In this article:
A typical foot should have an arch so that the middle of the foot does not touch the ground when standing. Flatfoot occurs when the arch of your foot has collapsed or fallen. It can develop in childhood or develop later in life as an adult.
Flatfoot has several causes, ranging from heredity to trauma to diabetes. The condition can occur in one foot or both feet. Flatfoot can progressively worsen to a point where tendons or ligaments stretch, tear, or rupture.
Prevention and management can reduce the probability of additional foot problems such as arthritis, bunions, hammertoes, and thickened skin lesions.
In many cases, flatfoot can be treated through a nonsurgical approach. Surgical management is considered when conservative treatment has not provided any benefit.
Complications Associated With a Flatfoot
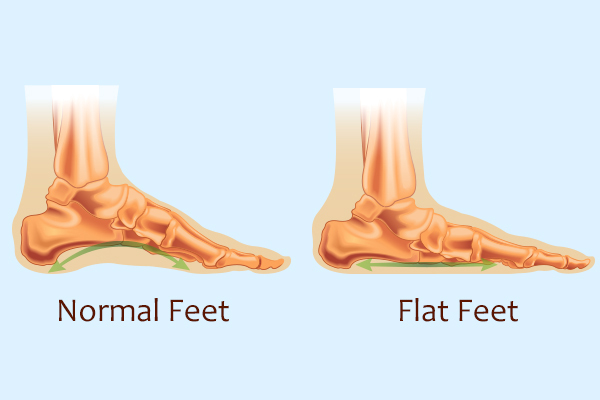
Flatfoot can cause injuries to your feet and legs due to the pressure on your ankles and knees. Some common problems associated with a flat foot are:
1. Ambulatory distortion
Flatfoot can also cause distortion to the movement of your feet and ankles. The foot acts as the foundation of your body. When the foundation changes, anything above the foundation can be altered.
2. Knee pain
If your arch flattens, the movement in your ankles changes, which in turn can change the movement of your knees, causing pain in these joints.
3. Plantar fasciitis
The plantar fascia is a band of tissue that runs on the bottom of your foot from your heel to your toes. Inflammation of this band of tissue is known as plantar fasciitis. Those with plantar fasciitis often complain of heel pain. When you have flatfoot, the plantar fascia can stretch and cause pain to your heel.
4. Achilles tendonitis
When you have a flattened foot, there is more motion in the area of the middle of your foot, also known as your midfoot. Your Achilles tendon will compensate for this extra motion by working harder and sometimes becomes excessively tightened, a condition known as Achilles tendonitis.
5. Shin splints
When your arch falls, stress to your legs increases, affecting your shins. Shin splints feel like a painful ache in the front of the lower leg. They often occur in athletes who have flatfoot, especially runners.
Nonsurgical Treatments for a Flatfoot
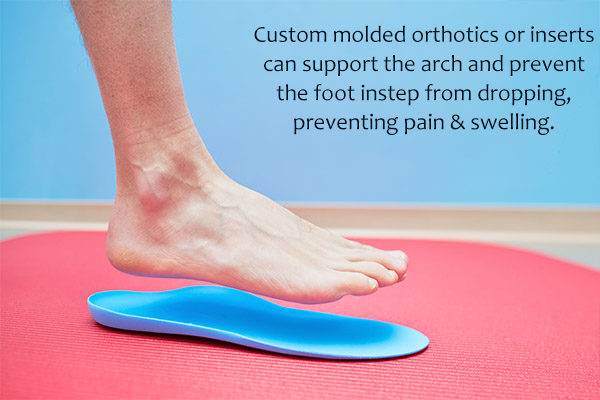
Most children with flatfoot inherited their foot type from a family member. Their feet are flexible and can be treated with inserts for their shoes called custom-molded orthotics, along with other nonsurgical interventions. These treatments can be used for adults too.
A variety of nonsurgical conservative treatments are available to relieve and prevent flatfoot pain:
- Custom-molded orthotics or inserts can support the arch and prevent the foot instep from dropping, preventing pain and swelling.
- Bracing can control and stabilize the ankle joint if flatfoot has severely progressed to affecting this joint.
- Stretching and strengthening exercises can help the foot maintain balance, stabilize joints and tissues, and prevent pain.
- Physical therapy can offer modalities to assist in pain relief, such as ultrasound therapy and cryotherapy (ice therapy).
- Supportive orthopedic shoes can support your feet and stabilize the foundation of your body.
- Anti-inflammatory medications and corticosteroid injections can reduce pain and swelling.
There may come the point when these conservative treatments are exhausted and no longer provide relief. At that time, surgical management may be an option.
Flatfoot Surgery
Flatfoot surgery is a complex procedure and refers to the reconstruction of the foot to create a supportive arch. Usually, one foot is operated on at a time. The surgery involves a combination of surgical procedures to restore the ligaments, tendons, and deformed bones of the foot.
Restoration can reduce the pain and assist the patient in returning to an active quality of life. People of all ages are eligible for this surgery.
When Is Flatfoot Surgery Needed?
