In this article:
Cellulitis is an acute bacterial infection that affects the deep layers of skin, namely, the lower dermis and subcutaneous tissue.

It is often acquired through a breach in the skin barrier, such as injuries, diabetes, eczema, surgical procedures, IV drug use, and lymphedema. The infection can induce redness, swelling, and pain at the affected site and can even trigger potentially dangerous complications if not treated properly.
Things to Do at Home
Antibiotics are the crux of cellulitis treatment, but a few self-care measures can also help reduce the intensity of symptoms, minimize the spread of infection, and reduce recovery time when coupled with standard medications.
1. Rest
Give your body plenty of rest to help it recuperate fast. The energy you save while resting will be utilized for fighting the infection.
2. Elevating and applying a warm or cold compress
Keeping the affected area in a raised position may help curb swelling. You can register some relief by applying a warm or cold compress on the infection site. (1)
3. Wound care
You have to monitor the condition of your wound every day to see if it is healing properly. The wound should be cleaned regularly and covered with a fresh dressing.
Home Remedies for Cellulitis
You can use these easily-available ingredients to expedite recovery from cellulitis, as they have delivered good results for several users:
1. Drink turmeric tonic
Turmeric is a much-touted healing agent which is credited with significant antimicrobial and anti-inflammatory properties that mainly stem from its chief compound curcumin. (2)(3)
There is considerable anecdotal evidence to support the infection-fighting potential of turmeric, but its efficacy for treating cellulitis still needs to be verified through proper scientific research.
How to use:
- Mix a teaspoon of turmeric into a mug full of water.
- Heat the solution until it comes to a boil.
- Add a bit of honey to sweeten its taste
- Drink this tonic twice daily until your condition improves.
2. Use garlic as a healing aid
Garlic is a common kitchen ingredient with exceptional medicinal properties that have been widely utilized by general users for treating infections like cellulitis.
Although a lot of people reported positive results after using this remedy, there is virtually no direct research to establish its mechanism or effectiveness. Nonetheless, garlic is one of the most commonly cited remedies for cellulitis, which may have something to do with its powerful anti-bacterial activity. (4)
How to use:
Garlic can be taken orally or applied topically at the site of infection to promote quicker recovery from cellulitis.
- People who can tolerate the strong taste and smell of raw garlic are advised to consume several cloves daily.
- Alternatively, you can prepare a healing oil by frying 3 or 4 crushed cloves, adding some virgin coconut oil to it, and then straining the liquid into a container once the mixture cools. Apply the oil on the infected area, and let it sit for several hours so that it gets absorbed into the skin before washing it off. Repeat the process daily.
Caution: Stop the topical use of garlic if you experience even the slightest irritation after applying it.
3. Use fenugreek topically
Fenugreek seed is another popular anecdotal remedy for treating skin inflammation and infections like cellulitis, which has gained greater legitimacy after being medically approved in Germany for topical use.
Fenugreek is enriched with certain phytonutrients called flavonoids which are known for their antioxidant, antibacterial, and anti-inflammatory effects, all of which can help in healing cellulitis. (5)
How to use:
- Soak 2 tablespoons of fenugreek seeds in warm water until they turn soft.
- Now mix these seeds with a little water and grind them into a paste.
- Apply this paste on the affected areas of your skin. Repeat the process daily for as long as it takes to overcome the infection.
Caution: Discontinue this remedy immediately in case of any discomfort or adverse reaction.
4. Dab on some manuka honey
Manuka honey is one of the purest and most therapeutic forms of honey that has been popularly used for wound-healing and other medicinal purposes, not just at home but also in hospitals across various countries. Thus, the external use of Manuka honey for treating cellulitis is largely safe and definitely worth a try. (6)
How to use:
Apply the manuka honey onto the affected areas of the skin, and leave it on for several hours so that it penetrates deep into the skin. Regular use is key for this remedy to work, so apply the honey daily until your symptoms subside.
