In this article:
Rhinitis refers to the irritation or swelling in the mucous lining of the nose. When it occurs after exposure to allergens, it is known as allergic rhinitis or hay fever, which is a highly prevalent ailment.

This chronic illness is associated with significant respiratory distress, which can impede your productivity and overall quality of life as well as aggravate comorbid conditions such as asthma.
Home Remedies to Relieve Allergic Rhinitis
The following cost-efficient and effective home remedies can help manage the symptoms of allergic rhinitis.
1. Flush your nose with saline water
Nasal congestion associated with allergic rhinitis can be treated with a saline nasal wash, which helps facilitate the easy removal of excess mucus. (1)(2)(3)
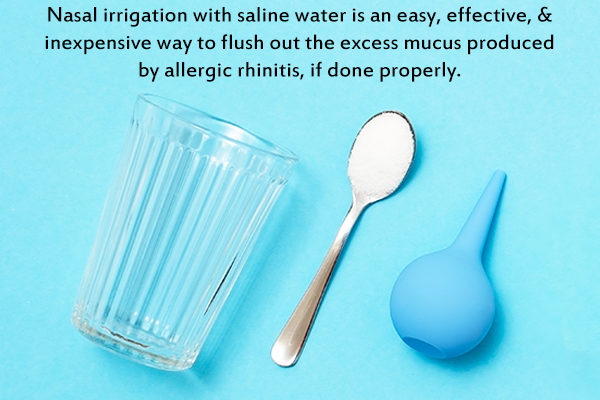
Both over-the-counter and homemade saline solutions can be used for nasal irrigation, but one study found self-made hypertonic solutions to be 0.9% more effective than commercial isotonic ones. (3) It is best if you consult your doctor to decide which one is most suitable for you.
Directions:
- Mix 1 teaspoon of salt in 2 cups of warm distilled water, or use an over-the-counter saline solution.
- Using a bulb syringe, pour small amounts of the solution into one nostril.
- Let the solution drain through the other nostril or mouth.
- Blow your nose gently to get rid of the mucus and remaining solution.
- Replicate the process in the other nostril.
- Perform this therapy twice every day until the symptoms subside.
Nasal irrigation with warm saline solution dilutes the thick mucus clogging your airways and helps flush it out along with other irritants that may be trapped inside the nose. This is a fairly safe method to clear a clogged nose, provided it’s done correctly.
2. Try steam inhalation
Steam inhalation helps dilute and loosen the excess mucus in your nasal passages, thus making it easier to expel.
Both these actions are useful for relieving the symptoms of allergic rhinitis, such as nasal congestion, sore throat, runny nose, postnasal drip, facial pain, nasal itch, eye irritation or watering, and sneezing. (4)(5)
Directions:
- Boil water and pour it into a big bowl.
- Add in a few drops of essential oils such as peppermint, eucalyptus, tea tree, or rosemary oil.
- Use a towel to cover your head and lean over the bowl.
- Inhale the steam with deep breaths for 5–10 minutes, and blow your nose thoroughly.
- Repeat the procedure multiple times a day until the symptoms subside.
Note: Steam inhalation is not safe for small children. Give them a warm bath or shower instead.
Steam inhalation involves breathing in warm, humid vapors that water down the consistency of the phlegm to make it easier to expel and may even curb the secretion of inflammatory chemicals from mast cells.
3. Drink stinging nettle tea
Stinging nettle has been widely used as an alternative treatment for seasonal allergies, including allergic rhinitis. It provides quick relief from itching, sneezing, coughing, and nasal congestion.
Multiple studies have demonstrated its role in alleviating allergic rhinitis by the action of its active compounds, including phenols that inhibit inflammatory pathways. (6)(7)
Directions:
- Mix 1 tablespoon of dried stinging nettle leaf in 1 cup of hot water.
- Cover the mixture and allow it to steep for 5 minutes.
- Strain and add honey.
- Consume this tea two to three times a day until the symptoms subside.
- Alternatively, consider stinging nettle supplements.
Note: Consult your doctor before using this remedy, as it may interact with your medications. Refrain from giving stinging nettle to pregnant women and young children.
Stinging nettle may help reduce the inflammatory symptoms of allergic rhinitis by inhibiting the release of histamine which is at the base of this adverse reaction.
4. Add probiotics to your diet

