In this article:
Pain in the ear often arises from problems in the ear or structures close to the ear. The pain may affect either of the ears or both, and it may be constant or intermittent.

Earache is a common source of discomfort among children and may have multiple causes. It can also disturb your child’s sleep and make them fussy.
Causes of Earache
Medically known as otalgia, ear pain can have various causes. When the pain truly originates in the ear, it is called primary otalgia, which is more common among children.
Pain developing outside the ear (even though the pain may be felt in the ear) is known as secondary otalgia and is more common among adults.
Secondary otalgia may result from dental infections or temporomandibular joint syndrome. In children, earache is generally caused by ear infections or inflammation, such as otitis media and otitis externa. (1)
The common causes of earache include:
- Infection in the external ear or earlobe (cellulitis)
- Ear canal injury or abscess
- Swimmer’s ear
- Neuralgia (irritation of the nerves)
- Flu or common cold
- Measles
- Allergies
- Teething (in infants)
- Buildup of earwax
- Ear piercing
- Tight headwear
- Loud noises
- Improperly fitting earphones
- Changes in air pressure (usually during air travel)
- Presence of a foreign object in the ear
- Improper use of cotton swabs
- Soap or shampoo
Some medical conditions:
- Parotitis (inflammation or infection of the parotid salivary gland)
- Sinusitis
- Pharyngeal infections
- Lymphadenitis/lymphadenopathy (swollen glands)
- Cervical spine injury
Symptoms Associated With Earache

Earache is generally defined as a burning, sharp, or dull pain in the ear that may be constant or recurring. It may affect one or both ears.
Earache in children can be identified through the following signs:
- Crying
- Pulling of the ear (without other symptoms; ear pulling alone is not generally an indication of a severe problem in the ear)
- Irritation
- Ear drainage
- Trouble hearing
- Lack of appetite, especially in babies
- Disturbed sleep
Adults may develop the following symptoms with an earache:
- Pressure in the ear
- Feeling of blockage in the ear
- Popping or cracking sound in the ear
- Ear drainage or bleeding
- Muffled hearing
- Redness, pain, and sensitivity of the skin overlying the mastoid bone (indicative of a severe infection)
Treating Earaches
Earaches usually resolve on their own within a week. However, to ease the pain, you may take painkillers such as acetaminophen.
If the pain does not subside, the doctor may suggest the following medicines:
- Antibiotics if the infection is caused by bacteria. It is important to follow the correct dosage prescribed by the doctor.
- Pain relievers, such as acetaminophen and ibuprofen, to help ease the pain and reduce the fever. Refrain from giving aspirin to your child unless prescribed by the doctor.
- Vaccines to help prevent ear infections.
- Antihistamines to relieve symptoms of allergies.
- Decongestants if the earache is caused by a cold.
ALSO READ: Earache Treatment Tips from an ENT
Diagnosing Earache
Otalgia or ear pain is a common complaint in the primary care setting. To diagnose the condition, the following will be performed:
1. Evaluation of patient history
The doctor may ask about:
- Your age
- Location of pain
- Aggravating factors
- Radiation of pain (if the pain is felt in the ear but is arising from another part of the body close to the ear)
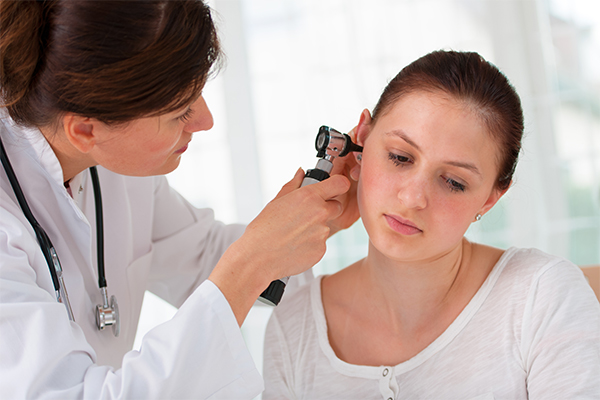
2. Physical examination
A physical exam is done to determine the source of pain and includes the inspection of the periauricular and auricle regions. Additionally, a thorough ear examination is done. Pneumatic otoscopy, tuning fork tests, and tympanometry are also helpful.
In primary otalgia, a detailed examination of the ear can document an abnormality in the ear. In the case of secondary otalgia, the ear itself may appear to be completely normal upon examination, so a more extensive and detailed examination is necessary to identify the source of the “referred” otalgia. (2)
3. Diagnostic tests
If the results of the physical exam indicate the presence of a severe cause or if the problem does not subside on symptomatic treatment, the patient may require further tests, such as:
- Audiometric testing
- CT scan
- Magnetic resonance imaging
- Fiber-optic naso-pharyngoscopy
- Erythrocyte sedimentation rate and other blood tests
- Ear or blood cultures
Risk Factors for Earache
The following factors increase the likelihood of developing an earache and must be considered for proper diagnosis and treatment:
- Smoking
- Alcohol consumption
- Age above 50 years
- Diabetes
- Overuse of cotton swabs
- Swimming and other water activities
- Snoring, sleep apnea
Complications Associated With Earaches
It is important to get timely treatment for earaches as persistent inflammation in the ear can cause damage to the structures of the ear often, which can lead to chronic or permanent hearing loss. Additionally, the infection may fester and spread to the surrounding structures.
When to See a Doctor
Although most earaches are brief and resolve on their own with no treatment, it is suggested to consult your doctor if you or your child experiences persistent or chronic earache.
Additionally, visit your doctor if:
- You or your child experiences any of these symptoms associated with an earache: fever, sore throat, vomiting, swelling around the ear, and discharge from the ear.
- A foreign object or other material appears to be stuck in the ear.
- Headache, dizziness, or weakness in the face muscles develops.
- There is a sudden cessation of the ear pain, this often indicates a ruptured eardrum and is usually associated with drainage from the ear canal.
- The pain or associated symptoms increase suddenly after 2–3 days.
Final Word
Earaches are a common occurrence that often produces discomfort, irritation, and hearing loss. If the problem is persistent, it is essential to visit your doctor to get a proper diagnosis.
Treatment is important as severe or persistent earaches can cause complications when left untreated. You can also take preventive measures to help reduce the occurrence of earaches or practice some home remedies to help subside the pain.

- Was this article helpful?
- YES, THANKS!NOT REALLY