5. Apply essential oils
Essential oils have gained a lot of traction among general users for addressing a wide array of maladies, including cellulitis. These oils are derived from various therapeutic plants and exhibit their own pharmacological properties.
Some of the most commonly used essential oils for treating cellulitis and other skin infections include tea tree oil, yarrow oil, oregano oil, etc., all of which work as anti-inflammatory as well as anti-microbial agents. (7)(8)
How to use:
- Essential oil is extremely potent, and must always be diluted with water or other carrier oils before application. In this case, it’s best if you use other beneficial oils like coconut oil/olive oil for added relief.
- Mix a few drops of your preferred essential oil in a tablespoon of coconut or olive oil and apply it all over the affected area.
Caution: Apply only a tiny amount first to rule out any skin irritation or reaction.
6. Soak the infected area in an Epsom salt bath
Epsom salt is one of the most extensively used home remedies for various conditions, but it rests mainly on anecdotal support with little to no scientific backing.
This therapeutic salt breaks down into magnesium and sulfate when exposed to water, which may help bring down skin inflammation and curb bacterial growth.
How to use:
- Fill a tub or bucket with water and add some Epsom salt to it.
- Soak the affected area in this bath for 15–20 minutes.
Lifestyle Changes to Prevent Cellulitis
Adopt these lifestyle changes to reduce the risk of cellulitis.
1. Keep it clean
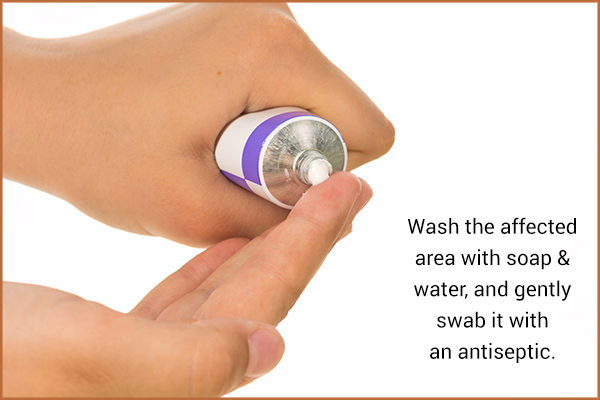
Open wounds should be cleaned every day to avoid infection. You can simply wash the affected site with soap and water and gently swab it with an antiseptic.
2. Avoid scratching
Getting stung or bitten by an insect often triggers a lot of itching, but you must resist the urge to scratch as it can erode the skin further and transfer the dirt and germs from your fingers and nails to the affected site.
If the itch becomes so overwhelming that it is hard to ignore and disrupts your sleep, ask your doctor to suggest some interventions to manage it safely.
3. Take care of your skin
Dry skin is more prone to damage, itching, and cracking, all of which pave the way for cellulitis. It is, therefore important to keep your skin well hydrated both from within and outside.
The easiest way to do so is by drinking plenty of water throughout the day and regularly moisturizing your skin with a lotion or ointment that is suitable for your specific skin type.
4. Keep your nails clean and properly filed
You could accidentally scratch yourself with a broken nail, so it is important to keep them properly trimmed and filed. When cutting your fingernails and toenails, take care not to injure the surrounding skin.
5. Avoid smoking and drinking
Unhealthy habits such as smoking and drinking alcohol can make you more prone to cellulitis and, therefore, should be avoided, especially in the wake of a skin injury.
6. Practice proper hand hygiene
Wash your hands frequently, especially after touching the infected area. Keeping your hands clean at all times, avoids contracting the infection in the first place. Hand sanitization is essential for people who already have cellulitis too, as it keeps the infection from spreading to other parts of the body.
7. Observe good personal hygiene

Personal hygiene is a must to avoid skin infections such as cellulitis. This includes regular bathing, changing your underwear every day, proper hand hygiene, changing out of damp clothes as soon as possible, and keeping your genital area clean and dry.
Make sure that your feet are moisture-free before putting on socks, wear fresh socks every day, and do not wear the same footwear for days on end.