A 2011 study demonstrated the effectiveness and safety of using probiotics for the treatment and prevention of hay fever. However, its mechanism could not be determined. (8)
Another 2013 study favored the administration of a specific probiotic, namely, Lactobacillus acidophilus, for reducing the frequency and severity of allergic rhinitis symptoms. (9)
Directions:
Probiotics are available in various forms, including natural sources such as yogurt, that can help boost the immune system.
Probiotics are good sources of healthy gut bacteria that can help in strengthening your immune response to various common allergens that cause rhinitis.
5. Consume more vitamin C
The antihistamine and immune-boosting properties of vitamin C play crucial roles in managing allergy symptoms, preventing infections, and reducing the duration of illness. (10)(11)
Directions:
- Consume vitamin C-rich foods, such as oranges, lemons, broccoli, kiwi, potatoes, strawberries, grapefruit, tomatoes, sprouts, and bell peppers.
- Alternatively, take vitamin C supplements upon consulting your doctor.
While multiple studies support the use of these therapies for reducing various symptoms of allergic rhinitis, more rigorous research is needed to conclusively establish their efficacy, safety, and mechanism of action.
Vitamin C is credited with significant antioxidant and anti-inflammatory potential that can help in the management of various allergies, including allergic rhinitis.
6. Consume turmeric like a medicine
Turmeric is credited with significant antioxidant, immune-boosting, and anti-inflammatory properties that can help in the management of allergic rhinitis symptoms, such as cough, sneezing, dry mouth, and nasal congestion. (12)
This remedy has been used by many to relieve allergic rhinitis, but there isn’t enough scientific evidence to confirm its mechanism and benefits.
Directions:
- Turmeric is a versatile spice that can be used in various dishes, and can, therefore, be easily included in your regular diet. Moreover, using black pepper with turmeric can enhance the bioactivity of curcumin which is turmeric’s chief medicinal compound.
- You can also brew yourself a nice cup of turmeric tea.
- You can ask your doctor about starting you on a turmeric supplement.
7. Have some honey every day
A study conducted in 2013 demonstrated that intake of a high dose of honey was beneficial in diminishing the symptoms of allergic rhinitis, thus favoring its use as an adjunct therapy. (13) Further studies are however needed to conclusively establish the efficacy of honey in managing allergic rhinitis.
Directions:
Consume one tablespoon of honey directly or mix it in a cup of warm water to make a therapeutic tonic.
8. Drink diluted apple cider vinegar
ACV is credited with antioxidant, antimicrobial and detoxifying properties that may help eliminate the germs responsible for inducing allergic rhinitis. (14)
Moreover, this mildly acidic liquid can help breakdown the phlegm accumulated in your respiratory airways and help speed up its expulsion to restore normal breathing.
Directions:
Always dilute ACV before consumption as it can be too harsh at its original concentration. Mix 1-2 tablespoons of ACV in a glass of warm water and drink this solution once a day.
Note: ACV is mildly acidic but can cause acid reflux and tooth erosion if consumed in undiluted form or excessive amounts can erode the tooth enamel hence it is advisable to consume it in diluted form and consult your doctor before consuming.
9. Include fish in your diet
Fish has also earned a lot of praise from general users for its ability to curb inflammation and an allergic response. A study concludes that fatty acids present in fish helped decrease the contraction of airways triggered by allergic diseases such as asthma. (15)
Directions:
Fish makes for a healthy addition to your diet and can be consumed hot or cold and as a separate dish or as part of salads.
10. Get more quercetin
Quercetin is a flavonoid that gives many fruits and vegetables their color. Thus, various foods that are naturally pigmented such as apples, grapes, berries, broccoli, onions, and such are heavily endowed with quercetin. Other good sources of these flavonoids include certain herbs, tea, and wine.
Quercetin works as a powerful antioxidant that may help in managing seasonal allergies, including allergic rhinitis. Moreover, a study shows that quercetin acts as natural antihistamine hence helps in reducing the symptoms of allergic rhinitis. (16)
Directions:
- You can simply include various foods that are rich in quercetin in your daily diet to reap the therapeutic benefits of this polyphenol.
- You can even take quercetin supplements but only after consulting your doctor about proper dosage and use.
Alternative Treatment
Here is another specialized intervention that may help reduce the intensity and frequency of allergic rhinitis, if done correctly:
Acupuncture
Acupuncture is a traditional Chinese technique that involves inserting needles at specific points of the body to enhance blood circulation and relieve various maladies. Since it is mildly invasive, one must always seek the help of a professional acupuncturist to perform this procedure to avoid any accidents or injuries.
Acupuncture was reported to be effective particularly in the reduction of nasal congestion signs and symptoms with improvement in the quality of life. (17) Research suggests that acupuncture exerts anti-inflammatory effects to prevent the development of allergic rhinitis. (18)
Measures to Avoid Allergens

