In this article:
Do you have severe pain with your periods? Have you had chronic pelvic pain or pain with intercourse? These symptoms could mean that you have endometriosis, a condition that affects 6%–10% of all women, (1) particularly in their 30s and 40s.
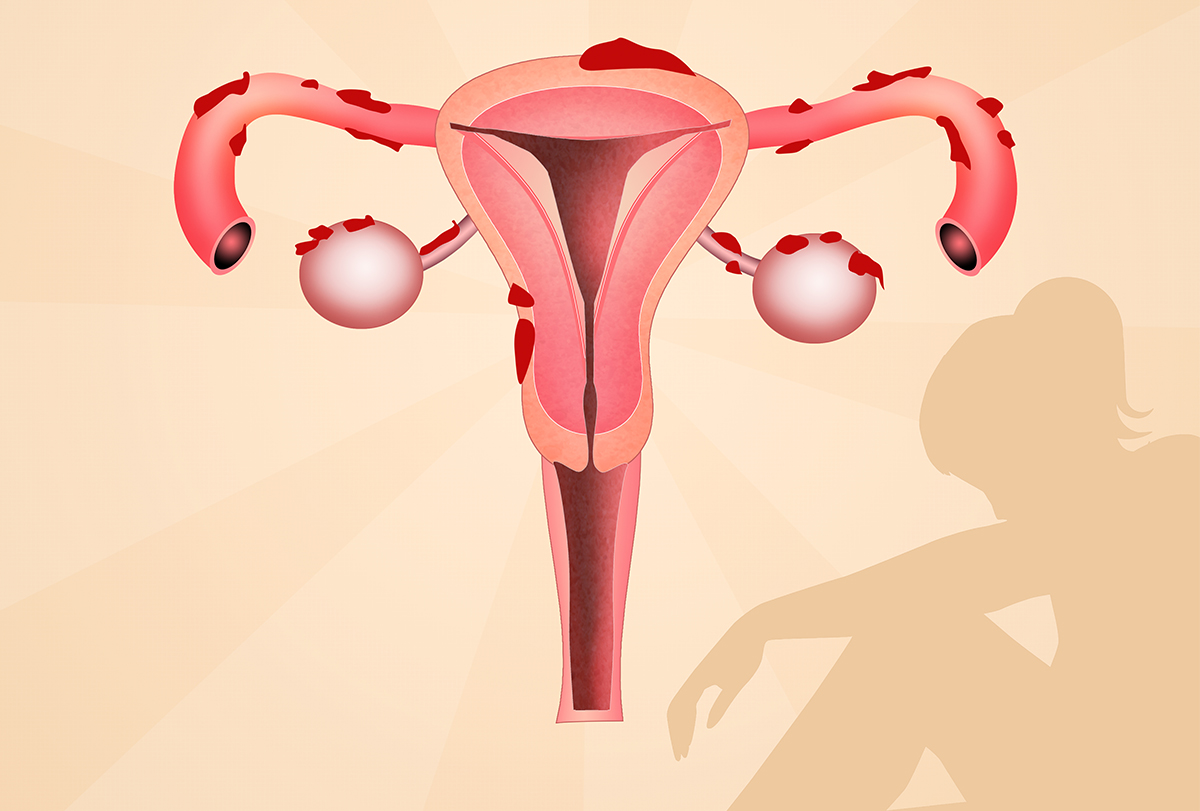
Endometriosis is a condition wherein the cells that form the internal uterine lining or endometrium grow outside of the uterus.
During a menstrual period, the lining inside the uterus is shed through the cervix and vagina. In women who have endometriosis, some part of that lining is present inside the abdomen and pelvis. With each menstrual cycle, while the uterine lining bleeds, these abnormally located cells also bleed. (2)
The presence of blood inside the abdomen and pelvis is irritating. It frequently causes severe pain. It can also cause scarring from chronic inflammation over a long period.
What Causes Endometriosis?
Implants of endometrial tissue outside of the uterus have multiple origins. (3) The most common theory is that blood from inside the uterus leaks back into the pelvis through the fallopian tubes. These endometrial cells then remain and grow in the pelvis.
With each menstrual cycle, these cells bleed along with the lining inside the uterus. While the uterine blood is shed outside the body, this blood remains in the pelvis and causes the complications seen in endometriosis.
There are two other theories of the causes of endometriosis:
- One theory explains that the endometrial cells remain in the pelvis during the development of the embryo. They then function as the lining of the uterus in response to hormones.
