worsening chronic drainage.
Additional signs may consist of no evidence of healing 2 weeks after appropriate treatment is given, foul odor, and the development of new necrotic tissue.
Are Bedsores Fatal?
If not treated on time, bedsores could become a severe medical condition, jeopardizing the life of the patient affected by it.
Key Points to Remember Regarding Bedsores
Some crucial points on taking care of bedsores are:
- Comprehensive geriatric assessment, including nutritional assessment.
- Optimizing nutrition in general.
- Removing all pressure over the lesion; applying basic techniques such as “floating heels.”
- Bedsore protection from potential contaminants.
- Frequent repositioning, recommended every 2 hours. However, this has not been studied in randomized controlled trials, and more research is needed. (9)
- Physical and occupational therapy evaluation; keeping the patient active if eligible for rehabilitation.
- If the wound becomes too severe for any other treatment, the doctor may recommend surgery to remove the dead tissue from the site.
- Was this article helpful?
- YES, THANKS!NOT REALLY