Sometimes, nonsurgical options do not relieve painful adult and pediatric flatfoot. If pain and swelling interfere with the quality of your daily life, surgery may be indicated.
Surgery also may be an option if the pain is persistent or inhibits your ability to walk. If a child seems to be walking abnormally and conservative options do not help, surgery may be the next option.
Consult a doctor regularly about your child’s foot development to ensure that their foot is developing on the right track. Surgery is typically offered as a “last resort.” If conservative management fails, strongly consider surgical correction to avoid worsening of the deformity. (1)
Checkup Before Surgery
Before surgery is performed, a number of steps must be taken.
The doctor will get a full history. History should include the presence of pain and its location, intensity, timing, functional problems, and alleviating or aggravating factors. (2)
The doctor will ask you a variety of questions:
- What recreational activities do you participate in?
- What is your profession?
- Have you had previous trauma or foot surgery?
- What kind of shoes do you wear?
- Are you diabetic?
- Does your child have any neurological deficits?
- Were there any complications during childbirth?
The doctor will examine your walk to evaluate gait, joint movement, and bone structure. The doctor will examine your foot and your shoes to check for excessive wear.
Imaging modalities may be performed, such as X-rays, MRI imaging, or CT scans. These are necessary to evaluate the bone structure, ligaments, and tendons of the foot. They can help the surgeon determine the appropriate surgical procedures to perform.
Surgical Reconstruction Procedures for a Flatfoot

There is a wide variety of approaches to the surgical treatment of flatfoot. (3) Your flatfoot reconstruction surgery will be tailored to the type of flatfoot you have.
- A structure principally involved in the development of flatfoot is the posterior tibial tendon. (4) If this tendon is damaged due to your flatfoot, it can be reconstructed by replacing it with another tendon in your foot.
- The heel bone can also be augmented to help create an arch in a procedure called a calcaneal osteotomy. (5) A cut in the heel bone is performed so that it can be moved to a proper position and held together with a metal screw or staple. The surgeon may also place a metal plate at the top of the foot to create a larger arch.
- Sometimes, bone resection is performed by removing excessive bone in your foot that is causing your flatfoot. This is called tarsal coalition resection surgery. (6) Bone and cartilage are removed and replaced with muscle or fatty tissue.
- For severe flatfoot and significant deformity, fusion of joints (4) may be necessary.
Recovery usually takes 6–12 weeks. You will not be able to bear weight or walk on the foot during this time.
Some Important Tips to Aid Recovery After Surgery
- Elevate your foot above your heart as much as possible to control swelling. Do not hang your leg down.
- Keep your cast or boot clean, dry, and intact to prevent infection.
- Follow your surgeon’s instructions.
- Do not place pressure or walk on your operated foot until advised by your surgeon.
- Avoid smoking to prevent healing complications.
- Apply ice behind your knee to help reduce swelling.
- Attend follow-up appointments when scheduled.
- Take pain medications as recommended to control pain.
- Take antibiotics, if prescribed by your surgeon, to prevent infection.
- Recruit a driver if surgery was performed on your right foot.
- Physical therapy may be useful for proper gait training and to be educated on how to use crutches properly.
- Rest as much as possible.
- Invest in a reusable cast protector for the shower that you can purchase at your local pharmacy. It will prevent your bandages and/or cast from getting wet.
- Prepare your home to be comfortable after surgery and have things placed conveniently for your reach.
- If your home is two stories, prepare the first level for you to spend most of your time.
Risks and Complications Associated With Flatfoot Surgery
Complications after flatfoot reconstruction can occur. It is important that your surgeon educate you on all of the possibilities that may happen after surgery and how they can be addressed.
Complications include but are not limited to:
- Bone infection
- Skin infection
- Lingering pain
- Excessive swelling
- Blood blisters
- Excessive bleeding
- A blood clot in the leg
- Poor incision healing
- Poor bone healing
- Fusion of bones in an incorrect place
- Nerve injury
- Recurrence
- Thickened scaring
- Stiffness
- Hardware failure
Some complications can be treated with medications, bone stimulators, topical treatment, or injections.
With more serious complications, revision surgery may be the only option. Revision surgery of flatfoot must address the residual deformity if one exists, address joint pain that persists, and restore strength and balance to the foot and ankle. (7)
When to See a Doctor After Surgery
Typically, you will see your surgeon within 1 week of your surgery. The doctor will evaluate your incisions and assess your foot and leg. Your surgeon will check for infections, a clot in your leg, proper incision healing, and swelling. The bandage will be changed, and a cast, splint, or boot will be reapplied.
Final Word
Some patients may not experience pain from flatfoot. However, this condition may worsen over time and lead to pain. It is important to catch flatfoot early to take measures to prevent pain and further deformity.
You must exhaust all conservative management approaches to painful flatfoot before considering surgery. If nonsurgical treatments fail to relieve symptoms and deformity worsens, you can take a more in-depth look into surgery. Surgery should be considered as the last resort.
- Was this article helpful?
- YES, THANKS!NOT REALLY