- The other is that the cells are distributed through the body by blood vessels and the lymphatic system. Studies have linked this spread of endometriosis to the presence of stem cells throughout the body. (4) Endometrial cells have been found throughout the body, including the lungs and, extremely rarely, the brain. (5)
ALSO READ: Understand Endometriosis Better with the Help of a Specialist
Symptoms of Endometriosis
Endometriosis is a common but discomforting condition that is characterized by several symptoms:
- The most common symptom associated with endometriosis is pelvic pain, often during menses. Menstrual pain is often so severe that it impacts daily activities.
- Bleeding may be heavy.
- Patients may also have severe pain with urination and bowel movements.
- Endometriosis that implants in the ovary usually forms a cyst, known as an endometrioma or “chocolate cyst” because it is filled with thick, dark blood. (6) Sometimes, ovaries affected by these cysts can stick to the uterus or pelvic walls. This stickiness or scarring can cause chronic pelvic pain and pain with intercourse.
Medical Treatment for Endometriosis

If you are young or have recently begun menstruating and do not have other complications, hormonal treatments may be the first line of treatment. Common agents are combination of birth control pills, progesterone-only birth control pills, (7) progesterone implants, or a progesterone-containing IUD.
- One benefit of birth control pills is lighter, less painful menses. Pills can also be prescribed continuously. Taking pills continuously means skipping the placebo or period week. This allows you to have fewer periods per year. The fewer periods you have, the less likely you will have pain and intrapelvic bleeding.
- The progesterone implant and shot can also have the same effect as birth control pills.
It is important to note the IUD will help decrease the thickness of the uterine lining but will likely not affect endometriosis in the pelvis. Other hormonal treatments for endometriosis include GnRH agonists. These medications mimic hormones that are released by the brain to control the menstrual cycle.
GnRH agonists decrease estrogen production in the ovaries by interfering with the signals from the brain to the ovaries. (8) Endometriosis is stimulated by estrogen. Without estrogen stimulation, endometriosis implants die.
GnRH agonists are effective against endometriosis, but they do have a downside. These medications reduce estrogen levels at all sites in the body and produce temporary menopause.
While using this medication, it is common to have hot flashes, skin dryness, and reversible bone loss.
Surgical treatments for endometriosis
A patient who has severe pain and evidence of an endometrioma on imaging or exam may choose to undergo a surgical procedure called laparoscopy.
During the surgery, the doctor inserts a camera into the abdomen to look at the organs directly. The doctor can then remove endometriotic implants and ovarian endometriosis or attempt to free scar tissue.
If endometriosis has been untreated for many years, the scar tissue may be exceedingly thick and difficult to remove. Repeated operations can also promote scarring in the pelvis and should not be performed unnecessarily.
If the patient does not respond to any other treatment or surgery, the doctor may recommend a hysterectomy, or the surgical removal of the entire uterus, as a last resort.
Diagnosing Endometriosis
If you have any of the symptoms of endometriosis, it is important to see your doctor for an evaluation. To date, no blood test will diagnose endometriosis.
Instead, your doctor will take a history, ask questions about your symptoms, and perform a thorough physical exam. He/she may order an ultrasound or MRI to evaluate your pelvis for signs of abnormality.
Once your doctor suspects endometriosis, you should be offered one of the many treatment options available. The treatment will depend upon the findings, age, and goals.
Risk Factors for Endometriosis
Endometriosis can develop in these groups:
- All women of reproductive age can be affected by endometriosis.
- Women who have a mother or sister with endometriosis have a 7–10 times higher likelihood of having the disease. (1)
- Endometriosis seems to occur equally across races. Recent studies have suggested that endometriosis has been overdiagnosed in Asian women and underdiagnosed in African American and Hispanic women. The issue may be related to systematic underdiagnosis. Access to care is thought to be another factor. By the time they seek infertility treatment, both Black and White women have been shown to have an equal incidence of the disease. (9)
Can Endometriosis Cause Difficulty With Bowel Movements?

Yes, up to one-third of women with endometriosis can have severe pain with bowel movements during menses. The pain can be “sharp and stabbing.” Patients can also have intermittent diarrhea and constipation during their menstrual cycles.
Pain with bowel movements implies that endometriosis implants are present in the wall of the colon or rectum. (10) If cells are present in the bladder, patients may also have pain with urination.
Can Unexplained Fatigue Be a Sign of Endometriosis?
While pelvic pain is the most well-known symptom of endometriosis, there is growing evidence that endometriosis causes many more complications.
In women with symptomatic endometriosis, up to 50% have been found to have fatigue and insomnia. This increase in fatigue was noted even when researchers controlled for “pain, insomnia, occupational stress, depression, BMI, and motherhood.”