8. Protect your skin
Covering your skin with protective gear can reduce the risk of injury and, thereby, infection. Always wear gloves when tending to your garden, handling abrasive equipment, or doing any such activity, which involves a high risk of cuts and scrapes.
Foot injuries are very common and often go unnoticed since you rarely observe your feet closely. So, always wear protective footwear whenever you venture outside, especially if you have diabetes.
9. Lose weight
People who fall on the heavy side are more likely to contract cellulitis than people with a normal body mass index.
Moreover, cellulitis treatment does not work as effectively on obese and overweight individuals as it does on healthy-weight patients. In fact, those who are overweight are often unresponsive to the preliminary treatment of cellulitis and need to be hospitalized. (9)(10)
10. Treat other medical conditions
Several medical conditions can predispose you to cellulitis, including eczema, athlete’s foot, leg ulcers, and lymphedema. If you suffer from any such problems, it is important to manage them properly to reduce the risk of cellulitis.
11. Promptly treat superficial skin infections

Untreated superficial skin infections like athlete’s foot can spread from the epidermis to the deeper layers of the skin and trigger cellulitis.
12. Drink ample amounts of water
Consume at least 3 liters of water throughout the day to keep your body sufficiently hydrated and to increase urination. A well-hydrated body is better equipped to fight infections, while frequent urination will help eliminate the infection-causing bacteria from your system. (11)
Most-Asked Questions About Cellulitis
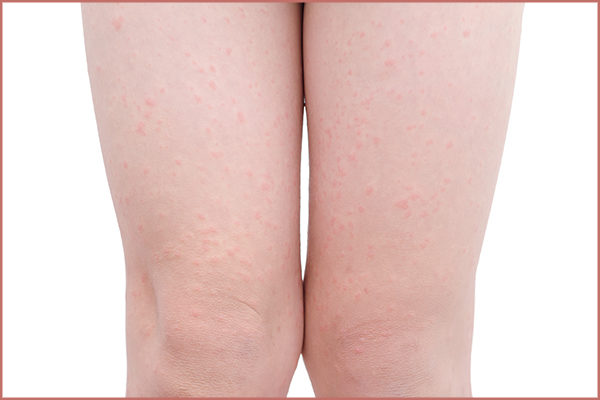
Is cellulitis contagious?
No, cellulitis does not spread from person to person through physical contact as the infection is embedded deep inside the skin. Impetigo, on the other hand, is a superficial skin infection that can be easily transmitted to others through a simple touch.
In cellulitis, the bacterial infection is limited to the deep layers of the skin that do not come in contact with other surfaces. Thus, the chance of transmission through contact is negligible.
Can you swim with cellulitis?
Wait for the injured skin to scab over before immersing it in water. Venturing into a public pool before the injured skin has scabbed over will not only delay the skin regeneration process but will also contaminate the water for others.
Scab tissue formation is your body’s way of protecting the injured skin and a sign of healing. Be extra careful to keep the infected wound away from other people if it is oozing pus.
Can you recover from cellulitis?
Yes, cellulitis is a curable condition that is best treated with doctor-prescribed antibiotics along with proper self-care and rest.
Early treatment not only promotes fast recovery but helps prevent the spread of infection. In some cases, untreated cellulitis can lead to shock or can spread to the blood and cause fatal sepsis.
Final Word
Personal hygiene, proper skin care, and staying injury-free are the three best ways to avoid cellulitis. But if it does occur, this deep-seated infection will require proper antibiotic treatment to thwart the growth of bacteria.
The prescribed medication will deliver symptomatic relief and fast healing if combined with the home therapies and self-care measures.
In some cases, untreated cellulitis can lead to shock or can spread to the blood and cause fatal sepsis. If the condition persists despite the prescribed treatment and care, consult your doctor for treatment modification or identification of some other condition that may be causing your symptoms.

- Was this article helpful?
- YES, THANKS!NOT REALLY


