In this article:
Lupus is an autoimmune disorder wherein your immune system wrongly perceives the body’s healthy tissue as a foreign threat and starts attacking it with autoantibodies, causing systemic inflammation that affects multiple organ systems.
Lupus does not have a standard set of symptoms. It can manifest differently in different patients and their treatment has to be customized accordingly.
Lupus is a lifelong condition characterized by periods of remission and flare-ups. Lupus flare-ups can vary in severity, from a mild disease that requires little treatment to severe cases that can be life-threatening.
The condition has many manifestations because different systems of the body may be involved. This illness with many faces can affect several or all organs, including the heart, lungs, kidneys, blood vessels, brain, joints, and skin.
Types of Lupus
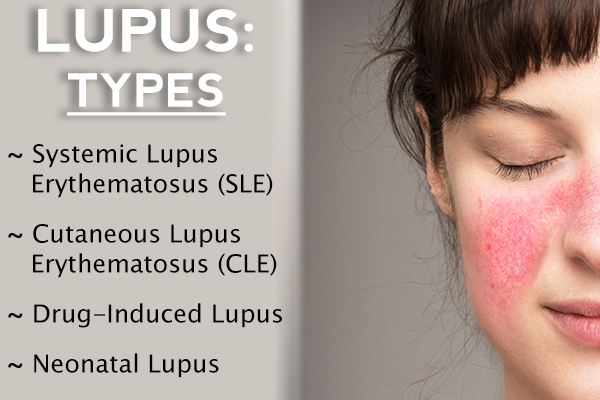
There are two main types of lupus: systemic lupus erythematosus and cutaneous lupus erythematosus. Other types are drug-induced lupus and neonatal lupus.
1. Systemic lupus erythematosus
The term lupus is broadly used to refer to systemic lupus erythematosus (SLE), which is the most familiar form of this disease. Systemic means it can affect the entire body and is more severe than the other types.
The symptoms of SLE can range from mild to severe and tend to appear in cycles of remissions and flare-ups. SLE is the most critical type of lupus and commonly affects the tendons, joints, and skin. It may also encompass the heart, brain, kidneys, and lungs.
2. Cutaneous lupus erythematosus
Cutaneous refers to something that affects the skin. The cutaneous lupus erythematosus (CLE) is essentially a skin disease that causes rashes, ulcers, hair loss, sun sensitivity, and swelling in the blood vessels.
CLE can develop in individuals whether they have SLE or not. Around 5% of people with cutaneous lupus may develop SLE later. (1)
Cutaneous lupus can be of two different types:
- Discoid lupus erythematosus (DLE): The impact of this form of lupus is limited to the skin. DLE is characterized by the appearance of a raised, thickened, and scaly rash on the face, scalp, or elsewhere, which often leaves behind a scar.
- Sub-acute cutaneous lupus erythematosus: Exposure to ultraviolet light can trigger a lupus rash, which is often found in sun-exposed regions of the body. This leads to the formation of skin lesions, which, unlike DLE, do not cause scarring.
3. Drug-induced lupus
Another important type of lupus is drug-induced lupus. It accounts for 10% of all lupus cases and the symptoms are similar to those of SLE. (2) Around 80 prescription drugs can cause an adverse reaction and trigger the onset or flare-up of lupus symptoms.
These drugs include medications used to treat hypertension, thyroid dysfunction, and seizures, as well as several antibiotics, antifungals, and oral contraceptive pills.
Procainamide, hydralazine, minocycline, and some types of sulfa medications are common culprits in drug-induced lupus. This type of lupus is relatively less aggressive with milder symptoms that tend to subside when the medicine is stopped.
4. Neonatal lupus
Rarely, the mother’s antibodies may have a negative impact on the fetus. As a result, the child may be born with a skin rash, low blood cell count, or liver problems. However, these symptoms usually resolve after 6 months, even without treatment, and have no lasting effects.
Symptoms of Lupus

The symptoms of lupus are discontinuous, vary among individuals, and may even change as the disease progresses.
The most common symptoms experienced by individuals with lupus are:
- Fatigue
- Muscle and joint pain
- Skin rashes – Butterfly-shaped rash across the cheeks and nose, known as a malar rash
- Alopecia (hair loss)
Other frequent symptoms include:
- Fever
- Generalized weakness
- Chest pain
- Oral dryness or ulcers
- Raynaud’s phenomenon
- Photosensitivity
- Malaise
- Anemia
- Anxiety
- Water retention
- Weight loss
- Clinical depression
- Stomachache
- Headaches and dizziness
- Confusion and seizures
- Pain while lying down or taking deep breaths
Lupus Flare-Ups
The period during which lupus symptoms, such as pain, fatigue, and a rash, get aggravated is known as a flare-up. It has a sudden onset and may be triggered by UV light exposure or stress. Because lupus may affect many body systems, additional symptoms depend upon the region affected.
For example, there may be nervous system involvement, which may cause burning and tingling of the peripheral nerves, loss of sensation or strength in a limb, headaches, or even confusion, seizures, and psychiatric problems.
If the circulatory system is affected, anemia or clotting problems arise, leading to easy bruising and bleeding. One of the most important and worrisome problems for individuals with lupus is the potential for kidney involvement.
“Lupus nephritis” may cause severe leg swelling and can sometimes lead to kidney failure. A need for hemodialysis or kidney transplant may arise.
Most-Asked Questions About Lupus
Do lupus symptoms worsen with age?
Not necessarily. Those who first develop SLE at an older age tend to have a milder course than younger individuals.
Why is lupus more common in women than men?
It has been postulated that the higher incidence in women than in men has to do with sex hormone differences between sexes.
Some studies have suggested that those on birth control pills may have a higher risk, and in some individuals, estrogen-containing medications seem to aggravate the disease. (3) However, other studies have not found this to be the case, so the matter is more complicated.
Other theories suggest that the female preponderance is related to genetic factors on the X chromosome. So, it is really not understood why women have so much greater risk. (4)
Final Word
Lupus is a rare and unpredictable disorder with symptoms that can vary from patient to patient and from time to time. The disease may be incurable, but it can be effectively managed through a multidimensional treatment approach that is customized to the patient’s needs.
This involves consuming a proper diet, getting adequate physical exercise, and making the necessary lifestyle changes along with taking doctor-prescribed medication. The sooner you start treatment, the better the treatment results and disease management.
For the sake of early diagnosis and treatment, you must educate yourself about the condition and its symptoms and work closely with your doctor to minimize flare-ups and the risk of complications.
Learning about the disease will help you identify the warning signs of an impending flare-up and seek immediate medical recourse to make the symptoms less severe. This proactive approach will help you lead a long, productive life, even with such a chronic illness.

- Was this article helpful?
- YES, THANKS!NOT REALLY