Since allergic rhinitis flares up upon exposure to allergens, it is important to follow certain preventive measures to avoid these triggers.
- Refrain from touching or rubbing your nose or eyes.
- Keep your hands clean and wash them with soap and water.
- Use a vacuum filter when vacuuming.
- Use a dehumidifier to lower the humidity levels indoors. Alternatively, avoid the use of humidifiers.
- Use hot water and detergent to wash your bedsheets and pillowcases.
- Avoid opening your windows during high-pollen and mold seasons. Instead, use air conditioners.
- Bathe your pets at regular intervals and maintain a hygiene routine. Restrict them from entering the bedroom to avoid pet dander.
- When going outside, wear a wide-brimmed hat and sunglasses to prevent pollen from entering your eyes.
- Use dust-mite proof covers for duvets, comforters, pillows, box springs, and mattresses.
- Cover your nose and mouth when working with wheat flour as it may trigger baker’s asthma. An allergy to wheat flour dust can induce allergic rhinitis and asthma symptoms as well. However, wheat in food forms isn’t problematic. Inhaling wheat flour, rye, or soya might trigger the condition.
Avoid other triggers that may aggravate the condition, including:
- Humidity
- Cold temperatures
- Wind
- Tobacco or wood smoke
- Chemical fumes
- Aerosol sprays
- Areas with high air pollution
- Strong fragrances such as perfumes or air fresheners
The following measures may aid recovery:
- Consume a diet rich in complex carbohydrates and low in fat.
- Drink plenty of water to maintain body hydration.
- Refrain from consuming alcohol, dairy products, and caffeine for some days.
- Change your clothes after coming from outside to avoid allergens.
Most-Asked Questions About Allergic Rhinitis

Are sinusitis and allergic rhinitis associated with each other?
Allergic rhinitis can cause a blockage in the sinuses resulting in fluid accumulation, which acts as a breeding ground for germs. The ensuing infection triggers inflammation in the sinus lining, which is referred to as sinusitis.
Is allergic rhinitis common during pregnancy?
Allergic rhinitis is a common ailment that may occur even before pregnancy and may improve, aggravate, or remain the same during this period. However, a few women may develop allergic rhinitis during pregnancy purely as a matter of coincidence. (19)
Does vitamin D play a role in allergic rhinitis?
Some clinical studies suggest that low vitamin D levels in the serum may increase the risk of developing allergic rhinitis, but others have produced conflicting results. (20)
It is also thought that gender and age may play a role in determining this relationship. Further studies are needed to conclusively establish this connection.
Are viral infections associated with allergic rhinitis?
Viral infections are common reasons for inflammation of the airways that is known as viral rhinitis. Viral and allergic rhinitis may influence each other’s onset. According to recent studies, viral infections can prevent allergy development or aggravate clinical symptoms of allergic rhinitis. (21)
Why do allergy symptoms worsen at night?
The symptoms can worsen at night due to the presence of indoor allergens, such as pet dander, pollen, and dust mites, especially on your bedding. (22)
Final Word
Allergic rhinitis is a lifelong condition that can only be managed but not cured. Living with this respiratory illness can take a toll on your daily life in the absence of proper treatment.
While allergic rhinitis is chiefly treated with medications, parallel therapies using natural products as well as body and mind practices are also available. These pharmacological and non-pharmacological interventions provide symptomatic relief from allergic rhinitis rather than treat the condition itself.

- Was this article helpful?
- YES, THANKS!NOT REALLY