The researchers concluded that this aspect of endometriosis was independent of disease symptoms. “Patients with varying levels of symptoms still showed increased symptoms of fatigue over patients without endometriosis.” (11)
Can Pelvic Pain Alone Confirm the Presence of Endometriosis?
Crampy pain with menses is common and is not, by itself, an indicator of endometriosis. Chronic pain syndromes, chronic fatigue, depression, and autoimmune conditions seem to overlap with endometriosis. These conditions may be diagnosed while endometriosis remains undiagnosed.
Interestingly, many women who have endometriosis are asymptomatic and are only diagnosed when they seek help for infertility. (12)
The Harmful Effects of Endometriosis on Pregnancy and Fertility

One of the main complications of endometriosis is infertility. Up to 50% of patients being treated for infertility are found to have endometriosis. (1)
The chronic inflammation associated with endometriosis often creates a hostile environment in the pelvis. In addition, chronic inflammation and bleeding often lead to scarring, which can damage the fallopian tubes.
Implants of endometriosis in the ovaries can affect ovarian function and further contribute to infertility. Once pregnant, patients generally have some relief from their symptoms. However, if scarring is present in the pelvis, it may cause pain during pregnancy as the uterus grows and stretches.
Why Does Endometriosis Trigger Pain During and After Intercourse?
One of the most common symptoms of endometriosis is pain with intercourse.
A frequent cause of pain is the scarring that occurs due to chronic inflammation and bleeding in the pelvis. (13) This is how it happens:
- The presence of blood in the pelvis provokes inflammation.
- The inflammatory cells can cause the surface of the uterus, tubes, and ovaries to become sticky.
- This stickiness, over time, causes thick scarring.
- Once scarred, the pelvis loses elasticity.
- The uterus, ovaries, and tubes can become locked in place by scars.
- Intercourse can cause these scars to pull and stretch.
- The loss of mobility and elasticity in the pelvis causes pain, which can be severe.
Why Does Endometriosis Cause Pain in the Legs?
The nerves that carry messages throughout the body branch out from the spinal cord. The nerve supply to the lower body passes through the pelvis and down to the legs.
When endometriosis grows in the pelvis, it can implant over these nerves, including the sciatic nerve. Bleeding from these implants can aggravate the nerves, causing inflammation and scarring. (14)
Once these nerves are irritated, pain fibers are activated, causing pain in the pelvis, back, and down the legs.
Medical Conditions That Mimic Endometriosis Symptoms
In the past, endometriosis was thought to be a reproductive issue. Now, endometriosis is revealed to be multifaceted.
- Patients with endometriosis can have symptoms that can overlap with irritable bowel syndrome or other gastrointestinal disorders.
- Untreated pelvic pain may lead to chronic pain syndromes and pain that is triggered by factors unrelated to endometriosis. (15)
- The fatigue that is common in patients with endometriosis may be misdiagnosed as chronic fatigue and/or depression.
- Chronic lower urinary tract problems can also be caused by endometriosis.
Expert Advice for Endometriosis Patients

Here’s what you need to know about managing endometriosis:
- See your gynecologist for evaluation, rather than relying on the suspected diagnosis of well-meaning friends and family.
- Surgery is not always necessary for treatment. Good control can be obtained with hormonal agents.
- Chronic, untreated endometriosis can lead to pelvic adhesions, pain, scarring, and infertility. Consider continuing treatment if you have been diagnosed with endometriosis.
- Just because you have endometriosis does not mean you will have infertility.
- There are other possible diagnoses for pain with intercourse; some sexually transmitted diseases can cause pain and infertility too. See your doctor for an evaluation.
- New medications are available for pain management in endometriosis. Your doctor may recommend these for you.
The good news is that treatments are available for endometriosis. If you are diagnosed, you should be able to suppress pelvic pain and chronic inflammation to a great degree. If you can minimize scarring, you are less likely to have pain with intercourse and long-term problems.
Reproductive endocrinologists are well versed in the treatment of endometriosis and related infertility, so you have reproductive options as well.
Final Word
Endometriosis is a tricky disease and has varied presentations. Some patients have terrible pain and have little to no visible disease at the time of surgery.
Other patients have findings on ultrasound and extreme pelvic abnormalities but complain very little of the pain. It is remarkable how patient experiences can vary with this disease.
Endometriosis does not have to limit your life choices. Take advantage of the treatments available to maximize your sexual and reproductive health.
- Was this article helpful?
- YES, THANKS!NOT REALLY


